 July
14
July
14
Tags
#TriggerWarning: Life After Trauma
At 2:09 am on June 12, 2016, Pulse had a message for its patrons:

via Facebook
It’s only eight words, but it gives me chills whenever I read it. Have you ever been anywhere and found yourself with that imperative? Run. Keep running. Or you may die.
The shooting at the Pulse nightclub in Orlando claimed the lives of 50 people and injured 53 others. For most of the country, that incident is now over, and in its wake the media is fraught with debate over gun control, homophobia, and terrorism. For the 53 injured, over 300 other survivors in the club, and the first responders to the scene, however, the Orlando shooting isn’t yet another shooting for US history books. That chilling life-or-death imperative was forced upon them, and now they face the formidable task of moving on. For them, this is far from over.
While everyone copes with traumatic events differently, there are certain reactions that we share as a species. For instance, we evolved a “fight-or-flight” response that is designed to get us out of dangerous situations alive. We become more alert, our heart rates rise, and our bodies direct all available resources to the systems that will need it most. It’s helpful in a pinch, but this state of hyperarousal is stressful to the body and distressing to the individual. If the danger persisted, we would benefit from being on constant alert all of the time. Since this is not the case, there is an equally important second component to the “flight-or-flight” response, and that entails bringing the body back to normal.
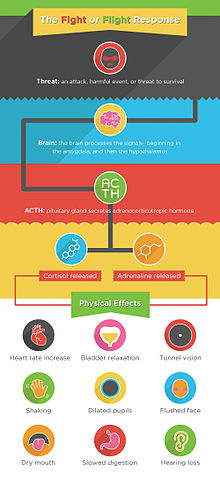
via Wikipedia
Coping with trauma can be a lengthy, difficult process for anyone. For some, however, that process crosses into the territory of Post-Traumatic Stress Disorder (PTSD). Like other mental illnesses, PTSD can be viewed as an extension of normal behaviors. It is natural to become on edge when you sense a threat, or to avoid dangerous situations when you can predict them. PTSD sufferers have these same reactions, but they have become overgeneralized to scenarios that do not warrant a “fight-or-flight” reaction. Often this occurs in the form of a “re-experiencing” symptom. According to the National Institute of Mental Health (NIMH), this can take the form of nightmares, frightening thoughts, or full-blown flashbacks, in which the body physically behaves as though you’ve entered a “fight-or-flight” situation.[1] In this case of a survivor of the Orlando shooting, for example, the person’s heart may begin to race and panic may set in after a car backfires. That backfiring sound, while not identical to a gunshot, becomes a trigger for PTSD symptoms given its relative similarity to the sound of a gun. Other symptoms of PTSD include avoidance of places or things that contain triggers, hyperreactivity, and changes in mood or cognition. To keep with the example of a survivor of the Orlando shooting, these symptoms could manifest as an avoidance of bars or other social settings; difficulty sleeping or heightened startling reactions; and depression or other negative feelings with regard his or her LGBTQ identity, given the homophobic context of the incident. PTSD may dissipate in a matter of months, but could also affect the individual for a substantially longer time period. Regardless of the specific manifestation, at least one month of PTSD symptoms is required for diagnosis.
PTSD used to be a condition primarily associated with war veterans. You may have heard the phrase “shell shock” in relation to soldiers; this refers to a condition that would later be recognized as PTSD. To this day, veterans remain among the most commonly afflicted by the condition. Although many soldiers will endure horrific experiences that most civilians would be hard-pressed to imagine, they do not all go on to develop PTSD. Importantly, those who do develop PTSD are not necessarily the ones who had been through the most trauma (if such a thing can be accurately and objectively quantified). Instead, this observation taught us that we are not all at equal risk to develop PTSD; trauma may be required to trigger it, but some are predisposed to develop the condition.
A now classic study by Gilbertson and colleagues examined differences in the brains of Vietnam War veterans, some of whom had developed PTSD and some who had not.[2] The study also took advantage of a natural genetic control group – identical twins of the veterans who had not gone to war themselves. The study identified two key findings related to the hippocampus, the region of the brain most heavily associated with memory formation. First, veterans with severe PTSD had smaller hippocampal volumes when compared to both veterans without PTSD as well as their own twins. This may indicate that traumatic experiences can have a toxic effect on the hippocampus, ultimately shrinking the region. It is important to note, however, that this is a correlation, and as the saying goes, correlation does not prove causation. With that in mind, the second major finding of the study is especially compelling; twins of PTSD sufferers who had not been to war also had smaller hippocampal volumes when compared to the non-PTSD veterans and siblings. These siblings had not undergone any trauma that could explain these differences. Thus, the smaller hippocampus seen in PTSD sufferers may not necessarily be the toxic result of trauma, but a pre-existing risk factor that could predict whether or not the person is likely to develop PTSD.

