 May
08
May
08
Tags
Neurons, Footballs, and the Draft! Oh my!
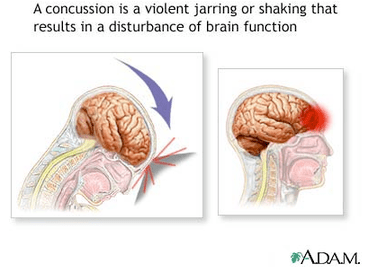
Tonight, a few hundred football players will be chosen by one of the 32 teams of the National Football League in the hopes of making millions of dollars and establishing their names in the glory of NFL history. Yet only a tiny fraction of college football players, 1.6%, and an even smaller fraction of high school players, 0.08%, ever get drafted by an NFL team1. Though improvements in rules and equipment have made football much safer than it used to be, the risk of serious injury remains. Perhaps the scariest injury that can occur in football is the concussion. Concussions are relatively common both in the NFL (approximately 0.4 concussions occur per NFL game2) and in college and high school (34.9% of high school players reported having multiple concussions3) football, but we still don’t fully understand the long-term effects of these brain injuries. What exactly is a concussion? Well, it results from your brain literally bouncing around in your skull. Pretty scary, right? To make matters worse, concussion symptoms vary widely, making them difficult to diagnose, especially during fast-paced games. And diagnosing concussions on site is extremely important because scientists have discovered that multiple concussions can lead to severe cognitive symptoms and other neurological problems, including the widely publicized disease chronic traumatic encephalopathy, or CTE4, although the science of how concussions can cause long-term problems largely remains a mystery.
Because of this danger, public figures such as popular science author Malcolm Gladwell5 believe that the popularity of football will not last long because parents and players will no longer be willing to accept the risk. Even President Barack Obama said earlier this year “I would not let my son play pro football6,” Especially after the jarring suicides of highly-regarded NFL players, including Junior Seau and Dave Duerson, there has been ongoing media coverage of the controversy and increasing public concern over concussions7. Although this coverage tends to imply a straight line from multiple concussions to CTE (I admit to having that impression before researching this post), there have been few articles that have gone into detail about the mechanisms of how concussions cause damage to the brain. This is understandable: the story of concussion awareness and prevention is complicated and incomplete, and has closely followed the progress of neuroscience and medicine toward understanding how the brain works.
The First Football Crisis
Originally played at elite colleges such as Harvard and Yale, American football first became popular at the end of the 19th century. This version of football was much different than the game we know today: there were no helmets or pads, and no forward passes. Opposing players essentially lined up and ran into each other at full-speed in an attempt to push the ball carrier forward a couple yards. As you would expect, there were a huge amount of injuries, and in the early 1900’s a string of football-related deaths occurred, many caused by skull fractures and brain contusions. This led to a public uproar, forcing rules changes designed to reduce dangerous contact, and eventually requiring players to wear plastic helmets (though they were primarily designed to protect against skull fracture8). While the new rules were effective in reducing injuries in general, they failed to address a known problem that was all too often – and too easily – ignored.
A report detailing the injuries on the Harvard football team during the 1905 season9 expressed concern that concussions may be taken too lightly: “concussion was treated by the players in general as a trivial injury and rather regarded as a joke.” However, the authors’ observations over the season were “not sufficient for us to draw any definite conclusions, but from conversation with various neurologists, we have obtained very various opinions in regard to the possibility of serious after effects.” Not even the neurologists of the time had any sort of consensus as to whether concussions had negative long-term effects. However, we should forgive these neurologists because very little was known about the brain at the time. Neuroscience was in its infancy. A few scientists still explained the brain using phrenology. That very same year, Santiago Ramon y Cajal and Camillo Golgi, considered among of the fathers of neuroscience, shared the Nobel Prize in Physiology or Medicine for their pioneering work on the anatomy of the brain10,11. It would be several more decades before another pair of famous neuroscientists, Hodgkin and Huxley, described the fundamental means of neural communication, the action potential12.
What is a Concussion?
After over a century of neuroscience research we now have a pretty good idea of what happens to the brain during a concussion.
This is perhaps best explained by an analogy: Imagine your skull is your car, and your brain is you, the driver. A concussion is similar to your car crashing into something. However, there is one important difference – your brain doesn’t have a seatbelt. So imagine you are driving without a seatbelt.
This brain should really be wearing a seatbelt – http://www.geekosystem.com/
When your car collides with something, it stops very quickly, but you keep moving until you collide with the door, window, windshield, or all of the above (your brain can bounce around in a high-impact collision, causing significant injury to the opposite side of the brain to where the impact occurred). Considering all the possible variations of the velocity and angle of the collision, along with the unique shapes of people’s brains, this could explain some of the variability in concussion symptoms – brain areas responsible for different functions can be affected. Unfortunately, at the moment we do not have the technology to put seatbelts inside of your skull to prevent concussions. What we can do is put a cushion around the outside of the car (i.e. a helmet), which is moderately effective in decreasing the suddenness of collisions, but you still don’t have a seatbelt and will bounce around on the inside. While they are excellent at preventing skull fractures and helpful in preventing concussions13, there is only so much a helmet can do.

