 October
13
October
13
Tags
The Wandering Nerve
What do epilepsy, depression, and anxiety all have in common? No, this is not some one-liner joke, there is an actual answer to this question. Could it be that they all could be targeted by a single treatment? To understand how this could be, let’s look into what these disorders are, first.
Epilepsy is a seizure disorder that is characterized by recurring and unpredictable seizures, meaning that for seizures to be considered epileptic, a patient must have more than one without an outside cause (such as drug abuse or recent brain trauma). Of the 70 million patients worldwide diagnosed with epilepsy (citation), about thirty percent of patients are diagnosed with refractory epilepsy, or epilepsy that does not respond to antiepileptic drugs.
Depression has many symptoms associated with it, that range from decreased energy and loss of interest in hobbies or activities, to difficulty concentrating and sleeping, to possible thoughts of suicide and/or attempting suicide (citation). About 5% of adults worldwide are believed to have depression, and approximately 29% to 46% of depressed patients do not respond fully to medicinal treatment (citation;citation).
Anxiety disorders are a class of disorders that all involve a feeling of dread or worry that does not go away and can get worse over time (citation); there are five major types of anxiety disorders, each with its own unique symptoms and triggers. It is estimated that about 40% of patients with an anxiety disorder do not respond completely to medications (citation).
If large portions of people with these disorders do not even respond to medications, then how could all three of them be treated by one therapy? Well, the answer rests in the massive effect of ONE crucial nerve: the vagus nerve,
Vagus nerve: anatomy and physiology
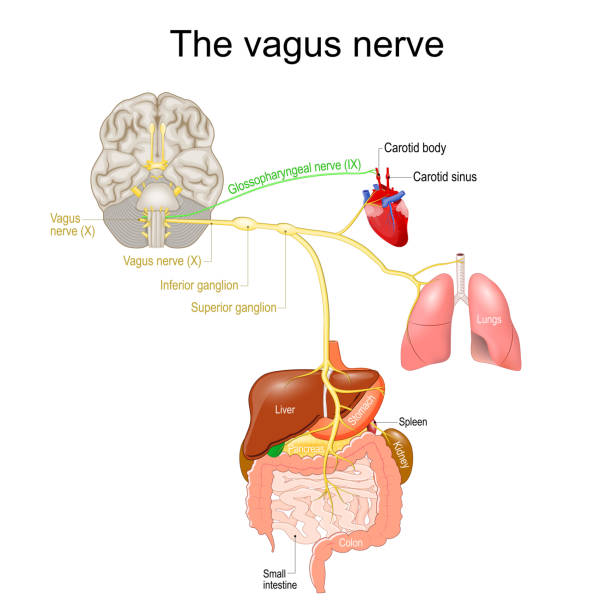
The so-called “wandering nerve” (as its name means in Latin), the vagus nerve plays a role in many of the
vital functions of your body. The vagus nerve is a part of the parasympathetic nervous system (PNS), also known as the “rest and digest” system. It is active when your body is not in “fight or flight” mode, which is instead mediated by the sympathetic nervous system (SNS; NeuWrite Article about the PNS and SNS). As a part of the PNS, the vagus nerve’s role is to send and receive signals that are important for slowing heart rate and breathing, beginning digestion, along with many more functions.
During “fight or flight” mode, the SNS increases heart rate and breathing, while inhibiting digestion and other processes, all in an effort to make sure you and your muscles get as much oxygen as possible. The body prepares to exert itself. In “rest and digest” mode, the PNS—in large part through the vagus nerve—innervates these same regions, just with the opposite effect. The body relaxes. This is all in an effort of self-preservation, and your body does this all unconsciously (without you having to think “ok brain, I need to get away from that tiger, speed up my breathing so I have more strength to do so,” or “ok brain, the coast is clear, time to start digesting again”).
After hearing all of this, you may be beginning to see the potential of the vagus nerve as a target for therapy of various disorders: indeed, there is a therapy using direct electrical stimulation of the vagus nerve to influence the brain, and this has been proven to treat epilepsy. This therapy, called vagus nerve stimulation (VNS), has also been highly efficacious in the treatment of disorders like depression and anxiety.
