 May
11
May
11
Identity Crisis
Who are you? How do you know?
I’ve been thinking a lot about identity this week. It all started when I received a letter from the IRS that began “Dear TAXPAYER” and essentially asked, “Are you who you say you are?” (Yes, it’s me! Please send me my tax refund!) To validate my identity, I was given a list of legitimate forms of identification and told to choose one from Column A and one from Column B. And just like that, I’m me. So, who are you? It seems like a simple question, but when you try to break identity down into discrete variables, the difficulty becomes readily apparent. Consider the sandwich.
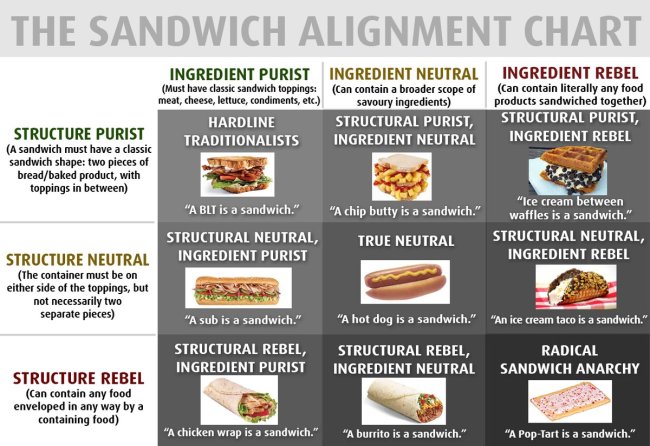
The Sandwich Alignment Chart by @matttomic
There’s an ongoing debate on the internet about whether a hot dog is a sandwich. Everyone from the National Hot Dog and Sausage Council to Meryl Streep has weighed in (and Meryl Streep seems to have a lot of experience with this sort of thing). It seems we know what a sandwich is, but at the same time are very unsure. I’d happily assign the title to a sausage sandwich, but something about calling a hot dog a sandwich seems totally wrong. And if sandwiches are this complicated, identity judgements about people must be exponentially more difficult. Let’s examine some cases where this judgement goes awry.
Mr. Sims pointed his pistol at his wife telling her that first he would shoot her and then himself. He yelled at her, “What are you doing here? Get out of my house. You are not my wife” [1].
You know that nagging feeling you get when you run into someone from your past in a new, unexpected location? You rack your brain, scanning through catalogues of faces and places, trying to see where she might fit in. College? Your first job? That party for a friend of a friend you went to last year? Despite not being exactly sure who this person is, you feel some emotional connection to her, and are sure you’ve met before. The Capgras delusion is like the opposite of this familiar feeling. You see the face of your spouse, but, lacking any emotional connection, are certain he is an impostor. In a Radiolab short, Dr. Carol Berman explains it’s as if “the feeling or the essence of the person…the soul of the person isn’t in there.” And if Black Mirror’s Be Right Back taught us anything, it’s that a replacement for a loved one is very difficult to accept.

Is this more or less creepy if one is an impostor?
Different from prosopagnosia, this isn’t an inability to recognize faces. It’s actually in spite of the admittedly remarkable resemblance that the belief persists, in line with the DSM-5 definition of delusions as “fixed beliefs that are not amenable to change in light of conflicting evidence.” First described in 1923 by Capgras and Reboul-Lachaux as “L’illusion des sosies” [2], meaning the illusion of look-alikes, the Capgras delusion was originally reported in psychiatric disorders (e.g. schizophrenia), but has also been associated with neurodegenerative disorders (e.g. Alzheimer’s disease) as well as with epilepsy, brain injury, cerebrovascular disease, hypothyroidism, and migraine attacks [3].
It’s been proposed that a simple failure in communication between brain regions could lead to Capgras [4]. Imagine your mother walks into a room. Visual information reaches your fusiform face area, and you recognize this face as your mother’s. At the same time there’s a problem with the connection (whether physically or functionally) between these visual processing areas and the limbic system, especially the amygdala, which usually provides important emotional information. If these regions aren’t communicating properly, you end up with a visual perception of a face indistinguishable from your mother’s without any of the associated feelings. That eerie lack of emotional response leads you to conclude that this person you feel nothing towards must be an impostor.
One patient’s behavior provided evidence of a specific disconnect between two regions, rather than a malfunction of one or another. He only experienced the delusion that his parents were impostors when he saw them in person, but when he heard their voices over the phone he was able to recognize them as themselves [4]. It seems both his emotional and visual representations were able to function fine independently, his auditory-emotional connection was intact, and only the visual-emotional connection was impaired. Capgras isn’t exclusively visual either. One paper reported the case of a blind woman who believed her cat was “replaced by a replica which was ‘ill-intentioned’ towards her” [5] based on sound alone, pointing to a specific auditory-emotional disconnect.
Initial evidence for this hypothesis relied on the galvanic skin response, a measure of autonomic arousal. The autonomic nervous system is involved in the things our bodies do to respond to the environment without conscious thought or effort, like increasing or decreasing heart rate. Changes in autonomic arousal can be used to indicate emotional information processing, and has been linked to amygdala activation. In healthy people there is a stereotypical, strong autonomic arousal (measured via galvanic skin response) to pictures of familiar faces. Patients with Capgras don’t show this automatic arousal to familiar faces, and this failure – indicative of an abnormal emotional response – could cause the delusion [4, 6, 7].
