 November
10
November
10
Tags
Say Cheese: The neuroscience of our devotion to dairy
You might be the kind of person that can’t wait for the “cheese pull” when grabbing a hot slice of pizza, or perhaps you’re the first at the table to suggest a cheese-filled charcuterie board for your appetizer (both of these examples are stemming from personal experience, of course). If you are a fellow cheese lover, you’ll know that there is just something about eating cheese that makes you feel amazing. What if I told you there were a neuroscientific basis for those good feelings, and that there are some surprising potential similarities between the euphoric feelings produced by cheese and those produced by narcotic drugs?
Cheese and opioids?
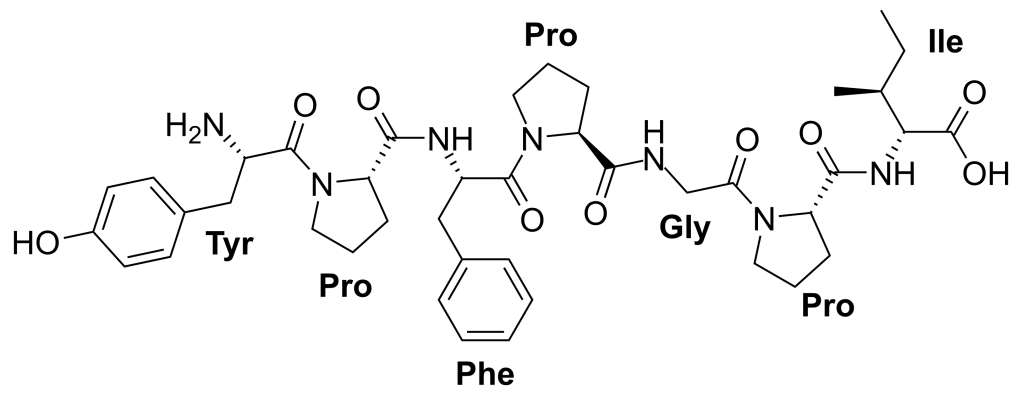
To better understand how cheese might affect our brains and bodies, let’s first look at how dairy products are processed by our digestive system. The protein in milk is primarily made up of a molecule called casein. In fact, casein accounts for up to 80% of the protein in cow’s milk. When producing cheese from milk, the casein content is concentrated, making cheese the premier source of casein on grocery store shelves [1]. During digestion, enzymes in the gastrointestinal tract break casein down into a molecule called casomorphin. If the name of this molecule looks familiar to you, it is probably because of its similarity to the molecule morphine, which is a popular opioid drug used for pain relief. This similarity is for good reason – casomorphin is an opioid molecule that binds to the same receptors in our nervous systems that handle opioid drugs.
Opioid drugs have become an important topic of study in recent decades due to the prevalence of opioid addiction and overdose deaths during the current opioid epidemic. Opioids are extremely effective at treating pain, but come with a host of unwanted side effects such as addiction and drug abuse, tolerance prompting continually increased use, and suppression of breathing that can lead to death. This is because the receptors on the surface of neurons that respond to opioids are found all over the brain in groups of cells responsible for changing our perception of pain, but also in cells that are important for reward and breathing rhythm.
This may leave you wondering why our brains would evolve to respond to opioid drugs in such harmful ways. Why have opioid receptors in the reward circuits that prompt addiction? In fact, the human body also creates its own opioid molecules called endogenous opioids. If you’ve ever heard of a “runner’s high”, a phenomenon in which exercise produces feelings of euphoria, you are looking at an experience caused by endorphins, another family of opioid molecules that bind to opioid receptors. The brain produces these endorphins to make us feel good and reinforce exercise behavior to keep our bodies healthy. The same concept has been shown for endogenous opioid production to reinforce food consumption. The same brain circuits that mediate the rewarding feeling that prompts further opioid drug use also keep us eating and control both our “liking” (a pleasurable response to eating) and “wanting” (our drive to fulfill some need) of food (see this previous NeuWrite article for more info on this topic!) [2]. Although this reinforcement is less necessary when food is more abundant in the modern era, evolutionarily speaking, promoting the consumption of food is an important survival mechanism.
How does casomorphin work?
Knowing now that eating cheese leads to the release of the opioid molecule casomorphin, is there strong evidence that these dietary opioids are the cause of our specific love for cheese? Are we truly cheese addicted at the opioid circuit level? Well, there are actually a variety of hypotheses of what casomorphin molecules do. Some sources suggest that casomorphin does have a direct effect on the parts of our brains that control reward and reinforcement, which means it is absorbed into our digestive tract, travels in the blood, evades chemicals in the blood and tissue that break down protein molecules, crosses the extremely fickle blood-brain barrier, and binds to opioid receptors in our brains [3]. Its effect on those brain circuits reinforces the feeding behavior and bolsters the consumption of cheese in the purest sense. The possibility of casomorphin reaching the brain is supported by the finding of casomorphin in the brain tissue of infants that received casein through feeding on breastmilk, indicating that the above steps happened successfully [4,5].
