 November
17
November
17
Tags
Brain and Blood, Diseases and Drugs
Neuroscientists love neurons. We learn about the endless types of neurons, the distinct ways in which they send chemical signals, how they connect to each other, and how these networks underlie behavior. Most of us eat, sleep, and breathe neurons. A smaller, badass group of neuroscientists instead champions glia, the underappreciated cells in the brain now known to be essential for the development and maintenance of neurons’ health and proper signaling. While glia are finally beginning to receive the attention they deserve, neuroscientists still forget that there’s anything else in the brain besides the neurons and glia, hence I always like to start talking about my work by showing this picture:

That is a cast of the blood vessels brain. Boom. Mind blown.
Yes, blood vessels look cool. And blood is important for bringing oxygen and nutrients to every tissue in the body. But why should neuroscientists care?
The blood vessels in the brain and spinal cord are actually quite different from blood vessels in the rest of the body. The vessels create a barrier between the blood and the brain tissue—we call it the blood-brain barrier, or BBB for short [1-4]. The BBB is important for two main reasons. One is to prevent toxins and pathogens from getting into the brain. Neurons that get sick and die are not able to regenerate the way that other cells in the body do (e.g., skin cells), and damaging neural networks can severely affect a person’s thoughts and behavior. The other reason that the BBB is important is that it maintains tight control over the levels of certain ions and molecules in the brain. Brain cells talk to each other via electrical and chemical signals, so the fluid around the neurons and glia has to have a very specific composition. If ions and molecules could easily flow from the blood into the brain, this perfectly balanced chemical environment would be compromised, and brain cell communication could be altered.
Unfortunately, the BBB breaks down in a range of neurological conditions including stroke, multiple sclerosis, epilepsy, and traumatic brain injury [4-6]. It’s a bit more controversial, but BBB breakdown has also been implicated in Alzheimer’s disease, Parkinson’s disease, and ALS [7-16]. In some of these cases, BBB breakdown is a consequence of the disease or injury, but in others it’s thought to be part of the cause. Either way, if we knew more about the BBB—how it breaks and how it gets repaired—we might be able to create treatments that decrease the severity of not one disease but a range of neurological conditions. So that’s why a super small group of neuroscientists (including yours truly) study blood vessels instead of neurons or glia.
The blood-brain barrier
The term “blood-brain barrier” is a bit dangerous as it elicits the image of a sturdy brick wall protecting the pristine neuronal space. And if you’re thinking of the BBB as a brick wall, when you think “BBB breakdown,” you think of that wall being shattered (cue Miley Cyrus on her wrecking ball, hitting hard in love). But the BBB is not actually a single physical entity.

The blood vessel walls are made up of cells called “endothelial cells”, and in the brain and spinal cord these endothelial cells have special qualities that together make up the barrier. Brain endothelial cells are attached to each other far more tightly (via “tight junctions”) than endothelial cells in the rest of the body, so molecules in the blood can’t squeeze between them into the brain. Additionally, in other parts of the body, there’s a lot of traffic through the endothelial cells (basically imagine little bubbles transporting things from one side of the cell, through the cell, and out the other side). In the brain and spinal cord, however, there are very few transportation bubbles. Just in case some small molecules try to diffuse unnoticed through the endothelial cells into the brain, the endothelial cells have pumps called efflux transporters to shoot them back out into the blood. Last but not least, immune cells need special receptors to get into body tissues from the blood. While these receptors are plentiful in other tissues, in the healthy brain and spinal cord, the blood vessels don’t have many of them. Because the BBB is so efficient, the brain endothelial cells need specific transporters to get important things (such as sugar for energy) into the brain.
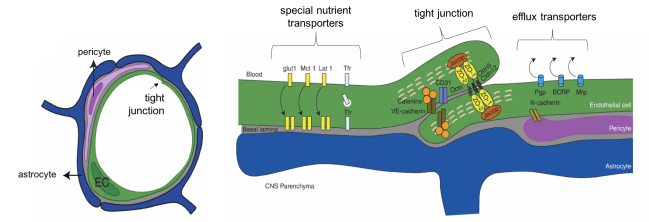
Endothelial cells (“ECs”) make up form blood vessel walls, as seen on the left. Brain ECs are surrounded by pericytes and astrocytes that help to maintain the barrier. Pictured on the right are some of the properties that make up the barrier such as tight junctions, efflux transporters, and special nutrient transporters. Image adapted from Daneman and Prat, 2015
In fact, the barrier is so effective that if you inject a healthy mouse with some blue dye, it easily seeps into every other tissue but the brain.

