 April
20
April
20
Tags
This is your brain on drugs: how cannabis products affect the brain and body
Into the weeds
Pot. Mary Jane. Grass. The Devil’s Lettuce. Weed. Most people have heard of cannabis and are aware of the general effects that may result from ingesting it – but fewer people appear to know the mechanisms of action underlying those experiences. Moreover, there is a significant difference between cannabis and marijuana and the way each of those substances are utilized – perhaps the line is muddied by the myriad of nicknames used for cannabis and its derivatives. Cannabis is, first and foremost, a plant. Cannabis contains more than one hundred different substances called cannabinoids, the most well-known of which are THC (Δ-9-tetrahydrocannabinol) and CBD (cannabidiol) (Ng & Gupta, 2023; Schilling et al., 2020). It is important to note that not every strain of the Cannabis plant contains the same amounts of cannabinoids. This variety results in a wide variety of strains with diverse effects on the body and mind following ingestion or topical application. Marijuana, then, is just one subset of these many strains of Cannabis, characterized by its high levels of THC and low levels of other cannabinoids such as CBD. Conversely, other Cannabis products such as hemp lack THC and other cannabinoids almost completely (Schilling et al., 2020). This is why hemp is commonly used to produce twine and other types of string – if you ingest hemp, you will certainly not feel any psychoactive effects, but its high tensile strength makes it a reliable component for the ropes that fasten and secure many everyday objects (Lilley, 2022). In this article, we will take some time to learn about Cannabis and how it interacts with your brain and body not only recreationally, but also in medical settings.
Cool cannabinoids
Cannabinoids each act on innate receptors in the body known as endogenous cannabinoid receptors. There are two main types of cannabinoid receptors, aptly named cannabinoid receptor-1 (CBR-1) and -2 (CBR-2) (Zou & Kumar, 2018). These CBRs are G-protein coupled receptors, a type of receptor that requires a ligand to bind at the membrane (a ligand is a specific type of binding agent with a particular affinity to each receptor subtype). Once bound, it triggers a change in the shape of the receptor, which leads to downstream changes of signals within the cell (Rogers, 2023). In the brain, this means an alteration of neural activity (Manzanares et al., 2006). Neurotransmitters are brain chemicals that influence the activity of cells (for example, GABA is an inhibitory neurotransmitter that tells a cell to stop firing). Cannabinoids can act like neurotransmitters to influence neurons and other cells in the body to behave differently. In the case of CBRs, this means that the binding of cannabinoid ligands, such as THC, are triggering a specific reaction in the cell that is unique to the ligand. This receptor interaction is what produces the side effects associated with different products of Cannabis; when you take CBD, you may feel resulting pain relief from its interactions with CBRs, whereas ingesting its psychoactive relative THC will lead to experiences typically associated with intake of marijuana – feeling “high”.
