 March
23
March
23
Tags
Clearing the fog around brain fog
When was the last time you forgot where you kept your keys, or blanked out on someone’s name during an important conversation, or got distracted and abandoned an important task? While everyone might have faced these problems on more than one occasion, chances are that for most of us, these events are few and far between. Now imagine having to deal with these events occurring more often, occasionally lasting for hours or even days. This could range from something as innocuous as forgetting someone’s name, to something much more consequential as forgetting to pick up your child from school. Many people suffer from these symptoms days on end, and go through the motions of daily life as if their brains are cluttered and fogged, unable to focus on tasks or retrieve vital information, and generally experiencing a condition termed “brain fog”.
The fogged up brain
The first time I heard about brain fog was when a friend declared that she was feeling like her brain wasn’t functioning properly. She felt mentally fatigued, had trouble multi-tasking and sometimes found it hard to focus on a specific task – all symptoms of brain fog, yet commonly dismissed as “just stress”. It was no great surprise when a few months later she was diagnosed with hypothyroidism – a thyroid hormone deficiency disorder resulting in symptoms such as impaired temperature sensation, slow metabolism and brain fog. In fact, a survey of over 5000 hypothyroidism patients revealed that about 80% experience brain fog, and about 46% experience brain fog symptoms even before the diagnosis [1], just like my friend.
During a book tour of the novel Jonanthan Strange and Mr. Norrell, author Sussana Clarke was diagnosed with chronic fatigue syndrome (CFS; also known as myalgic encephalomyelitis), and she had to abruptly stop working. Brain fog is one of the major symptoms of CFS. Clarke’s particular case is an example of how debilitating brain fog can be, as she struggled to keep track of the elaborate worlds and characters she built in her fantasy novel, and eventually paused writing the much-awaited sequel due to her illness [2].
CFS and hypothyroidism are not the only causes of brain fog. Cancer patients and survivors who have undergone chemotherapy (Central Nervous System (CNS) and non-CNS cancers), lupus patients, menopausal and pregnant women also experience brain fog to varying degrees. These days, people are more aware of this phenomenon, because it is also experienced by COVID-19 patients, particularly those who have symptoms lasting for months, aka long COVID.
From a neuroscience standpoint, it is fascinating that many disorders with vastly different etiologies present brain fog as a prominent symptom. For instance, hypothyroidism is a hormonal disorder, and pregnancy and menopause are associated with major hormonal changes and fluctuations. On the other hand, lupus is a chronic autoimmune disorder, and COVID-19, being a viral infection, elicits immune responses. Cancer treatment and chemotherapeutic drugs cause a specific type of brain fog, called ‘chemo fog’ or ‘chemo brain’ [3]. To date, there is no known single cause for CFS [4]. Despite different origins, studying the pathophysiology, or the underlying mechanisms of these disorders, can shed light on how and why brain fog occurs.
Microglia – frenemies of the brain
One of the most common pathophysiologies for all the conditions that cause brain fog is neuroinflammation. Neuroinflammation is caused by activation of the innate immune system of the central nervous system. In other words, it is a process by which the immune system within the brain is able to get rid of infectious particles and dead cells.
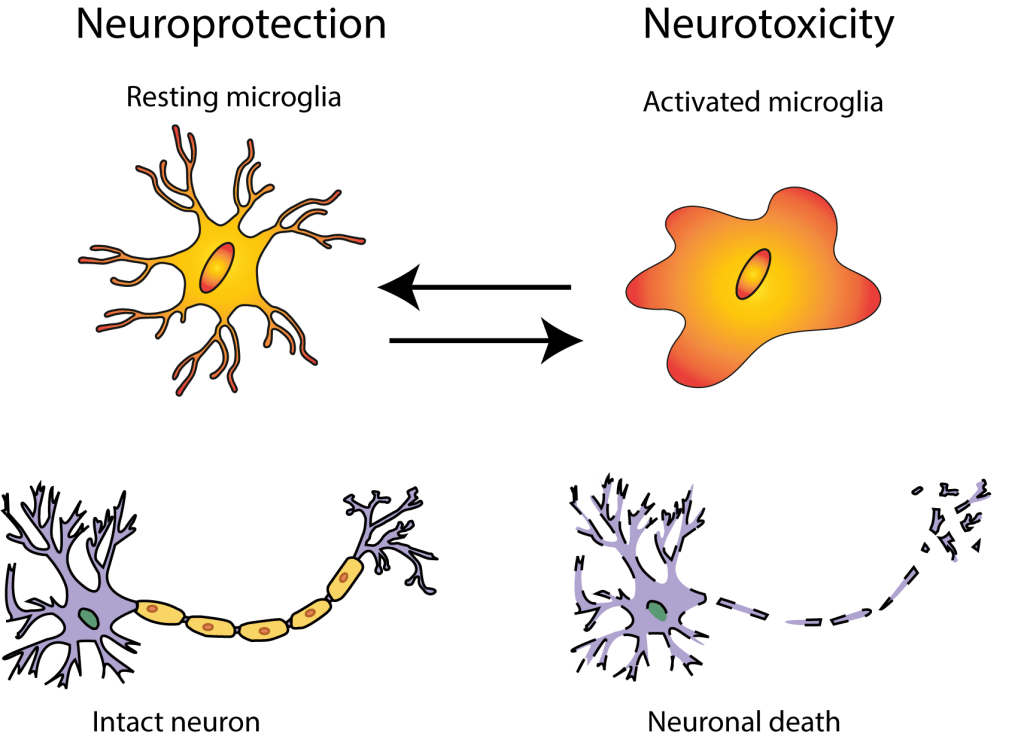
One of the primary immune cells within the nervous system are microglia – which are responsible for maintaining a healthy brain, precisely by clearing out microbes and dead debris [5]. However, if the microglia are over-activated (such as in the case of neurodegenerative disease), neuroprotection can soon turn into neurotoxicity. In other words, over-active microglia wrongly attack useful connections between neurons, hamper formation of new neural cells within the area of the brain important for memory formation, and disrupt the protective insulation of neurons, which literally results in “frayed nerves”.