Various mouse organs after injection of a blue dye called Evan’s Blue. Because of the BBB, the dye does not get into the brain.

The BBB is occasionally dysfunctional (aren’t we all)
In conditions such as stroke, multiple sclerosis, epilepsy, and traumatic brain injury, the endothelial cells that make up the vessel walls lose some of their special properties. How they lose them is still not entirely clear. But the properties change. Tight junctions get cut or endothelial cells decrease their production or tight junction components. There is increased movement through the endothelial cells (think bubble transport). Endothelial cells start producing more of the receptors for immune cells. While some immune cells can be important for fighting infection, too many can cause chronic inflammation.

A mouse model of stroke. Green fluorescence signifies BBB leakage in the area of the stroke. Image taken by Kaja Bajc in the Daneman Lab
In mouse models of these diseases and injuries, there is BBB breakdown at the site of the problem. Researchers can measure breakdown by injecting the mouse with a fluorescent molecule. Because of the broken barrier, the fluorescent molecule will leak into the brain right around the region that is sick or damaged. In human patients, doctors can detect blood-brain barrier breakdown with a special type of MRI. In most cases, the BBB is eventually repaired, but exactly how it is repaired and what signals lead to this repair are still mostly unknown.
The BBB says no to drugs
While the BBB is necessary for keeping the brain safe and healthy, it also presents a huge problem for treating the brain (e.g. brain tumors, mood disorders, neurodegenerative diseases, etc.) because most drugs cannot get across the barrier. So while some neuroscientists who study the blood-brain barrier are interested in how its dysfunction changes the course of disease, others study the BBB in order to figure out how to get past it. Many strategies have been developed by scientists and drug companies throughout the years, but a good method of drug delivery is still very much a work in progress.
What are these existing strategies? One strategy is to inhibit those efflux pumps that normally make sure nothing sneaks through the endothelial cells. A drug that does this—Tariquidar—is currently in clinical trials to help get anti-cancer drugs into the brain. Another strategy is to literally break apart the endothelial cells in a very specific location so that a little bit of drug (already in the blood) can get in. This can be done in a few ways, but the most promising seems to be focused ultrasound with microbubbles—basically a person is injected with lots of super, super tiny bubbles and then low-power ultrasound is applied at a very specific spot in the brain [17-20]. The ultrasound waves make the bubbles in the blood get excited and bounce around, punching a little hole into the vessel wall. For an awesome description of this procedure, check out this Radiolab episode. This strategy is also in clinical trials to be used with cancer treatment.
Strategies that disrupt the BBB can be harmful, though, because the drug is not the only thing that ends up getting into the brain, and that perfect chemical balance can be disrupted. Many scientists are therefore working on drug delivery strategies that take advantage of BBB properties rather than trying to break the BBB. As mentioned previously, brain endothelial cells have transporters that bring very s pecific molecules into the brain from the blood. For example, one of these transporters is responsible for shuttling glucose across the barrier, another is responsible for bringing insulin in, etc. Researchers are trying to build drugs that essentially trick the transporters into letting them through. This is literally called the “Trojan horse approach.” ArmaGen, a pharmaceutical company, recently received FDA approval for a clinical trial targeting the insulin transporter to treat Hurler and Hunter syndromes.