Nifty neurotransmission
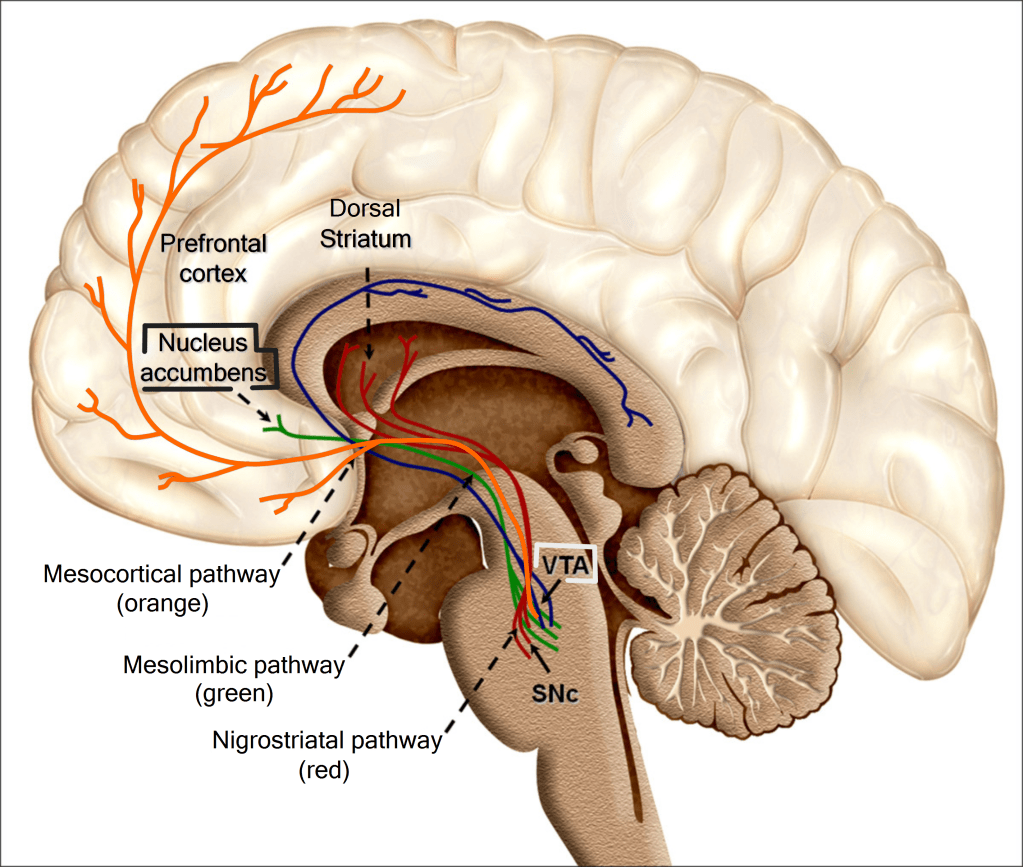
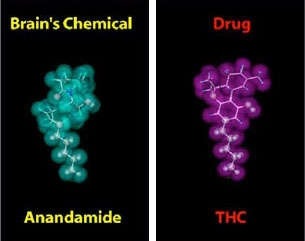
Another neurotransmitter you have undoubtedly heard of is dopamine. This endogenous (made within the brain) chemical is tied to the brain’s reward system; dopamine activity is correlated with pleasurable feelings. Briefly, the brain’s reward system has a few major players: the ventral tegmental area (VTA) and the nucleus accumbens (NAc) (Lupica et al., 2004). Within the VTA, there are many neurons that are responsible for the transmission of dopamine to the NAc, which is often referred to as the reward center of the brain because of this dopaminergic input. After signals are transmitted to the NAc, they are then relayed to the part of the brain called the frontal cortex, where they are processed (Figure 1, Arias-Carrion et al., 2010) There are also many GABAergic, or inhibitory, neurons that project from VTA that may play a role in dampening the activity of dopaminergic neurons. These projections are part of the mesolimbic pathway, one of the major roads for the transmission of reward signaling in the brain (Lupica et al., 2004; U.S. Department of Health and Human Services, 2016). This pathway is important for reinforcement of reward-related learning and motivation, behaviors that are indeed influenced by dopamine signaling (Malenka et al., 2009). When THC is introduced to the brain, it directly modulates this pathway by altering inhibitory signaling. Inhibitory neurons between VTA and NAc – which make connections with NAc and neighboring dopaminergic neurons – contain cannabinoid receptors which are compatible with THC. THC is strikingly similar in composition to Anandamide, an endogenous cannabinoid that acts on CBR-1s (Figure 2, U.S. Department of Health and Human Services, 2021). Due to this structural similarity, THC is also able to act upon CBR-1s on these inhibitory neurons in the mesolimbic pathway. Thus, when THC is present in the brain, it competes with endogenous cannabinoids like Anandamide to bind on CBR-1s. In doing so, THC leads to a decrease in inhibitory activity onto dopaminergic neurons, thereby increasing the flow of dopamine. This increase in dopamine level is what leads to the “high” that users experience after ingesting THC. To see an animation of this phenomenon, check out the video below:
The Reward Circuit: How the Brain Responds to Marijuana
Clinical cannabidiol
The way different cannabinoids influence cellular activity in the body is not only dependent on which type of receptor (CBR) they interact with, but also the distribution of those receptors in the body and the route of administration of the cannabinoid-containing substance. Interestingly, CBR-1s are the most prominently expressed receptor subtype of the GPCR family in the brain (Zou & Kumar, 2018). CBR-1 is also expressed in other areas of the body, but CBR-2s are more prominent in the peripheral nervous system (Eskander et al., 2020). CBR expression across different regions of the body is partially responsible and necessary for the effects of topical CBD on your aching lower back. In fact, there are CBR-2 receptors right in the skin that CBD binds to to exercise its effects (Baswan et al., 2020). CBD has gained acclaim in the past decade for its calming and analgesic properties, but the research being done to understand the mechanisms underlying those claims has not always been communicated clearly and thoroughly. In recent years, research done in both animal models and in human clinical trials has begun to shed more light on the effects and clinical potential of CBD.