All the negative effects of persistent activation of microglia are observed in mice treated with a commonly used chemotherapeutic drug [3, 6]. In addition, chemotherapy-treated mice also show memory deficits, similar to the behavioral deficits shown by patients with chemo fog [3]. Interestingly, a new study found that mice with mild COVID-19 also had persistently active microglia [7]. Activated microglia secrete certain proteins, and the level of these proteins were found to be increased in patients with CFS, who self-reported higher fatigue scores [8]. A form of auto-immune hypothyroidism, called Hashimoto’s syndrome, is also associated with neuroinflammation – a mouse model of this disease showed anxiety-like and depressive-like behaviors, along with increased levels of biomarkers for activated microglia [9]. While neuroinflammation is seen in all of the above disorders causing brain fog, it is important to remember that there can be several different underlying causes for brain fog in patients suffering from these disorders [10].
Challenges and opportunities
How does brain fog experienced by a hypothyroidism patient differ from that experienced by a cancer treatment patient? How can we differentiate brain fog, a chronic long-term condition, from bad and stressful days? These are but two out of many unanswered questions. Addressing the second question is especially important for preventing missed diagnostic opportunities, as well as avoiding misdiagnosis. One of the challenges of studying brain fog is the lack of objective diagnostic tests. While doctors use fatigue scales to rate patients’ severity of fatigue, most or all of these scores are obtained through patient self-reporting or via answers to questionnaires [11].
The other challenge is that these diagnostic tests are not uniformly used. For instance, a major challenge of determining the cause of brain fog in cancer treatment patients is that brain fog/fatigue diagnostics are not conducted before chemotherapy. There is an added layer of complexity since illness representation among patients can indicate increased levels of anxiety and fatigue (i.e. the expectation of brain fog symptoms might prime patients to be more sensitive and could inflate self-reporting scores). Therefore it is imperative that scientists, diagnosticians, doctors and clinicians develop objective methods and uniform diagnostic measures to catch brain fog earlier in disease progression.
Given that we understand so little about brain fog, and the process of discovering mechanistic details is time-consuming, the only therapeutic option available to patients suffering from brain fog at this time is symptom management. While medication to treat the underlying disease causing brain fog is prescribed, patients are also advised to improve sleeping habits, follow an exercise regimen, maintain a balanced diet and take diet supplements such as multivitamins, antioxidants and probiotics [10, 12]. Probiotics are a particularly attractive option, and a recent study showed that gut samples of patients suffering from CFS lacked two health-promoting bacterial species [12]. Interestingly, patients with lower concentration of these bacteria reported higher fatigue scores. Gut microbiome plays a role in maintaining the blood-brain barrier, which blocks foreign materials from entering the brain, and thereby can prevent microglia over-activation. More such studies are required to discover and develop effective therapeutic strategies.
A new world
Surviving cancer due to chemotherapy is a medical achievement, as well as an example of the resilient spirit of survivors. Yet, these cancer survivors are left to deal with another form of debilitating, though thankfully not life-threatening, illness. As of January 2023, 11% of people in the US who had COVID-19 suffer from long COVID, which adds to the millions of people suffering from brian fog due to hypothyroidism and CFS worldwide. Brain fog is an immediate public mental health crisis and requires our urgent attention.
