 October
06
October
06
Tags
Fighting COVID might leave you with a bad taste in your mouth
It’s never a good feeling to find yourself gazing at two strong, dark purple lines on your at-home COVID test. Not only are you staring down at least five days of isolation, but you likely don’t feel physically great either. During a recent bout of COVID, I had the usual symptoms – severe sore throat, body aches, runny nose, and coughing. What I didn’t see coming was shooting awake in bed that very night with an absolutely awful taste in my mouth. It was as if I had sucked on cough medication tablets designed to be swallowed, or eaten a not-quite-right grapefruit. Water did absolutely nothing to ease the feeling. With my tongue prickling, I realized that this symptom wasn’t a reaction to COVID at all, but instead a supposedly rare side effect of starting the antiviral drug prescribed by my doctor to treat it.
An effective antiviral treatment for COVID
The drug in question here is Paxlovid, an antiviral regimen produced by pharmaceutical giant Pfizer that began to make its way to patients in December of 2021. Paxlovid is the brand name for two known drugs packaged together: nirmatrelvir, which is an antiviral chemical known to fight coronaviruses of many kinds in humans, and ritonavir, an antiviral drug that boosts the effects of other antiviral medications and helps them stick around in the body for longer before being broken down. Both of these drugs are protease inhibitors. Proteases are enzymes in the body that cut apart other proteins; therefore, protease inhibitors are drugs that stop the target enzyme from being able to do the cutting. Protease inhibitors are commonly used for fighting viruses, especially HIV. Unlike bacterial pathogens that are sensitive to antibiotic drugs, viruses make their impact on the body by hijacking our cells into replicating their genetic material and protein structure for them. By making these copies, they can spread to other cells and hosts. Protease inhibitors fight viruses by disrupting this process of replication, which often relies on proteases to function correctly [1].

In the case of using nirmatrelvir for COVID, the drug targets Mpro, a protease important for cutting the viral particles into their final form to make copies and proliferate in their host [2,3]. Therefore, by inhibiting Mpro, Paxlovid prevents the viral particles from proliferating and further infecting the host. (As an aside, see this previous NeuWrite article for more information on Mpro and its effects on our brain’s blood vessels). When taken within the first five days of COVID symptom onset, Paxlovid has been seen as a kind of miracle drug, with Pfizer reporting in its clinical trials that the risk of death and hospitalization from COVID in patients at high risk of adverse effects was decreased by a whopping 89% [3]. In the real world, one study in Israel found these positive effects from nirmatrelvir during January’s Omicron surge, keeping older adults out of the hospital and preventing their death [4].
While these results strongly support the use of Paxlovid to decrease suffering and death from COVID-19, Pfizer does report in its clinical trial data that 6% of patients that took it experienced “dysgeusia” [5,6]. According to the Cleveland Clinic, dysgeusia is the medical term for a distorted sense of taste and can lead to patients having a constant bad taste in their mouths or perceiving all foods ingested as sour, bitter, or metallic. Dysgeusia can be caused by many different factors, such as infections, medications, and even simply loss of smell (olfaction, or your sense of smell, plays a huge role in taste perception – think about how you may not be able to taste as well when you are sick with a stuffy nose). Ironically, one of the potential symptoms of COVID-19 infection is, in fact, also dysgeusia. More commonly, COVID infection is associated with a loss of taste and smell, although some patients report distorted versions of these senses during recovery.
While Pfizer reports that only a small proportion of patients receiving Paxlovid experience dysgeusia, a very informal poll of my family and friends would suggest otherwise, with most of their responses including some level of altered taste for the duration of the five-day drug regimen. Further googling led me to a variety of articles and personal accounts of “Paxlovid Mouth”, including the hard-to-describe flavor resembling unswallowed medication or rotting citrus. So, what is known about taste and antiviral medications? What are some neuroscientific factors that could underlie this phenomenon?
How do we taste?
Our sense of taste is governed by an intricate network of cells in our mouths that communicate with the brain. The rough surface of our tongues is made up of “papillae,” or bumps that increase the surface area of our tongues and are home to receptors for different sensations. The tiny papillae in the middle of the tongue are actually not related to taste at all. Instead, these sensory receptors send signals regarding touch to the brain and contribute to the idea of “mouthfeel”. The larger, round papillae around the edges and back of the tongue, however, are home to what we know as taste buds, which are groups of 10-50 individual taste receptor cells shaped like flower buds. Each taste receptor cell has proteins on its outer surface that detect the various chemicals in food that give it its distinctive flavors. Once a taste chemical binds to the surface, the corresponding proteins can change the electrical charge of the receptor cell. This allows the receptor cell to send electrical signals through the nervous system to the brain [7]. Once in the brain, the electrical signals from a constellation of taste receptor cells activated at the same time are decoded to determine the details of a flavor.
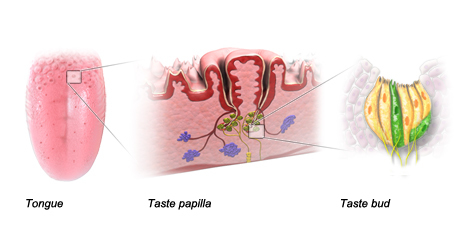
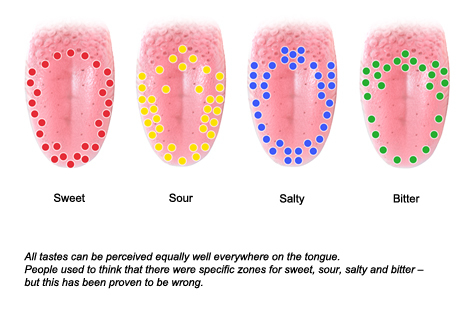
Each taste bud can encode information about a variety of chemicals and flavors, but are often more sensitive to a specific flavor group: sweet, sour, salty, bitter, and savory (or umami). Perhaps most important for understanding Paxlovid’s effect on taste is the fact that our mouth is most strongly attuned to bitter flavors. Despite our love for sweet, sour, or salty, humans have 25 different taste receptors dedicated to encoding bitter chemicals (in comparison, just two taste receptor types cover the processing of sweet taste), and the back of the tongue near the throat is especially sensitive to bitter taste [7,8]. This is probably because bitter tastes often signal the ingestion of dangerous or poisonous compounds, so it is actually more important for our survival that we detect these unpleasant components than the pleasant ones.