Historically, research has uncovered that CBD may be exercising its analgesic effect on non-CBRs in the brain and body, including multiple membrane channels tightly involved in pain signaling pathways. The relevant pathways each involve a brain region called the periaqueductal gray (PAG). Using rats as a model, researchers have studied the effects of CBD on pain sensation by introducing it directly to the PAG. It was shown that rats receiving CBD displayed decreased pain related behavior, indicative of antinociceptive (anti-pain) action (Maione et al., 2011). These additional targets for CBD were an important advancement in this field of work, revealing additional targets for pain intervention and novel treatments.
In two case studies of chronic back pain, adults given transdermal CBD cream each reported significant improvement of their symptoms (Eskander et al., 2020). Transdermal creams are seemingly highly varied due to private companies’ proprietary preparations, but the efficacy of general samples has previously been validated in animal models that measured the amount of CBD present in the muscle following topical application. In one of the case studies, researchers followed a patient with a past lumbar spinal fusion who sustained a lumbar spine compression fracture after a fall. Despite this significant history of lumbar spinal issues and pain he initially reported as 8/10 in severity, transdermal CBD applications were able to lower his perceived pain level to a 1-2/10 (Eskander et al., 2020). Remarkably, after just 4 weeks of CBD, he was able to cease treatment. In light of the ongoing opioid crisis (check out this NeuWrite article to learn more), it is particularly appealing to consider other non-addictive compounds that may help to treat clinical pain and decrease the amount of opioid prescriptions doctors must distribute.
Finally, it is interesting to note that CBD has clinical potential that reaches far beyond pain management. It has also been shown that systemic CBD administration was sufficient to reduce the frequency of seizures in multiple mouse and rat models (Patra et al., 2018). The potential of CBD to ameliorate seizure and related symptoms was further explored in this study by delivering CBD orally and by switching to chronic dosing. In doing so, they found that additional seizure models were protected against negative outcomes and symptoms, and following chronic administration, this included memory errors in a model of epilepsy.