Sixteen years after collapsing during her book tour, Susanna Clarke was able to publish a new novel, Piranesi, completely different from her first novel, yet equally rich and complex in its fantastical world-building. She managed to capture the intricacies of CFS and embed them in her story-telling [13]. Clarke’s journey is inspiring, to those with or without brain fog, as she continues to navigate the world around her despite chronic mental health challenges.
References
[1] Ettleson, Matthew D., Ava Raine, Alice Batistuzzo, Samuel P. Batista, Elizabeth McAninch, Maria Cristina T. V. Teixeira, Jacqueline Jonklaas, Neda Laiteerapong, Miriam O. Ribeiro, and Antonio C. Bianco. “Brain Fog in Hypothyroidism: Understanding the Patient’s Perspective.” Endocrine Practice : Official Journal of the American College of Endocrinology and the American Association of Clinical Endocrinologists 28, no. 3 (March 2022): 257–64. https://doi.org/10.1016/j.eprac.2021.12.003.
[3] Gibson, Erin M., Surya Nagaraja, Alfonso Ocampo, Lydia T. Tam, Lauren S. Wood, Praveen N. Pallegar, Jacob J. Greene, et al. “Methotrexate Chemotherapy Induces Persistent Tri-Glial Dysregulation That Underlies Chemotherapy-Related Cognitive Impairment.” Cell 176, no. 1 (January 10, 2019): 43-55.e13. https://doi.org/10.1016/j.cell.2018.10.049.
[4] Komaroff, Anthony L., and W. Ian Lipkin. “Insights from Myalgic Encephalomyelitis/Chronic Fatigue Syndrome May Help Unravel the Pathogenesis of Postacute COVID-19 Syndrome.” Trends in Molecular Medicine 27, no. 9 (September 1, 2021): 895–906. https://doi.org/10.1016/j.molmed.2021.06.002.
[5] Colonna, Marco, and Oleg Butovsky. “Microglia Function in the Central Nervous System During Health and Neurodegeneration.” Annual Review of Immunology 35, no. 1 (April 26, 2017): 441–68. https://doi.org/10.1146/annurev-immunol-051116-052358.
[6] Gibson, Erin M., and Michelle Monje. “Microglia in Cancer Therapy-Related Cognitive Impairment.” Trends in Neurosciences 44, no. 6 (June 1, 2021): 441–51. https://doi.org/10.1016/j.tins.2021.02.003.
[7] Fernández-Castañeda, Anthony, Peiwen Lu, Anna C. Geraghty, Eric Song, Myoung-Hwa Lee, Jamie Wood, Belgin Yalçın, et al. “Mild Respiratory SARS-CoV-2 Infection Can Cause Multi-Lineage Cellular Dysregulation and Myelin Loss in the Brain.” BioRxiv, January 1, 2022, 2022.01.07.475453. https://doi.org/10.1101/2022.01.07.475453.
[8] Nakatomi, Yasuhito, Kei Mizuno, Akira Ishii, Yasuhiro Wada, Masaaki Tanaka, Shusaku Tazawa, Kayo Onoe, et al. “Neuroinflammation in Patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: An 11C-(<em>R</Em>)-PK11195 PET Study.” Journal of Nuclear Medicine 55, no. 6 (June 1, 2014): 945. https://doi.org/10.2967/jnumed.113.131045.
[9] Cai, Yao-Jun, Fen Wang, Zhang-Xiang Chen, Li Li, Hua Fan, Zhang-Bi Wu, Jin-Fang Ge, Wen Hu, Qu-Nan Wang, and De-Fa Zhu. “Hashimoto’s Thyroiditis Induces Neuroinflammation and Emotional Alterations in Euthyroid Mice.” Journal of Neuroinflammation 15, no. 1 (October 29, 2018): 299. https://doi.org/10.1186/s12974-018-1341-z.
[10] Samuels, Mary H., and Lori J. Bernstein. “Brain Fog in Hypothyroidism: What Is It, How Is It Measured, and What Can Be Done About It.” Thyroid 32, no. 7 (July 1, 2022): 752–63. https://doi.org/10.1089/thy.2022.0139.
[11] https://dsq-sds.org/article/view/938/1113
[12] Guo, Cheng, Xiaoyu Che, Thomas Briese, Amit Ranjan, Orchid Allicock, Rachel A. Yates, Aaron Cheng, et al. “Deficient Butyrate-Producing Capacity in the Gut Microbiome Is Associated with Bacterial Network Disturbances and Fatigue Symptoms in ME/CFS.” Cell Host & Microbe 31, no. 2 (February 8, 2023): 288-304.e8. https://doi.org/10.1016/j.chom.2023.01.004.
[13] https://www.newyorker.com/magazine/2020/09/14/susanna-clarkes-fantasy-world-of-interiors
Cover image credits: Jacqueline Mosko and DallE

You must be logged in to post a comment.