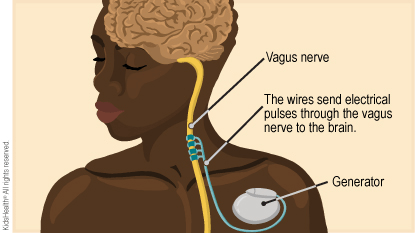
Vagus Nerve Stimulation (VNS)
VNS involves the use of electrodes implanted in the body to stimulate the vagus nerve with direct electrical pulses. The first VNS device was implanted in a human in 1988 to treat drug-resistant epilepsy, and was approved by the Food and Drug Administration (FDA) for the treatment of this type of epilepsy in 1997. Although how it works is still not known, there are several proposed mechanisms including modulation of neurotransmitters (here; here; here), cerebral blood flow (here), and desynchronization of brain activity (here). Regardless of how it works, this therapy has proved useful in treating a plethora of common disorders, including those aforementioned; epilepsy, depression, and anxiety.
VNS and Epilepsy
The first, and main, method used to treat epilepsy is the use of antiepileptic drugs (AEDs); and for some people, their epilepsy can be treated with one or maybe two AEDs. However, as stated earlier, about one-third of those who suffer from epilepsy have a drug-resistant form; luckily, there are alternatives, such as VNS. A study published in 2012 showed that VNS reduced seizure incidence in patients with refractory epilepsy, with “20–40% of patients achieving a greater than 50% reduction in seizure frequency”.There are side effects that may occur, however. The electrodes that VNS uses to stimulate the vagus nerve are placed in the neck because this is where all of its fibers can be targeted at once before reaching the brain. Since this is the case, many of the side effects relate to discomfort in the throat: coughing, hoarseness, throat pain, and even—though of a lower incidence—vocal cord paralysis. Even so, the potential benefits outweigh the risks, for some.
Another non-medicinal treatment of refractory epilepsy is the surgical removal of the region of the brain that is determined to be the origin of the seizures. The caveat of this, however, is that it is highly invasive and may have unforeseen consequences. There are several famous examples from the past of surgical treatment of epilepsy gone awry: in some of these cases, patients were impaired in certain capacities because a region of their brain was removed that was essential for functioning (citation). Despite our increased knowledge about the brain, there still may be serious unforeseen consequences. That is why VNS is such a promising alternative for refractory epilepsy: it is less invasive, has fewer complications, and nothing is removed.
VNS and the Modulation of Neurotransmitters:
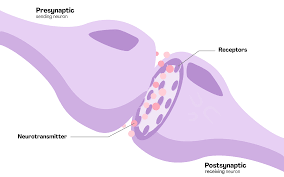
One cause of epilepsy is an imbalance in the ratio of the neurotransmitters glutamate and gamma-aminobutyric acid (GABA). Glutamate is the body’s major excitatory neurotransmitter, and GABA is the major inhibitory neurotransmitter. While the exact mechanisms by which VNS reduces seizure frequency are still unknown, there is a hypothesis that VNS treatment has anticonvulsant effects because it decreases the excitability of the brain (citation). Since epileptic seizures are the result of overexcitation (a lot of neurons firing at once), consider this one crucial finding: when the brains of patients treated with VNS were looked at after a year of treatment, scientists found that there was an increase in the number of receptors that respond to GABA (citation). By increasing responsiveness to GABA, VNS decreases the brain’s excitability, therefore confirming the aforementioned hypothesis.
While testing its efficacy for the treatment of epilepsy, researchers also began to see VNS’s potential for treating common psychiatric illnesses like depression and anxiety disorders. In a study conducted by researchers in 2008, it was found that VNS was effective in reducing the severity of depression, and that efficacy increased over time following the device’s implantation. This study was also significant because it reproduced the results of a similar study conducted by another group, which is the hallmark of good science.
One reason for the antidepressant effect of VNS may be due to the increase in the number of receptors for GABA, that crucial neurotransmitter we talked about earlier. In the brains of patients with depressive disorders, a lower concentration of GABA and GABA receptors has been seen (citation). As well, supplements that increase GABA levels in the brain have been shown to have antidepressant and relaxing effects, attesting to the likelihood that VNS works to protect against all three of these disorders through the modulation of GABA.
