 February
24
February
24
Tags
The Neuroscience of Stress
Not to brag, but I would consider myself to be an expert in stress – not the study of it, but because of how often I’ve experienced it throughout my adult life (yay, grad school!). If you’re reading this article, I’m guessing you can think of a time when you’ve experienced stress, whether that’s cramming before a final exam, preparing for a job interview, or figuring out what to do with your life. But what is stress, exactly?
What we think of as stress is actually activation of the stress response [1]. The stress response happens when our brain detects a real or potential threat. Neural circuits activate which engage our body to respond to the threat and reestablish allostasis (the active process of regulating your body to maintain stability). For the most part this system works well, especially in an acute (short-term) crisis like running from a bear. This was advantageous for our ancestors who had to worry about evading predators and finding enough food for the day. But in today’s society, although we no longer encounter the same acute stressors like running from predators trying to eat us, we face a different kind of danger. Psychological and social stressors can activate our stress response chronically (all the time). When we are chronically stressed, our bodies don’t have a chance to recover, and this can lead to a multitude of mental and physical problems (Figure 1).
Not all stress is bad, however. In addition to helping us in short-term emergencies, a healthy level of stress can also motivate us to be productive and focused, and to make progress toward our goals. Without any stress, life would be pretty boring. But as our stress levels increase for long periods of time, this starts to cause wear and tear on our body, leading to fatigue, exhaustion, and burnout [2].
So what happens to our brain when we’re stressed, and what effects can this have on our mental and physical well-being? And finally, how can our understanding of stress help us to develop better strategies to manage it, and to live a more balanced and purposeful life?
A brief history of the study of stress
Coined the “father of stress research,” Hans Selye was a scientist who, sometime in the 1930s, stumbled upon a finding that revolutionized the way we think about stress [1]. His research involved injecting rats with a specific compound. He found that the injection led the rats to develop an array of health problems. After rejoicing about discovering the effect of this new compound, he then tested a control group of rats he injected with only salt water (as any good scientist would). To his surprise, these rats developed the exact same health conditions. He continued to inject new groups of rats with different kinds of compounds and always got the same result. Eventually, he realized that rather than a compound making the rats sick, it was the experience of the injection itself that was causing these symptoms. In other words – stress was making the rats sick!
Selye went on to develop the concept of “general adaptation syndrome,” which has evolved into what we call the stress response today [1]. The syndrome consists of three stages: first is the alarm phase where the stressor is initially perceived. This is followed by the resistance phase, where the stress response is activated and your body attempts to return to a baseline level. The exhaustion phase occurs when the stressor persists and therefore your stress response cannot turn off (chronic stress). This is precisely when stress begins to cause more harm than good. Selye was not only the first to define stress from a biological standpoint, he was also the first to theorize that overexposing the body to stress can lead to exhaustion and sickness – an important point that I’ll touch on a bit later.
The stressed-out brain
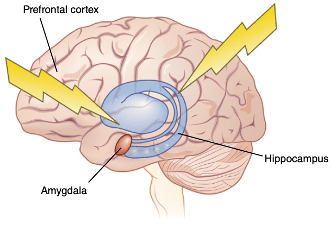
The stress response is a complex process that involves interactions between the brain, the body, and countless neurotransmitters and hormones that I won’t have time to address in this article. Instead, I will focus on three brain regions that play a major role in regulating the stress response: the amygdala, hippocampus, and prefrontal cortex (PFC).
Let’s start with the amygdala: a small but mighty structure that is important for many functions including memory, decision making and emotional processing. Research suggests that over-activation of the amygdala is correlated with increased stress responses [2]. The amygdala’s level of reactivity to a perceived threat has been shown to predict vulnerability to stress [1]. Subjects with overactive amygdalas are also more likely to experience depression and anxiety symptoms, indicating a possible connection between stress and psychological disorders [1]. Interestingly, the amygdala responds to stress differently in males and females [3]. In males, stress decreased activity between the amygdala and other brain regions necessary for interpreting and understanding others’ emotions; in females, stress increased this activity. This may explain why men are more likely to withdraw during stress, while women are more likely to seek social support [3].
