 June
28
June
28
Tags
Zika: Predicting the long-term effects of an unrelenting virus
Summer is upon us, and with that comes much-anticipated vacation travel. As you pack your bag with sunblock, clothes that haven’t seen the light of day since your trip last year, and that sci-fi novel that has been sitting on your nightstand since February, don’t forget what might be the most important item: bug spray.
Although it’s no longer a major media focus, the Zika virus hasn’t disappeared since it came on the scene in 2015. As of June, 2018, over 4,000 women in the United States and its territories have tested positive for Zika. Frighteningly, there’s still so much we don’t know about it, including its long-term effects.
Just to recap: Zika is mainly carried and spread by the Aedes aegypti mosquito. Although Zika has been around for decades, it was brought to global attention in 2015 during a devastating outbreak in Brazil. In February of 2016 the World Health Organization (WHO) declared this outbreak a Public Health Emergency.
Zika has now been firmly established as a cause of microcephaly and studies continue to show that the Zika virus is neurotropic (preferentially attacking the nervous system). However, researchers have discovered that only around 10% of Zika-exposed fetuses present any kind of malformation when born. Many infants exposed to Zika in utero are born with a normal head size but then quickly display serious cognitive deficiencies and motor impairments as they age. This means that solely investigating the consequences of Zika in children who show physical deformities provides a limited snapshot of the potential consequences of this virus.
It has only been a few years since the 2015 outbreak, so our ability to study the long-term consequences of Zika exposure in humans is limited. Consequently, researchers have begun using model systems, like cerebral organoids (i.e. “mini-brains”) or mice. These models will enable scientists to predict neurocognitive effects of the virus, hopefully gathering information that will allow early intervention and improve the quality of life for those infected with Zika.
Earlier this month, researchers in Rio de Janeiro, Brazil published a study in which they investigated the long-term impact of Zika infection in mice and discovered that an FDA-approved drug holds the potential for reducing the effects of Zika exposure.
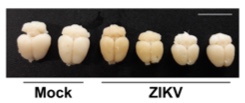
Example control (mock) and Zika-infected mouse brains at 23 days post-infection. (Souza and Frost et al. Science Translational Medicine)
The team, led by researchers Souza and Frost, infected newborn (postnatal day 3) mice with the Zika virus. They chose postnatal day 3 because at that time a mouse’s brain and immune system are at a stage of maturity comparable to a human fetus in its second or third gestational trimester.
Previous epidemiological and clinical studies showed that Zika-infected infants, regardless of whether they were microcephalic, were more likely to have spontaneous seizures than healthy babies. This led the research team to hypothesize that the Zika-infected mice would be more prone to seizures during development.

Mice received a Zika or control (mock) injection at postnatal day 3 (P3). (Souza and Frost et al. Science Translational Medicine)
Zika infection leads to seizures in both humans and mice
Sure enough, they found that 65% of animals had seizures on the 9th day after Zika infection. By 12 days post-infection, when replication of the Zika virus in the brains of these mice was highest, 88% of the mice exhibited seizures. These seizures did, however, subside as the mice grew older– by 100 days post-infection, no seizures were recorded for Zika-infected mice.
The researchers were intrigued by the possibility that the effect they saw may be even more obvious, and possibly provide more information, if mice were given a proconvulsant, a drug that can causes epileptic seizures. They used well-established proconvulsant pentylenetetrazol (PTZ), an inhibitor of g-aminobutyric acid (GABA) receptors. GABA is an inhibitory neurotransmitter—its action reduces activity of the nervous system. When GABA can no longer bind to its receptor, the nervous system is essentially in firing overload, and that’s what causes those seizures.
They found that, even at 100 and 110 days post Zika infection, infected mice were more susceptible to these pharmacologically-induced seizures than non-infected mice. This may indicate that infants infected with Zika are more likely to suffer from long-term neurochemical imbalances.
Zika infection affects motor function
In addition to seizures, normocephalic babies infected with Zika have shown serious motor dysfunction. With this in mind, the researchers performed a variety of behavioral tests with Zika-infected mice and found that, at 9 days post-infection, older male and female mice showed decreased muscle strength in a hindlimb suspension test. Both sexes also showed impaired locomotion. In addition, these mice were unable to distinguish between novel and familiar objects in a novel object recognition test, a sign of short-term memory impairment.
Zika and brain atrophy
Cell death and impaired neural precursor proliferation, (i.e. expansion of stem cell populations required for the production of multiple brain cell types), are well-established consequences of Zika infection– infants born with a normal head circumference but exposed to Zika in utero can later develop microcephaly.
The Brazil-based research team found that Zika-infected mice showed brain atrophy and necrosis of various brain structures, including the hippocampus. A few mice showed severe brain atrophy when the virus was at its peak point of replication. Of greatest concern, the observed cell death persisted into adulthood, raising concerns about the ultimate neurological consequences for children exposed to Zika as they move into adulthood.
Immune response to Zika
The team knew that seizure-causing epileptic disorders had been linked to inflammation of the brain, and so they decided to investigate whether this inflammation could also be present for those infected with Zika. The research team found that the brains of Zika-infected mice did in fact show increased inflammation, based on expression of various immune response genes.
So, what could be done to reduce this inflammatory response and possibly lessen the immediate and long-term effects of Zika infection?
The research team aimed to answer this question by manipulating the immune system. They treated Zika-infected mice with tumor necrosis factor-alpha (TNF-α) neutralizing antibody infliximab from the day of injection (postnatal day 3) to 12 days post-injection. TNF-α is a cell-signaling protein, produced by immune cells, that causes inflammation. Infliximab inhibits TNF-α, and in doing so decreases the inflammatory response.
Zika-infected mice treated with infliximab showed a decrease in seizures at 12 days post-injection. This suggested that decreasing immune response early on in infection, using drugs like infliximab, could be essential for decreasing the prevalence of, or even preventing, seizures in individuals exposed to Zika. Unfortunately, they found that memory and motor impairments caused by Zika infection were not alleviated by infliximab treatment.
Zika’s lasting impact
Researchers are working to better understand Zika and propose potential treatments, but this unrelenting virus has already done a great deal of damage, and we’re still left with so many questions.
What are the long-term effects of Zika beyond the individual and their family?
How will communities, entire nations, the planet be impacted by Zika? And how will we address that impact?
If we look to the past, it’s clear that disease, oftentimes caused by a virus, has molded societies, and is believed to have played a significant role in the origin of humans. To further that point, viral DNA makes up about 8% of our genome!

Interactive map courtesy of the Centers for Disease Control and Prevention
So, for now, what’s the best course of action? Your best bet is to avoid exposure, regardless of your age and if you plan to get pregnant. If you think you’ve been exposed and are considering starting a family, absolutely get tested. Researchers will continue to make strides in understanding this virus, but it may be a long road until we can prevent its effects, or eradicate it altogether.
In the meantime, stay informed by checking in with organizations like the CDC— and don’t forget to pack that bug spray!
Samantha (Sam) Jones is a science researcher and writer who just completed her PhD in the Biomedical Sciences program at UCSD. Sam grew up in the Boston area as an avid Red Sox fan and lover of lobster and moved to the West Coast in 2013 to start graduate school. As a graduate student she became increasingly passionate about improving public science literacy, which led her to writing geared toward the general public. When not hunched over a computer, you can find her reading, teaching yoga, and spending time outside appreciating the beautiful San Diego weather.

You must be logged in to post a comment.