Similarly, researchers found that long-term use of VNS in both mice and humans helped improve anxiety and depression by modulating other neurotransmitters (2018). Some concluded that VNS’s therapeutic effects may be a result of an increase in the neurotransmitters serotonin and noradrenaline, which are two neurotransmitters that are commonly targeted for both depressive and anxiety disorders because of their roles in mood regulation and motivation (2011). (citation; citation). More research showed that VNS helped in various anxiety disorders, such as post-traumatic stress disorder (PTSD) and obsessive-compulsive disorder (OCD), and the research found that VNS showed: long-term symptom improvement in humans with anxiety disorders (2008); improvement in tolerance to phobia-based therapies in humans; and significantly reduced signs of anxiety in mice (2018). All of this research attests to the potential that VNS has as a therapeutic alternative for depression and anxiety disorders and that VNS potentially could be approved for therapeutic intervention in patients with depression and anxiety.
The Nerve of the Future?
The vagus nerve is central to most of our vital functions; with such a wide-ranging influence on the body and the brain—from regulating breathing and heart rate, aiding in digestion, along with many more cognitive and emotional functions—the vagus nerve is responsible for so much of our health. This is why it is such an important target for the treatment of a variety of diseases, and why VNS is such an important therapeutic device. Previous NeuWrite articles (here;here) have even talked about how we ourselves can stimulate our vagus nerve through simple deep breathing exercises, so that we can harness our body’s natural relaxation mechanisms. If diseases as disparate as depression and epilepsy can both be treated using VNS, it makes us wonder: what other disorders may benefit from this therapy? How else could we use this wandering nerve to help people?
References
- https://www.frontiersin.org/articles/10.3389/fneur.2017.00301/full
- https://www.nimh.nih.gov/health/topics/depression
- https://pubmed.ncbi.nlm.nih.gov/8827185/#:~:text=Our%20results%20suggest%20that%20between,to%2034%25%20of%20this%20population.
- https://www.who.int/health-topics/depression#tab=tab_1
- https://www.nimh.nih.gov/health/topics/anxiety-disorders
- https://www.hhs.gov/answers/mental-health-and-substance-abuse/what-are-the-five-major-types-of-anxiety-disorders/index.html
- https://www.psychiatrictimes.com/view/treatment-resistant-anxiety-disorders-neurotrophic-perspectives
- https://neuwritesd.org/2022/05/26/why-does-breathing-slowly-make-us-feel-better/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3633308/#:~:text=In%201988%20Penry%20et%20al,treatment%20for%20medically%20refractory%20epilepsy.’
- https://onlinelibrary.wiley.com/doi/10.1002/9781118346396.ch13#:~:text=Summary,levels%20in%20the%20brain%20stem
- https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1528-1157.1998.tb01155.x
- https://www.sciencedirect.com/science/article/abs/pii/0920121194000839
- https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1528-1157.1998.tb01448.x
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3633308/#:~:text=In%201988%20Penry%20et%20al,treatment%20for%20medically%20refractory%20epilepsy.
- https://onlinelibrary.wiley.com/doi/10.1002/9781118346396.ch13#:~:text=Summary,levels%20in%20the%20brain%20stem
- https://psycnet.apa.org/record/1958-01945-001
- https://www.nature.com/articles/1301082
- https://www.sciencedirect.com/science/article/abs/pii/S0920121103001074?via%3Dihub
- https://pubmed.ncbi.nlm.nih.gov/18177525/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3412149/
- https://renuerx.com/general-health/the-role-of-gaba-neurotransmitters-in-depression-anxiety/
- https://www.frontiersin.org/articles/10.3389/fpsyt.2018.00044/full#:~:text=Vagus%20nerve%20stimulation%20has%20shown,%2Dresistant%20depression%20(8)
- https://www.sciencedirect.com/science/article/abs/pii/S0006322311007475
- https://www.healthdirect.gov.au/serotonin#:~:text=Serotonin%20is%20a%20chemical%20that,by%20the%20body’s%20nerve%20cells.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6182595/
- https://www.sciencedirect.com/science/article/abs/pii/S1935861X0800003X
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6301121/
- https://neuwritesd.org/2019/08/29/the-neuroscience-of-the-breath/
- https://www.kenhub.com/en/library/anatomy/the-vagus-nerve
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3400480/


Pingback: Striking and Totally Unexpected | NeuWrite San Diego