 July
07
July
07
Tags
The Forgotten:
Image source: “New Awakenings: The Legacy & Future of Encephalitis Lethargica (EL)” (Sparacin 2012)
Some call it “the sleepy-sickness”, others encephalitis lethargica. This mysterious disease, lost to time, bears its colloquial name because those who contracted it entered an “all-enveloping trancelike sleep” (1); and some of those who entered this sleep, did not awake for decades. They had been said to possibly be fully conscious and aware, but not awake–motionless, speechless–all day. Of those not completely incapacitated, symptoms such as rigidity of movement and tremors appeared. But there was a different side to this illness as well, however.
However, contrary to its name, the victims of this “sleepy sickness” also first showed a great degree of excitement of “body and soul”, the likes of which resembled Tourette’s Syndrome: frantic, violent movements and tics, and “compulsions of all kinds”, as described by Dr. Sacks (1). But the commonalities between encephalitis lethargica (EL) and Tourette’s Syndrome (TS) do not end there. In his book, “The Man Who Mistook His Wife for a Hat”, Dr. Oliver Sacks called these two diseases, among others, “diseases of excess”.
Encephalitis lethargica
Symptoms
In most of the literature describing encephalitis lethargica, there are two “phases”: acute and chronic (7). These two phases can be described separately but, as Leslie Hoffman and Joel Vilensky (7) illustrate, “the two often blended together.” The acute phase was characterized by “excessive sleepiness, disorders of ocular motility, fever, and movement disorders”, and “presented as a gradual onset of non-descript flu-like symptoms” (7). In contrast, the chronic phase included symptoms such as rigidity of movement, abnormalities in eye movements, involuntary movements, difficulties with speech and breathing, and some psychiatric disorders. However, as Sacks described, we do not see widespread descriptions of the psychiatric side of this disease, which are the “excesses” of this forgotten disease, because neurology has yet to recognize that the excess of a function means anything is wrong. Sacks himself worked with some of the patients and did more than just clinically describe their pathology. Rather, he gave narrative accounts, and described the psychiatric manifestations of their disease before they went into a deep sleep: changes in mood, feelings of euphoria, increased sexual drive, hallucinations, excessive puns, joviality, and silliness, as well as psychosis present in about 30% of patients (7). Dr. Sacks considered these symptoms to be reminiscent of Tourette’s Syndrome, a disorder that makes its victims move uncontrollably, jerking violently, sometimes yelling without a desire to. This is another disease that Sacks described as a “disease of excess”. The similarity of EL and TS arises most strikingly in one symptom: tics, which are defined as involuntary movements, actions, or behaviors carried out by the afflicted individual that seem to be excessive.
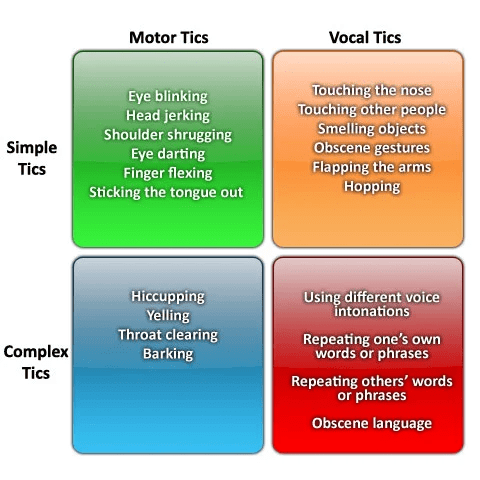
Tics
Most of the medical and scientific literature regarding EL describes it as a flu-like illness that turns into a disease of excessive sleepiness (7). However, other symptoms which Sacks presented as occurring earlier on in the progression of the sickness — such as the feelings of euphoria and tics – seem to be characteristic of TS. As described by a patient of Dr. Sacks, TS is a disease that almost makes you feel “too well”: you don’t feel sick in the traditional sense, but you are so euphoric and energetic that sometimes it becomes a burden.
As it so happens, both EL and TS share a unique disorder: dysfunction in a region of the brain known as the basal ganglia (3: Berardelli 2003). The basal ganglia is a collection of many structures that, in one aspect, deals with decision-making and actions. Thus, it may almost seem intuitive why the basal ganglia would be the location affected to produce the tics–involuntary movements or actions– characteristic of these two disorders, as well as others. Despite their similarities, the two disorders do have differentiation in their pathologies which explain why they are unique.
In encephalitis lethargica, studies found inflammation and other signs of infection in many regions of the brain. Some abnormalities in these regions can explain the latent, sleepy period of the disease, such as the pons, which has been found to play a role in alertness. Their rigidity of movement and tremors are explained specifically by the alterations in the substantia nigra (a structure we will come back to in the next section) (7). This why we see similarities between EL and Parkison’s disease.