See if you can find me in this picture…Hint: I’m not one of the cheerleaders. http://wheresrooster.com/wp-content/uploads/2010/10/Helmet.jpg
The Sterile Inflammatory Response
But what happens inside of your head down at the cellular level during a concussion? It turns out that often it is not the initial impact that causes the most damage to the brain, but the body’s response to the injury. There are two phases of traumatic brain injury: the initial physical injury and the secondary reaction of the body. The first phase is virtually instantaneous – neurons at the point of impact are stretched, twisted, or crushed. However, the second phase is much slower, taking on the order of minutes to hours. This slower response is known as the sterile inflammatory response: in cases such as concussions when an injury is sterile, meaning no foreign bacteria, viruses, etc. enter, the body’s immune response can do more harm than good14. Our immune system is very efficient at fighting off infections because of its speed and lethality, but this can cause collateral damage to nearby cells. If you scrape your arm in the dirt, you want this response to be strong and fast in order to prevent an infection from taking hold. Losing some skin cells in the process is a small price to pay; they’ll grow back anyway. However, this is a serious problem when it happens in the brain – collateral damage to neurons near the injury can cause serious cognitive deficits, and these neurons won’t grow back.

Figure from Roth et al. (2014) showing the overreactive immune response to concussions in the brain. Immune cells are in green and the damaging chemicals they use to kill bacteria and viruses are in red.
These processes only account for the acute symptoms of concussions, however. The current concussion controversy revolves around the connection between multiple concussions over a whole career and the neurodegenerative disorder chronic traumatic encephalopathy, or CTE.
Punch Drunk
Links between repetitive head trauma and neurological troubles later in life have been documented going back almost a hundred years. In the early 20th century, boxing became enormously popular in the US, and even more so than football it featured, and encouraged, hits to the head. A study of boxers at the time described the “punch drunk” state: “Fighters in whom the early symptoms are well recognized are said by the fans to be ‘cuckoo,’ ‘goofy,’ ‘cutting paper dolls,’ or ‘slug nutty’ … Many cases remain mild in nature and do not progress beyond this point.” However, in some cases “marked mental deterioration may set in necessitating commitment to an asylum”15. A systematic study of boxers with progressive neurological disease was not performed until 1957, when Critchley first described “chronic progressive traumatic encephalopathy of boxers,” with symptoms varying from memory deficits to depression to uninhibited violent behavior16. Later, a study of 224 former boxers found that 17% suffered from these types of neurological symptoms and that the severity of symptoms correlated with the length of the boxers’ careers17.

A fight involving one of the most famous and successful boxers of all time, Jack Dempsey. http://en.wikipedia.org/wiki/File:Jack_Dempsey_v_Georges_Carpentier_cph.3b35134.jpg
While we have a decent understanding of the acute effects of concussions on a cellular level, how repeated head trauma can lead to chronic neurodegenerative diseases like CTE remains largely a mystery. Many contact sport athletes never develop symptoms despite suffering multiple concussions during their careers18. CTE is similar to a number of other neurodegenerative diseases – including Alzheimer’s – in that one of its symptoms is the pathological accumulation of a protein, called tau, in particular areas of the brain4. What distinguishes CTE from the other tau-related diseases is where this protein accumulates – emotional centers of the brain including the amygdala and hippocampus. It is unknown whether this specifically causes emotional symptoms in people suffering from CTE. However, almost half of confirmed CTE patients also had a second neurodegenerative disorder, such as Alzheimer’s18. The relationship between these diseases and symptoms is complicated, and in order to disambiguate the root causes of and risk factors for CTE more extensive research will have to be done, not only on individuals with CTE but also on those who have suffered multiple concussions yet do not experience adverse symptoms later in life.

Figure from Tartaglia et al. (2014) showing the overlap of symptoms in different concussion-related and non-concussion-related disorders. The connections between these different disorders is still unclear and the subject of intense ongoing research.
Can Concussions be Treated or Prevented?
Now that we have a better understanding of the physics and molecular biology of concussions, there may be ways to reduce their frequency or severity. The most recent generation of football helmets is more effective than the last at preventing concussions (13), and it is conceivable that helmets can be further improved to reduce – though probably not eliminate – the incidence of concussions. A recent study using a mouse model of concussions19 found that applying an antioxidant to the skull immediately after a concussion reduced the amount of tissue damage and cell death by counteracting immune system’s sterile inflammatory response20. While this seems a potentially promising treatment for concussions, it is a very long way from being used in humans. Many more rounds of tests must be performed, especially on the long-term consequences of using such a chemical in the brain.