From Gilbertson et al. (2002). The colored regions represent the two sides of the hippocampus. The comparisons are as follows: (a) These brains belong to two unrelated veterans. The veteran on the left has PTSD, and the one on the right does not. The hippocampus in the PTSD patient (left) is smaller. (b) These brains belong to twins. The twin in the top image is a veteran with PTSD, and the one in the bottom image has never been to war. The hippocampus in the twin with PTSD (top) is smaller. (c) These brains belong to the combat-unexposed twins of unrelated veterans. The twin on the left’s sibling has PTSD, and the one on the right’s does not. The hippocampus in the twin whose sibling has PTSD (left) is smaller.
Of course, PTSD is not a condition reserved for veterans of war. Anyone can develop PTSD following a traumatic event, be it a shooting, sexual assault, disaster, or any other event in which there is an imminent sense of a threat to one’s life. The National Center for PTSD estimates that approximately 8 in 100 people will experience PTSD, with the prevalence somewhat higher in women than men. Importantly, PTSD can also develop following traumatic experiences that are not threatening to the individual; first responders (who can of course find themselves in life-threatening situations) are at an elevated risk to develop PTSD, given their frequent exposure to horrific sights and situations. PTSD can also develop following a sudden tragic event such as the unexpected loss of a loved one.
In the case of the Orlando shooting, there is concern that PTSD and related anxiety conditions will manifest beyond those individuals directly involved to the LGBTQ community at large. This is a community that is already at higher risk to be the victims of hate crimes and discrimination, through no fault of their own. In the words of President Obama, Pulse is “a place of solidarity and empowerment where people have come together to raise awareness, to speak their minds, and to advocate for their civil rights.” Pulse and places like it have become areas of refuge for people who may not be able to freely express themselves in daily life. Now that Pulse has become the site of the deadliest mass shooting in our nation’s history, members of the LGBTQ community find themselves with shaken confidence that there is anywhere they can truly be safe, to relax without worry, even during Pride Month.
Inspiring displays of pride and solidarity have followed in the wake of this tragedy, from members of the LGBTQ community and allies alike. Coming together like this is incredibly important to mitigate the long-term impact of traumatic events. People are significantly less likely to develop PTSD when they are able to seek help and support from friends, families, and support groups. Likewise, seeking the support of a therapist that specializes in exposure therapies and/or cognitive behavioral therapy has demonstrated relative efficacy in treating PTSD. While medications can be used to help trauma victims cope, there is no clear consensus regarding the most effective drugs to treat PTSD. In fact, drugs classically used to treat acute anxiety, including benzodiazepines such as Valium or Xanax, have not only been ineffective at treating PTSD, but when they are administered following trauma, some evidence suggests that the resulting PTSD symptoms are even worse.[3]
The current atmosphere in our country is especially volatile. So far in 2016, there have been over 180 mass shootings.[4] Race relations have continued to deteriorate in the wake of the murders of #AltonSterling and #PhilandoCastile.[5] The LGBTQ community remains threatened by both violence and discriminatory legislation. Not to mention we are currently in the midst of a particularly divisive presidential election. Until we can begin to mend the roots of our heartbreak, it is imperative that we support each other in the wake of such trauma. Remember that everyone copes differently, and that some of us may need a little extra help bouncing back from tragedy. We can come together and heal, or isolate and feed the fear. It’s our choice.

References
[1]Post-Traumatic Stress Disorder, National Institute of Mental Health.
[2]Gilbertson, M.W., Shenton, M.E., Ciszewski, A., Kasai, K., Lasko, N.B., Orr, S.P., and Pitman, R.K. (2002). Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nat Neurosci 5(11): 1242-1247.
[3]Guina, J., Rossetter, S.R., DeRhodes, B.J., Nahhas, R.W., and Welton, R.S. (2015). Benzodiazepines for PTSD: A systematic review and meta-analysis. J Psychiatr Pract 21(4): 281-303.
[5]Race Relations are at Lowest Point in Obama Presidency, Poll Finds. New York Times.

You must be logged in to post a comment.