Outside of taste, additional sensations can be driven by chemicals that activate other types of receptors in the mouth that transmit temperature or touch information. Called chemesthesis, this process is sometimes confused with taste and can also contribute to unpleasant feelings in the mouth. One very common example of chemesthesis is the sensation of spiciness during which the chemical capsaicin in peppers binds to receptors that are sensitive to irritants and heat. This is why the sensation of ingesting spicy food isn’t quite a flavor, but certainly contributes to the experience of eating it.
What causes Paxlovid Mouth?
So, knowing how the mouth and brain encode tastes and other chemicals, what is the deal with Paxlovid and why did it make my mouth taste so darn bad? It turns out that there is some precedent in the scientific literature for this exact dysgeusia problem stemming from antiviral use. The second Paxlovid component ritonavir has been used in the past to treat another well-known viral disease, HIV. In a study comparing patients that were healthy and those that had HIV, ritonavir itself was described as bitter and affected the ability to detect salty flavors across patients. One possible reason given for the prolonged bitter flavor resulting from ritonavir, as opposed to the brief unpleasantness after tasting something bitter and spitting it out, is that drugs taken systemically and circulating throughout the body are sometimes secreted back into the saliva. In the study referenced above, the amount of ritonavir it took for patients to detect a bitter flavor by tasting the drug reflected the amount one might find in the saliva after given a systemic dose of ritonavir [9].
Although the exact mechanisms by which Paxlovid makes your mouth feel terrible aren’t known, it’s possible that this mechanism stands for the combined antiviral regimen, too. In a recent article from The Atlantic, interviews with health professionals, scientists, and Pfizer itself reveal similar hypotheses. Although Pfizer simply reports that both chemicals are known to be bitter, other hypotheses for the prolonged bitter taste throughout the entire regimen similarly involve secretion of the drugs back into the saliva where they may reactivate certain bitter taste receptors, or trigger chemesthesis receptors that are not often activated by our usual diet. Not only would this lead to a bad taste in your mouth, but a taste that you can’t quite describe having never experienced something similar before.
A further look into the use of antiviral medications that produce dysgeusia shows that this side effect is sometimes intolerable and leads to patients discontinuing treatment. Luckily for sufferers of Paxlovid Mouth, the miserable sensations appear to only remain in place during the five days of treatment and the benefits of the treatment usually outweigh the discomfort (remember, one of the symptoms of your COVID-19 infection could also be dysgeusia, and probably a version that would last much longer). So, if you find yourself suffering through a bitter mouth due to Paxlovid, be sure to find yourself some cinnamon candies to suck on and think about all of the cool neuroscience that is contributing to your malady.
References
- Pfizer. How a protease inhibitor works to fight COVID-19. Accessed September 27, 2022.https://www.pfizer.com/news/articles/how_a_coronavirus_protease_inhibitor_works_to_fight_covid_19
- National Institutes of Health COVID-19 Treatment Guidelines. Ritonavir-boosted nirmatrelvir (Paxlovid). Accessed September 27, 2022. https://www.covid19treatmentguidelines.nih.gov/therapies/antiviral-therapy/ritonavir-boosted-nirmatrelvir–paxlovid-/
- Katella, K. 13 things to know about Paxlovid, the latest COVID-19 pill. Yale Medicine. Accessed September 27, 2022. https://www.yalemedicine.org/news/13-things-to-know-paxlovid-covid-19
- Arbel R, Sagy YW, Hoshen M, Battat E, Lavie G, Sergienko R, Friger M, Waxman JG, Dagan N, Balicer R, Ben-Shlomo Y, Peretz A, Yaron S, Serby D, Hammerman A, Netzer D (2022) Nirmatrelvir use and severe COVID-19 outcomes during the omicron surge. New England Journal of Medicine, 387:790-8.
- Pfizer. Pfizer shares top-line results from phase 2/3 EPIC-PEP study of Paxlovid for post-exposure prophylactic use. Accessed September 27, 2022. https://www.pfizer.com/news/press-release/press-release-detail/pfizer-shares-top-line-results-phase-23-epic-pep-study
- Pfizer. Pfizer reports additional data on Paxlovid supporting upcoming new drug application submission to U.S. FDA. Accessed September 27, 2022. https://www.pfizer.com/news/press-release/press-release-detail/pfizer-reports-additional-data-paxlovidtm-supporting
- Institute for Quality and Efficiency in Health Care (IQWiG): Cologne, Germany (via National Institutes of Health National Library of Medicine, National Center for Biotechnology Information). How does our sense of taste work? Accessed September 27, 2022. https://www.ncbi.nlm.nih.gov/books/NBK279408/
- Ahmad R, Dalziel JE (2020) G protein-coupled receptors in taste physiology and pharmacology. Frontiers in Pharmacology, 11:587664
- Schiffman SS, Zervakis J, Heffron S, Heald AE (1999) Effect of protease inhibitors on the sense of taste. Nutrition, 15:767-772
Cover Image Source: Wikimedia Commons/Kches16414/CC BY-SA 4.0/ https://commons.wikimedia.org/w/index.php?curid=115808735

You must be logged in to post a comment.