In contrast, in the brains of patients with Tourette’s, although there is dysfunction in the basal ganglia as well–a commonality between EL and TS that may explain tics (Berardelli 2003)–many other regions were
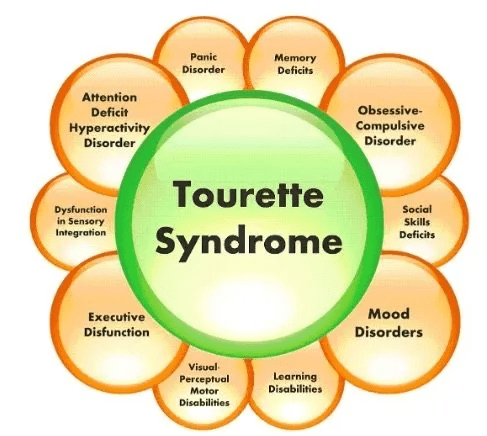
also studied and shown to have different structure and function from healthy brains (4, Table 1). This includes altered structures in regions associated with sensorimotor functioning, memory, and emotional regulation, which may explain learning disabilities, sensory processing difficulties, and behavioral issues associated with TS (2). Taken together, these studies on the brains of patients with EL and TS suggest that damage to the basal ganglia result in the behavioral tics found in both diseases. However, the origin of these tics may not rest in the morphology of those structures, but rather the amount of dopamine found in them (8; 9).
Dopamine and Movement
Dopamine is a neurotransmitter that has many roles in the brain and performs different functions depending on where it is present. There are two key functions of dopamine: as a chemical that brings us pleasure and rewards us, and as a chemical that aids in our movements. Structures that control the release of dopamine as a reward are a collection known as the mesolimbic pathway. These structures are flooded with dopamine when something pleasurable occurs and is a key component in our understanding of addiction. The other important pathway, the nigrostriatal pathway, gets its name from the two major structures that comprise the pathway: the substantia nigra and the striatum.
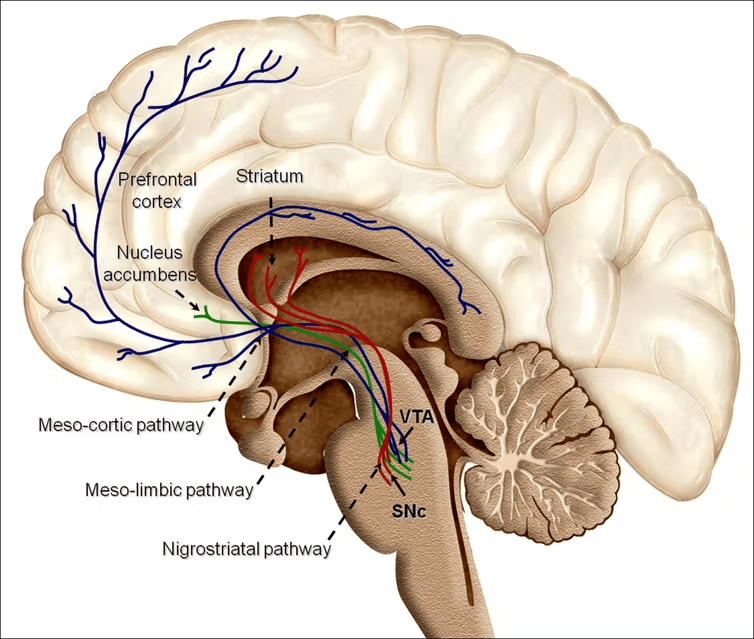
The nigrostriatal pathway is an important pathway for movement and routines. While the striatum controls our movements more directly, the substantia nigra in specific contributes to the fluidity of our movement and fine motor skills by sending dopaminergic signals to the striatum to regulate it. The substantia nigra is affected in Parkinson’s disease by the degeneration of dopaminergic neurons, and this is why those with Parkinson’s show rigidity in their movements, rather than a complete halt to movement. It as well has been found to be affected in EL, and that is why there are also symptoms of rigidity and a coma-like state in EL.
Tying back to the two disorders we are discussing, one structure we just discussed, the striatum, happens to be a structure within the basal ganglia; and, as we stated earlier, basal ganglia dysfunction is a key component of both of these ailments. Because it is structures in the basal ganglia that control movement, especially the striatum, dysfunction here can have an impact directly on what we do. However, in the case of EL and TS, this may not be due to a defect in the basal ganglia’s structures themselves. Rather, we may see similarities in EL and TS because of a dysfunction in how dopamine interacts with these structures, rather than abnormalities in the structures themselves. With all their similarities, the differences between TS and EL give us a clue into dopamine’s role in the control of movements, including the disparate reactions we see to a drug used to treat them: levodopa, also known as L-Dopa.