Changing perspectives
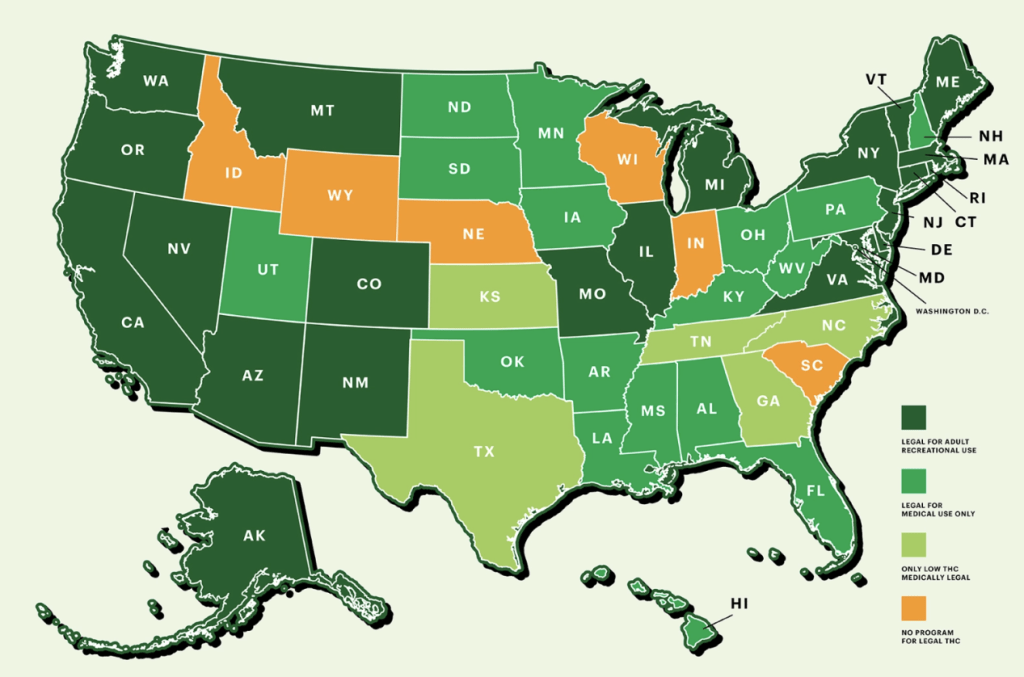
Altogether, it seems that Cannabis and its derivative products have great potential in both treating human health and for safe recreational use. Unfortunately, research into these avenues is lagging behind many other neuroscientific fields due to tight governmental restrictions and regulations. In fact, marijuana is only legalized for recreational use in certain states, with other states allowing only medical use, and even more banning all but CBD products lacking THC (Figure 3). Despite this steadily increasing legalization in several states, marijuana and other Cannabis-derived products are still often overlooked as legitimate clinical interventions. In addition, there is still a great deal of stigma surrounding its use. Worst of all, many in the United States remain incarcerated for possession of marijuana while thousands enjoy its safe and legal use every day, in spite of the decriminalization of small amounts of marijuana in 27 states and DC (Hartman, 2022; Oleck, 2020). Finally, I would be remiss not to acknowledge that Black people have historically been disproportionately arrested and penalized for possession of small amounts of marijuana (American Civil Liberties Union, 2023; Oleck, 2020). With better education about how Cannabis products interact with the body, plus the advocacy work and scientific research being conducted all over the world, we can continue to demystify Cannabis and its potential for safe recreational and clinical use.
Sources
American Civil Liberties Union. (2023). Marijuana arrests by the numbers. American Civil Liberties Union. Retrieved April 18, 2023, from https://www.aclu.org/gallery/marijuana-arrests-numbers
Arias-Carrión, O., Stamelou, M., Murillo-Rodríguez, E., Menéndez-González, M., & Pöppel, E. (2010). Dopaminergic reward system: A short integrative review. International Archives of Medicine, 3(1), 24. https://doi.org/10.1186/1755-7682-3-24
Baswan, S. M., Klosner, A. E., Glynn, K., Rajgopal, A., Malik, K., Yim, S., & Stern, N. (2020). Therapeutic potential of cannabidiol (CBD) for skin health and disorders. Clinical, Cosmetic and Investigational Dermatology, 13(2020), 927–942. https://doi.org/10.2147/ccid.s286411
Eskander, MD, MBA, J. P., Spall, BS, J., Spall, BA, A., Shah, MD, MBA, R. V., & Kaye, MD, PhD, A. D. (2020). Cannabidiol (CBD) as a treatment of acute and chronic back pain: A case series and literature review. Journal of Opioid Management, 16(3), 215–218. https://doi.org/10.5055/jom.2020.0570
Hartman, M. (2022, May 31). Report cannabis overview. National Conference of State Legislatures. Retrieved April 18, 2023, from https://www.ncsl.org/civil-and-criminal-justice/cannabis-overview
Lilley, A. (2022, October 6). Hemp rope – features, benefits and uses. R&W Rope. Retrieved April 14, 2023, from https://rwrope.com/blogs/news/hemp-rope-features-benefits-and-uses#:~:text=Hemp%20rope%20has%20very%20high,%2C%20weight%20loading%2C%20and%20more.