The hippocampus is involved in encoding memories about facts and events, as well as spatial navigation. As you might imagine, stressful events tend to be remembered. These memories are crucial for our survival, as they enable us to learn from our mistakes and avoid future danger. A 2010 study confirmed that acute stress enhances memory consolidation and performance [5]. However, chronic or extreme stress can dysregulate this system, resulting in conditions like post-traumatic stress disorder (PTSD) [5]. Studies have shown that PTSD patients have impaired memory function and reduced hippocampal volume [4]. These impairments may be related to the fact that neurons in the hippocampus have an abundance of receptors for glucocorticoids – the main hormone that is released during the stress response [2]. Along with chronic stress and PTSD, shrinkage of the hippocampus has also been linked to Alzheimer’s disease and major depression [2]. Although the underlying mechanism connecting each of these factors remains a mystery, current research indicates that the hippocampus plays a significant role in the relationship between stress, memory, and disease.
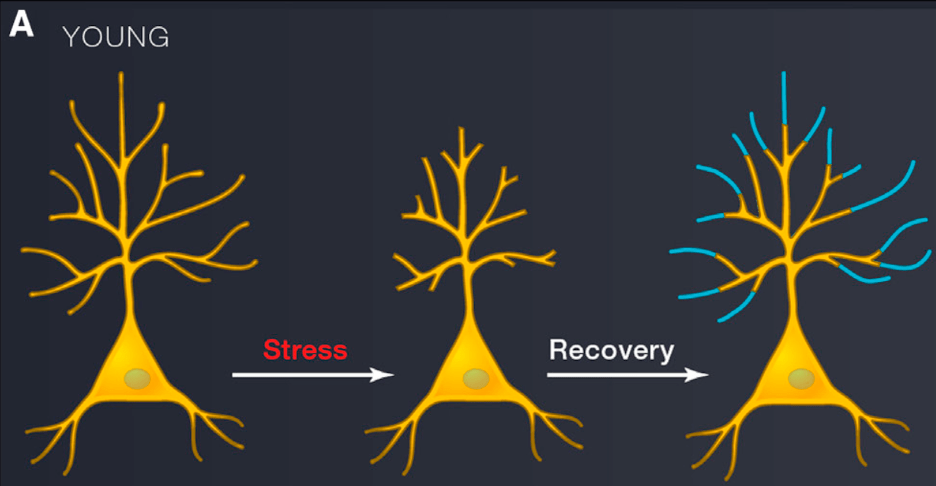
The PFC is another important structure involved in memory, planning, decision making, and other complex cognitive behaviors. Stress has been shown to affect both the structure and function of the PFC (along with the amygdala and hippocampus). In rats, chronic stress led to decreased functioning of PFC neurons and impaired performance on PFC-dependent tasks [6]. Damage to PFC neurons has a ripple effect on the rest of the stress system – for instance, projections from the hippocampus to the PFC, and from the PFC to the amygdala are necessary for regulation of the stress response [6]. But there’s good news! When the stress was removed, young animals showed resilience, meaning their PFC neurons recovered [6]. This is because the PFC is capable of neuroplasticity, or the ability of neural circuits to rewire and form new connections. However as we age, neurons in the PFC become less resilient to stress [6].
While the link between stress and disease is still not fully understood, one thing is clear: chronic stress is bad for us. Future work studying brain regions like the amygdala, hippocampus, and PFC will continue to reveal new ways that chronic stress impacts the mind and body, and how this may make us more susceptible to physical and psychological disease.
Relationship between stress and disease
We know that stress is linked to a variety of physical and mental health problems, though there is still some debate about causality (did the stress make you sick, or does being sick make you stressed?). The general consensus, though, is that continued stress can only increase your risk of getting diseases [9]. Initially, stress activates the immune system to engage defenses against injury and pathogens [1]. But as the stress response continues, such as in instances of chronic stress, immunity begins to be suppressed [1]. Interestingly, one of the main treatments for autoimmune disease is to give patients large amounts of glucocorticoids (the hormone released during the stress response) [9]. It might sound counterintuitive, but because this treatment suppresses the immune system, the body can no longer continue to attack itself. To sum this up: immediate stress activates the immune system, and prolonged stress suppresses it.