Figure from Roth et al. (2014) showing a substantially decreased immune response (in green) in the brain to a concussion when treated with the antioxidant glutathione (“vehicle” is the control condition).
Perhaps for now the best approach to concussion prevention is moderation. One popular idea is to institute “hit counts,” akin to “pitch counts” in baseball, and thus decrease the chances of suffering a concussion by decreasing the total amount of contact. It also makes sense that only the best concussion-reducing helmets should be used. These steps are particularly important for younger players, as their brains are still developing and are thought to be much more vulnerable to serious damage resulting from head trauma.
Over the next few days of the NFL Draft extravaganza, I’ll be rooting for the Seahawks to draft good players to help them keep winning football games (because winning is great – perhaps a subject for a future post). But over the next several years I’ll be rooting for the ongoing efforts of the dedicated scientists researching the long term effects of concussions and figuring out ways to prevent them. Hopefully sometime in the near future, playing the most popular sport in the US will no longer carry such a risk of long-term brain injury – especially in the interests of the vast majority of football players who will not have the opportunity to earn millions playing in the NFL.
References:
- http://www.ncaa.org/about/resources/research/probability-competing-beyond-high-school
- Casson, I. R., Viano, D. C., Powell, J. W. & Pellman, E. J. Twelve years of national football league concussion data. Sports Health 2, 471–83 (2010).
- Mckee, A. C., Daneshvar, D. H., Alvarez, V. E. & Stein, T. D. The neuropathology of sport. 29–51 (2014). doi:10.1007/s00401-013-1230-6
- Tartaglia, M. C. et al. Chronic traumatic encephalopathy and other neurodegenerative proteinopathies. Front. Hum. Neurosci. 8, 30 (2014).
- http://www.cbssports.com/collegefootball/writer/dennis-dodd/23380419/author-malcolm-gladwell-says-football-will-become-ghettoized
- http://www.newyorker.com/reporting/2014/01/27/140127fa_fact_remnick?currentPage=all
- http://mmqb.si.com/tag/head-trauma-in-football-a-special-report/
- Harrison, E. A. & Harvey, W. Head Injury and Evidence in Early American Football. 1–12 (2014). doi:10.2105/AJPH.2013.301840
- E. H. Nichols and H.B. Smith. The Physical Aspect of American Football. Boston Medical and Surgical Journal (1906):1.
- Cajal, S. Ramón y, 1888a. Estructura de los centros nerviosos de las aves. Rev. Trimest. Histol. Norm. Patol. 1, 1–10.
- Golgi, C., 1873. Sulla struttura della sostanza grigia del cervelo. Gazzetta Medica Italiana. Lombardia 33, 244–246.
- Hodgkin, A. & Huxley, A. A quantitative description of membrane current and its application to conduction and excitation in nerve. J. Physiol. 500–544 (1952).
- Hampshire, N. et al. Can helmet design reduce the risk of concussion in football? 1–4 (2014). doi:10.3171/2014.1.JNS13916
- Rock, K. L., Latz, E., Ontiveros, F. & Kono, H. The sterile inflammatory response. Annu. Rev. Immunol. 28, 321–42 (2010).
- Martland, H. (1928). Punch drunk. JAMA 91, 1103–1107. doi: 10.1001/jama.1928.02700150029009
- Critchley, M. (1957). Medical Aspects of Boxing, Particularly from a neurological standpoint. BMJ 1, 357–362. doi: 10.1136/bmj.1.5015.357
- Roberts, A. (1969). Brain Damage in Boxers: a Study of the Prevalence of Traumatic Encephalopathy among Ex-Professional Boxers. London: Pitman Medical and Scientific Publishing Co., Ltd.
- McKee, A. C., Stern, R. A., Nowinski, C. J., Stern, R. A., Daneshvar, D. H., Alvarez, V. E., et al. (2013). The spectrum of disease in chronic traumatic encephalopathy. Brain 136, 43–64. doi: 10.1093/brain/aws307
- http://mmqb.si.com/2014/04/17/mouse-concussions-nfl-cte/
- Roth, T. L. et al. Transcranial amelioration of inflammation and cell death after brain injury. Nature 505, 223–8 (2014).


Pingback: “It ain’t about how hard you hit” | NeuWrite San Diego