Treatment with Levodopa
L-Dopa is an amino acid in our bodies that is a precursor to dopamine–which means it will become the dopamine molecule. Drugs supplementing L-Dopa were first developed to try to control the consequences of Parkinson’s disease, by increasing the amount of dopamine in the brain, since Parkinson’s destroys so many of the vital dopamine-producing neurons in the brain. L-Dopa is used, rather than the neurotransmitter dopamine itself, because dopamine supplements cannot cross the blood-brain barrier, the “barrier” that keeps toxins and pathogens out of your brain’s blood supply.
In six adult patients with TS who were treated with levodopa supplements, one study found that both self-reported and videotaped tic severity decreased (5). In similar fashion, one TS patient seen by Sacks, after given a minute dose of an L-Dopa medication (Haldol), “now found himself tic-free, but without significant ill effects”.
In patients with EL, one region of the brain affected is the substantia nigra: a powerhouse for dopamine production in the midbrain. The Parkinsonian symptoms shown in postencephalitic patients is thus clearly described by this alteration, since it is the same thing that happens in Parkinson’s Disease. When dopamine is reintroduced to the brains of the patients in a trance, as Dr. Sacks described, “[t]hey were transformed by it”: awakened, excited, and displaying Tourette-like symptoms, such as the famed tics. This suggests that it is not simply an excess of dopamine that causes tics and other Tourette-like symptoms (as once thought) but rather the different interactions dopamine has in the brain, as shown by comparing both the case studies presented by Oliver Sacks and the study conducted by Black and Mink (5). The emergence of tics in patients with encephalitis lethargic and the reduction of tics in those with TS, both by administration of levodopa, again leads us to ponder what dopamine’s relationship to our movements is.
Both these diseases–these diseases of excess–seem to give us a clue into how our brain not only lacks capabilities when altered, but can also give us something new. As Dr, Sacks described it: an extravagance, a new life. The notion of being “too well”.
References
1) Sacks, O. (1985). The man who mistook his wife for a hat and other clinical tales. New York: Summit Books.
2) (2021) Tourette Syndrome Fact Sheet. National Institute of Neurological Disorders and Stroke, National Institutes of Health. https://www.ninds.nih.gov/health-information/patient-caregiver-education/fact-sheets/tourette-syndrome-fact-sheet
3) Badenoch, J., Searle, T., Watson, I., & Cavanna, A. E. (2021). Tics in patients with encephalitis. Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology, 42(4), 1311–1323. https://doi.org/10.1007/s10072-021-05065-w
4) Felling, R. J., & Singer, H. S. (2011). Neurobiology of tourette syndrome: current status and need for further investigation. The Journal of neuroscience : the official journal of the Society for Neuroscience, 31(35), 12387–12395. https://doi.org/10.1523/JNEUROSCI.0150-11.2011
5) Black, K.J. and Mink, J.W. (2000), Response to levodopa challenge in Tourette syndrome. Mov. Disord., 15: 1194-1198. https://doi.org/10.1002/1531-8257(200011)15:6<1194::AID-MDS1019>3.0.CO;2-H
6) Dryden, J. (2002), Brain activity changes in Tourette syndrome. The Source, Washington University in St Louis. https://source.wustl.edu/2002/01/brain-activity-changes-in-tourette-syndrome/
7) Hoffman, L. A., & Vilensky, J. A. (2017). Encephalitis lethargica: 100 years after the epidemic. Brain : a journal of neurology, 140(8), 2246–2251. https://doi.org/10.1093/brain/awx177
8) Caligiore, D., Mannella, F., Arbib, M. A., & Baldassarre, G. (2017). Dysfunctions of the basal ganglia-cerebellar-thalamo-cortical system produce motor tics in Tourette syndrome. PLoS computational biology, 13(3), e1005395. https://doi.org/10.1371/journal.pcbi.1005395
9) Black, K. J., Piccirillo, M. L., Koller, J. M., Hseih, T., Wang, L., Mintun, M. A. (2013), PeerJPrePrints. https://www.researchgate.net/publication/344991131_Levodopa-stimulated_dopamine_release_in_Tourette_syndrome
10) Sparacino, D. (2012), New Awakenings: The Legacy & Future of Encephalitis Lethargica (EL). rn.com, AMN Healthcar Education Services. https://www.rn.com/nursing-news/new-awakenings-encephalitis-lethargica/#:~:text=Originally%20developed%20to%20treat%20Parkinson’s,Parkinson’s%20(NYT%2C%202011)

You must be logged in to post a comment.