Other scientists instead posit that casomorphin may just act in the digestive tract and isn’t involved in reward processing per se. Interestingly, the parts of our nervous system that control the gut also have opioid receptors that are thought to be important for absorption and secretion of chemicals into the digestive tract and gut motility (which is perhaps why constipation is a common side effect of opioid drug use) [6]. Casomorphins may simply stay in the gut and control how we absorb other nutrients from cheese via opioid receptors there. Casomorphin and other similar milk-derived opioids have been shown to lengthen the time it takes for food to progress through the gastrointestinal tract, reduce diarrhea, and stimulate the secretion of molecules important for controlling metabolism [7]. While there are currently two different schools of thought on the function of casomorphin – “works in the brain” vs. “works in the gut”, it will take further research to determine which camp (or perhaps both) are correct.
What else do we love about cheese?
Assuming that direct activation of the brain’s opioid receptors by casomorphin is perhaps only a part of why eating cheese is so darn rewarding, what are other characteristics of cheese that might contribute to its “hyperpalatability” (the term we use to describe foods that are excessively pleasurable to eat)? As the Western diet continues to progress away from whole foods (fruits, veggies, legumes, etc.) and towards hyperpalatable, highly processed foods (cheese, potato chips, ice cream, etc.), neuroscientists and psychologists have attempted to pin down the exact signals in modern food that promote our fixation on and loss of control around certain foods.
One psychological study [8] asked college students to reflect on which foods from a list they felt were the most “problematic,” or how out of control and prone to overeating they felt when presented with that food. Unsurprisingly, chocolate, ice cream, and french fries topped the list, while plain cucumber, broccoli, and beans brought up the rear. The researchers determined that the level of processing the food went through, the glycemic load (which depends on the amount of refined carbohydrates and how fast they are processed in the body), and the fat content all contributed to the overeating potential of the foods on their list.
Controlled laboratory testing in rodents shows that exposure to both fatty and sugary foods can lead to behavioral signs similar to drug addiction, such as binge eating and the willingness to endure painful shocks to the feet in order to obtain the rewarding food. By comparison, mice and rats fed normal rodent food don’t display this kind of behavior. Interestingly, the cessation of binge eating sugary foods can lead to withdrawal symptoms in rodents that are shockingly similar to that seen after opioid use, including tremors, teeth chattering, and aggressive behavior. More importantly for our understanding of the rewarding effects of cheese and despite being less studied, binge eating of high fat food results in some neuroscientific and behavioral similarities to sugar binging and drug use. While rats that binge on fatty foods don’t display typical signs of drug withdrawal, they do exhibit signs similar to addiction, such as the tolerance of pain to gain access to food and even neurochemical changes in the brain that are reminiscent of drug abuse [9]. Further, salty food has been hypothesized to function through similar reward channels to reinforce sodium consumption [10], a function that has been recently counterproductive in a society with unlimited access to heavily processed, sodium-laden food.

Cheese & I
We still have a lot to understand about our complicated relationship with cheese, especially since this bond is probably a consequence of a variety of factors from our evolutionary response to food, the possible effect of food-derived opioids, and societal factors with which our physiology hasn’t quite kept up. It’s possible that you really could be “addicted” to cheese through direct effects of casomorphin on brain reward mechanisms much like opioid drugs, or perhaps the fatty, salty goodness of cheese is enough to kick those same brain circuits into high gear through the evolutionary mechanisms that keep us eating. So, if you ever feel your mouth watering over fondue or find yourself standing in front of the fridge with some shredded cheddar after work, rest assured that your brain is working as designed.
References
- Panoff L (2019) Is Cheese Addictive? Healthline.com (https://www.healthline.com/nutrition/is-cheese-addictive); Accessed November 10, 2022
- Le Merrer J, Becker JAJ, Befort K, Kieffer BL (2009) Reward processing by the opioid system in the brain. Physiological Reviews, 89: 1379-1412
- Peuhkuri K, Sihvola N, Korpela R (2011) Dietary proteins and food-related reward signals. Food & Nutrition Research, 55:5595
- Pasi A, Mahler H, Lansel N, Bernasconi C, Messiha FS (1993) Beta-casomorphin-immunoreactivity in the brain stem of the human infant. Research Communications in Chemical Pathology and Pharmacology, 80(3):305-322
- Jarmolowska B, Sidor K, Iwan M, Bielikowicz K, Kaczmarski M, Kostyra E, Kostyra H (2007) Changes of beta-casomorphin content in human milk during lactation. Peptides, 28:1982-1986
- Holzer P (2009) Opioid receptors in the gastrointestinal tract. Regulatory Peptides, 155(1-3):11-17
- Meisel, H (2005) Biochemical properties of peptides encrypted in bovine milk proteins. Current Medicinal Chemistry, 12:1905-1919
- Schulte EM, Avena NM, Gearhardt AN (2015) Which foods may be addictive? The roles of processing, fat content, and glycemic load. PLoS ONE, 10(2): e0117959
- Avena NM (2010) The study of food addiction using animal models of binge eating. Appetite, 55(3):734-737
- Morris MJ, Na ES, Johnson AK (2008) Salt craving: the psychobiology of pathogenic sodium intake. Physiology & Behavior, 94(5): 709-721
Cover Image Source: Eva K./Wikimedia Commons/GFDL 1.2)

You must be logged in to post a comment.