He perseverated on this content despite attempts to engage him: “How can you help me, I am dead.” When asked about suicidal ideation he indicated, “I am dead, how can I be suicidal?” When providers commented on the novelty of speaking with a dead person, he replied, “Maybe you are dead too” [8].
Also rare, related to identity, and first described by a Frenchman (Vive La France!) [1] the Cotard delusion is the belief that you are dead or do not exist. While 89% of patients with Cotard delusion also have symptoms of depression [9], these patients do not wish to die, but feel true apathy toward death, thinking of additional bodily harm as “redundant” [1]. Rather than a disconnect between just one sensory area and the limbic system, there’s a hypothesis that a lack of emotional information accompanies all sensory modalities in Cotard delusion, and it would be suspected that these patients would lack a strong autonomic arousal to all kinds of external stimuli, not just to faces [10].
However, recent work suggests that there must be something more to both Capgras and Cotard than a failure of autonomic responses. Meaning, there’s a need for a second deficit that impairs the part of the brain that would otherwise reject this delusional belief (“you’re an impostor,” or “I’m dead”) after it has arisen [11]. Otherwise, why would the belief persist despite all of the evidence to the contrary? For example, patients with lesions to part of their prefrontal cortex lack strong autonomic responses to pictures of familiar faces (like in Capgras), but do not have delusions about the identities of these familiar people. Meanwhile, patients with an autonomic nervous system condition known as “pure autonomic failure” show no autonomic response to any type of sensory stimuli (like is predicted to be the case in Cotard), and yet they don’t believe they are dead [11].
Support for the need of a second factor (beyond the autonomic failure) to cause these delusions comes from a recent study of 17 patients with brain lesions causing delusional misidentifications. The authors examined the lesion locations and found that they were all functionally connected to an area of the brain that’s active in studies of familiarity (left retrosplenial cortex) [12]. What’s more, 16 of the lesions were also functionally connected to a region active during expectation violation (right frontal cortex), which is part of belief evaluation [12]. So, beyond the damage that caused the lack of familiar feelings, these patients also had damage that impaired their abilities to evaluate their belief that this lack of familiarity meant there was an impostor in their midst.
While these two disorders are very rare, the impaired sense of self-identity and the identity of your loved ones is something all too common in people suffering from dementia. A sense of your own and others identities requires a complicated combination of memories and sensory and emotional information, and involves many different brain areas. Hard as we might try, no sandwich-inspired chart can begin to approach this level of complexity. Perhaps that’s why the IRS boiled down my identity to just one form of ID from Column A and one from Column B.
References
[1] Riggs, S., Perry, T., Dowben, J. & Burson, R. (2017). Vive La France: Three Delusional Disorders Originally Reported in the French Medical Literature. Perspect Psychiatr Care, 53, 5–9.
[2] Capgras, J., & Reboul-Lachaux, J. (1923). L’illusion des ‘‘sosies’’dans un delire systematize. Soc Clin Med Ment., 11, 6–16.
[3] Cannas, A., Meloni, M., Mascia, M.M. et al. (2017). Capgras syndrome in Parkinson’s disease: two new cases and literature review. Neurol Sci., 38, 225.
[4] Hirstein, W., & Ramachandran, V. S. (1997). Capgras syndrome: a novel probe for understanding the neural representation of the identity and familiarity of persons. Proceedings of the Royal Society B: Biological Sciences, 264(1380), 437–444.
[5] Reid, I., Young, A.W., & Hellawell, D.J. (1993). Voice recognition impairment in a blind Capgras patient. Behav Neurol., 6(4), 225-228.
[6] Ellis, H.D., Young, A.W., Quayle, A.H., & de Pauw, K.W. (1997). Reduced autonomic responses to faces in Capgras delusion. Proc R Soc Lond Biol Sci., B264, 1085–1092.
[7] Brighetti, G., Bonifacci, P., Borlimi, R., & Ottaviani, C. (2007). “Far from the heart far from the eye”: Evidence from the Capgras delusion. Cognitive Neuropsychiaty, 12(3), 189-197.
[8] Bott, N., Keller, C., Kuppuswamy, M., Spelber, D., & Zeier, J. (2016). Cotard Delusion in the Context of Schizophrenia: A Case Report and Review of the Literature. Frontiers in Psychology, 7, 1351.
[9] Solimine, S., Chan, S., & Morihara, S. K. (2016). Cotard Syndrome: “I’m Dead, So Why Do I Need to Eat?” The Primary Care Companion for CNS Disorders, 18(2), 10.4088/PCC.15l01862.
[10] Ramachandran, V. S. & Blakeslee, S. (1998). Phantoms in the brain: Probing the mysteries of the human mind, New York: William Morrow.
[11] Coltheart, M. (2007). The 33rd Sir Frederick Bartlett Lecture Cognitive neuropsychiatry and delusional belief. The Quarterly Journal of Experimental Psychology, 60(8), 1041-1062.
[12] Darby, R.R., Laganiere, S., Pascual-Leone, A., Prasad, S., & Fox, M.D. (2017). Finding the imposter: brain connectivity of lesions causing delusional misidentifications. Brain, 140(2), 497-507.

You must be logged in to post a comment.