In terms of psychological disorders, while it’s unlikely that stress is the sole cause of anxiety or depression, there is a lot of evidence to suggest that stress presents additional risk to genetically predisposed individuals. Studies have shown that a significant proportion of patients with major depression have increased concentrations of cortisol (another important stress hormone) [1]. Patients with major depression were also found to have a 10-15% smaller hippocampus [7]. Chronic stress, particularly early in life, poses a risk for psychiatric disease [8]. Early life stress has been shown to disrupt the development and function of the brain’s limbic system (including the amygdala and hippocampus, which send projections to the PFC) [8]. Exposure to severe stressors can lead to PTSD, though this is not always the case, which indicates that other factors play a role in the development of PTSD such as the type of stressor, genetics, and socioeconomic status [1]. So, while you probably don’t have to worry about stress causing depression, be aware that chronic stress could be changing your brain in ways that may make you more susceptible to depression and other mental illnesses.
How this knowledge can help us
If you’ve made it this far, I suspect you may be experiencing a higher level of stress (sorry!). Fortunately, there remain some silver linings to be learned from this research. First, although stress is linked to several negative outcomes, the truth is that these mental and physical responses don’t happen to everyone. In fact, the majority of people recover from the stress response, and can adapt their habits or behavior to lessen its effects in the future [10]. Along those same lines, our brains are capable of neural plasticity – meaning as we learn new coping mechanisms and skills, our brain rewires and forms new connections [10]. And finally, we can take action to build resilience and strengthen these new neural pathways [10]. Some examples of this include physical exercise, mindfulness meditation, therapy, seeking support in friends and family, and finding meaning and purpose in our lives.
Although stress is an unavoidable consequence of life, keep in mind that a healthy level of stress can actually be good for us. Within a healthy range of stress or during acute stressors, the stress response is necessary to activate our brain and body to react accordingly and bring ourselves back to a baseline level. But even if you cross over into chronic or extreme stress, you are not doomed! Humans are ever-changing beings capable of recovering and adapting. While it might not feel like it in those difficult moments, we can learn to manage stress in a way that allows us to lead meaningful and fulfilling lives.
References
- Godoy, L. D., Rossignoli, M. T., Delfino-Pereira, P., Garcia-Cairasco, N., & de Lima Umeoka, E. H. (2018). A comprehensive overview on stress neurobiology: basic concepts and clinical implications. Frontiers in behavioral neuroscience, 127.
- McEwen, B. S., Bowles, N. P., Gray, J. D., Hill, M. N., Hunter, R. G., Karatsoreos, I. N., & Nasca, C. (2015). Mechanisms of stress in the brain. Nature neuroscience, 18(10), 1353-1363.
- Mather, M., Lighthall, N. R., Nga, L., & Gorlick, M. A. (2010). Sex differences in how stress affects brain activity during face viewing. Neuroreport, 21(14), 933.
- Douglas, J. (1999, October). Alterations in brain structure and function associated with post-traumatic stress disorder. In Seminars in clinical neuropsychiatry (Vol. 4, No. 4, pp. 249-255).
- Henckens, M. J., Hermans, E. J., Pu, Z., Joëls, M., & Fernández, G. (2009). Stressed memories: how acute stress affects memory formation in humans. Journal of Neuroscience, 29(32), 10111-10119.
- McEwen, B. S., & Morrison, J. H. (2013). The brain on stress: vulnerability and plasticity of the prefrontal cortex over the life course. Neuron, 79(1), 16-29.
- Sapolsky, R. M. (2000). The possibility of neurotoxicity in the hippocampus in major depression: a primer on neuron death. Biological psychiatry, 48(8), 755-765.
- Peña, C. J., Kronman, H. G., Walker, D. M., Cates, H. M., Bagot, R. C., Purushothaman, I., … & Nestler, E. J. (2017). Early life stress confers lifelong stress susceptibility in mice via ventral tegmental area OTX2. Science, 356(6343), 1185-1188.
- Sapolsky, R. M. (2004). Why zebras don’t get ulcers: The acclaimed guide to stress, stress-related diseases, and coping. Holt paperbacks.
- McEwen, B. S., Gray, J. D., & Nasca, C. (2015). Recognizing resilience: Learning from the effects of stress on the brain. Neurobiology of stress, 1, 1-11.


You must be logged in to post a comment.