pecific molecules into the brain from the blood. For example, one of these transporters is responsible for shuttling glucose across the barrier, another is responsible for bringing insulin in, etc. Researchers are trying to build drugs that essentially trick the transporters into letting them through. This is literally called the “Trojan horse approach.” ArmaGen, a pharmaceutical company, recently received FDA approval for a clinical trial targeting the insulin transporter to treat Hurler and Hunter syndromes.
Seeing double
There is an incredible amount that scientists have yet to uncover about the BBB, especially the cellular and molecular events that occur as it breaks down and is repaired. As we learn more about the BBB, the clinical advantages will be two-fold. First, we can reduce breakdown and hasten repair, thereby decreasing symptom severity in a range of diseases and injuries (stroke, multiple sclerosis, epilepsy, traumatic brain injury). And second, knowing more about the BBB will enable scientists and doctors to design better strategies for delivering treatment to the brain for a whole host of other conditions including brain tumors. I love neurons and glia as much as the next neuroscientist, but the BBB also deserves the spotlight once in awhile!
References
- S. M. Gloor et al., Molecular and cellular permeability control at the blood-brain barrier. Brain Research Reviews 36, 258-264 (2001).
- L. L. Rubin, J. M. Staddon, The cell biology of the blood-brain barrier. Annu Rev Neurosci 22, 11-28 (1999).
- N. R. Saunders, C. J. Ek, M. D. Habgood, K. M. Dziegielewska, Barriers in the brain: a renaissance? Trends Neurosci 31, 279-286 (2008).
- B. V. Zlokovic, The blood-brain barrier in health and chronic neurodegenerative disorders. Neuron 57, 178-201 (2008).
- J. I. Alvarez, R. Cayrol, A. Prat, Disruption of central nervous system barriers in multiple sclerosis. Biochim Biophys Acta 1812, 252-264 (2011).
- K. E. Sandoval, K. A. Witt, Blood-brain barrier tight junction permeability and ischemic stroke. Neurobiol Dis 32, 200-219 (2008).
- M. A. Erickson, W. A. Banks, Blood-brain barrier dysfunction as a cause and consequence of Alzheimer’s disease. J Cereb Blood Flow Metab 33, 1500-1513 (2013).
- M. R. Halliday et al., Accelerated pericyte degeneration and blood-brain barrier breakdown in apolipoprotein E4 carriers with Alzheimer’s disease. J Cereb Blood Flow Metab 36, 216-227 (2016).
- B. D. Zipser et al., Microvascular injury and blood-brain barrier leakage in Alzheimer’s disease. Neurobiol Aging 28, 977-986 (2007).
- M. D’Haeseleer, M. Cambron, L. Vanopdenbosch, J. De Keyser, Vascular aspects of multiple sclerosis. Lancet Neurol 10, 657-666 (2011).
- R. Cabezas et al., Astrocytic modulation of blood brain barrier: perspectives on Parkinson’s disease. Frontiers in cellular neuroscience 8, (2015).
- Y. C. Chung et al., The role of neuroinflammation on the pathogenesis of Parkinson’s disease. BMB Rep 43, 225-232 (2010).
- B. A. Faucheux, A. M. Bonnet, Y. Agid, E. C. Hirsch, Blood vessels change in the mesencephalon of patients with Parkinson’s disease. Lancet 353, 981-982 (1999).
- H. Donnenfeld, R. J. Kascsak, H. Bartfeld, Deposits of IgG and C 3 in the spinal cord and motor cortex of ALS patients. Journal of neuroimmunology, (1984).
- M. C. Evans, Y. Couch, N. Sibson, M. R. Turner, Inflammation and neurovascular changes in amyotrophic lateral sclerosis. Mol Cell Neurosci 53, 34-41 (2013).
- A. Leonardi, G. Abbruzzese, L. Arata, L. Cocito, M. Vische, Cerebrospinal fluid (CSF) findings in amyotrophic lateral sclerosis. J Neurol 231, 75-78 (1984).
- A. Burgess, K. Hynynen, Drug delivery across the blood-brain barrier using focused ultrasound. Expert Opin Drug Deliv 11, 711-721 (2014).
- K. Hynynen, Macromolecular delivery across the blood-brain barrier. Methods Mol Biol 480, 175-185 (2009).
- K. Hynynen, N. McDannold, N. A. Sheikov, F. A. Jolesz, N. Vykhodtseva, Local and reversible blood brain barrier disruption by noninvasive focused ultrasound at frequencies suitable for trans-skull sonications. Neuroimage 24, 12-20 (2005).
- K. Hynynen et al., Focal disruption of the blood-brain barrier due to 260-kHz ultrasound bursts: a method for molecular imaging and targeted drug delivery. J Neurosurg 105, 445-454 (2006).

Pingback: What’s happening in the brain with COVID-19? | NeuWrite San Diego