Maione, S., Piscitelli, F., Gatta, L., Vita, D., De Petrocellis, L., Palazzo, E., de Novellis, V., & Di Marzo, V. (2011). Non-psychoactive cannabinoids modulate the descending pathway of antinociception in anaesthetized rats through several mechanisms of action. British Journal of Pharmacology, 162(3), 584–596. https://doi.org/10.1111/j.1476-5381.2010.01063.x
Malenka RC, Nestler EJ, Hyman SE (2009). Sydor A, Brown RY (eds.). Molecular Neuropharmacology: A Foundation for Clinical Neuroscience (2nd ed.). New York: McGraw-Hill Medical. pp. 147–148, 367, 376.
Manzanares, J., Julian, M., & Carrascosa, A. (2006). Role of the cannabinoid system in pain control and therapeutic implications for the management of acute and chronic pain episodes. Current Neuropharmacology, 4(3), 239–257. https://doi.org/10.2174/157015906778019527
Ng, T., & Gupta, V. (2023). Tetrahydrocannabinol (THC). In StatPearls. https://www.ncbi.nlm.nih.gov/pubmed/33085321
Oleck, J. (2020, June 26). With 40,000 Americans incarcerated for marijuana offenses, the cannabis industry needs to step up, activists said this week. Forbes. Retrieved April 18, 2023, from https://www.forbes.com/sites/joanoleck/2020/06/26/with-40000-americans-incarcerated-for-marijuana-offenses-the-cannabis-industry-needs-to-step-up-activists-said-this-week/?sh=24c479a0c16f
Patra, P. H., Barker‐Haliski, M., White, H. S., Whalley, B. J., Glyn, S., Sandhu, H., Jones, N., Bazelot, M., Williams, C. M., & McNeish, A. J. (2018). Cannabidiol reduces seizures and associated behavioral comorbidities in a range of animal seizure and epilepsy models. Epilepsia, 60(2), 303–314. https://doi.org/10.1111/epi.14629
Rogers, K. (2023, March 20). G protein-coupled receptor. Encyclopædia Britannica. Retrieved April 12, 2023, from https://www.britannica.com/science/G-protein-coupled-receptor
Schilling, S., Melzer, R., & McCabe, P. F. (2020). Cannabis sativa. Curr Biol, 30(1), R8-R9. https://doi.org/10.1016/j.cub.2019.10.039
U.S. Department of Health and Human Services. (2016). The reward circuit: How the brain responds to marijuana. National Institutes of Health. Retrieved April 12, 2023, from https://nida.nih.gov/videos/reward-circuit-how-brain-responds-to-marijuana#:~:text=There%2C%20THC%20competes%20with%20the,neurons%20to%20release%20more%20dopamine.
U.S. Department of Health and Human Services. (2021, April 13). How does marijuana produce its effects? National Institutes of Health. Retrieved April 12, 2023, from https://nida.nih.gov/publications/research-reports/marijuana/how-does-marijuana-produce-its-effects
Zou, S., & Kumar, U. (2018). Cannabinoid Receptors and the Endocannabinoid System: Signaling and Function in the Central Nervous System. Int J Mol Sci, 19(3). https://doi.org/10.3390/ijms19030833


Pingback: Chasing a Runner’s High | NeuWrite San Diego
Pingback: Solving the Puzzle of Addiction | NeuWrite San Diego