 October
01
October
01
Tags
Stem cells and their applications in Neurobiology
You have probably heard about neurons and blood cells, but have you ever wondered where they come from? Their ‘mother’ cells are called stem cells, and not only are the ‘parents’ of all the other cells in our bodies, but they are also a very important tool for all kinds of research!
What are stem cells?
Stem cells are a type of cell in our bodies that are defined by two main characteristics: self-renewal and pluripotency. Self-renewal means that these types of cells are capable of dividing indefinitely, giving rise to the same cell type. Pluripotency means that these cells can become any other type of cell, such as neurons or skin cells, in a process called differentiation. In reality, only the stem cells that are present during early stages of development, early after conception, fully possess these two properties; they are called embryonic stem cells. After we are born and already have a fully developed body, different kinds of stem cells in various parts of our bodies are more limited in their capacity to differentiate into other cell lines. For example, in our bone marrow there is a reservoir of the so-called “hematopoietic” stem cells (hema- comes from Greek and means blood). These cells can differentiate into any type of blood cell, such as platelets, but they are not able to become other non-blood cell types (such as neurons, for instance) under regular physiological conditions. Therefore, we can differentiate between embryonic stem cells, which are truly pluripotent and give rise to all of the other cell types present in our bodies, and adult stem cells, which are more specialized stem cells that can differentiate into specific cell types normally associated with a particular tissue.
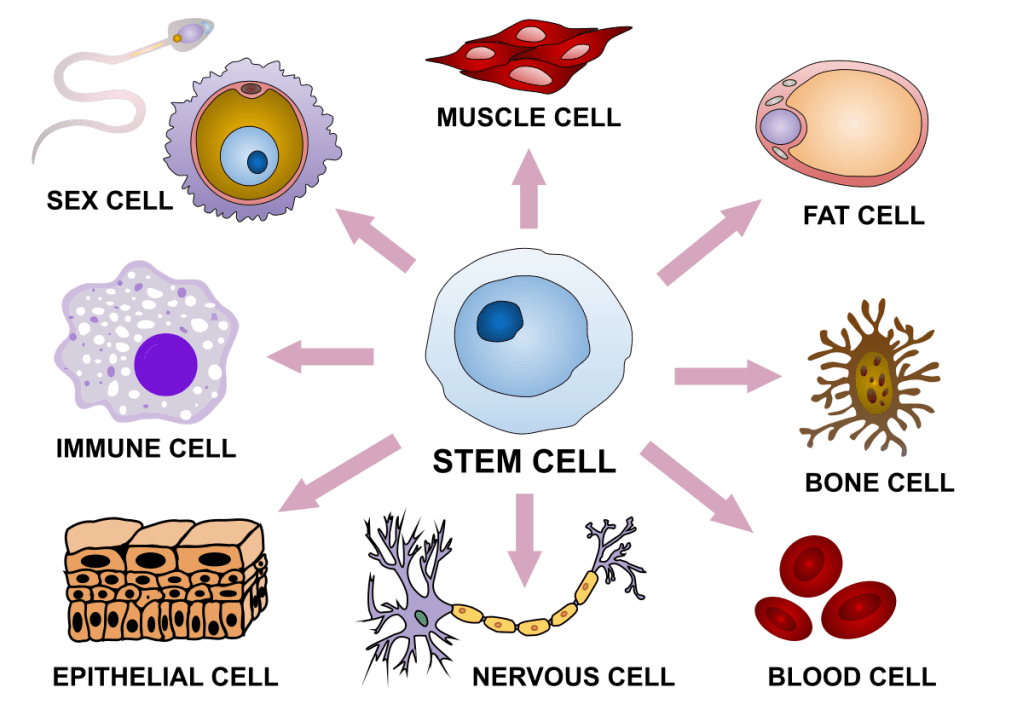
What exactly do stem cells do?
The main function of adult stem cells is to step up to the plate as replacements for old or damaged cells in their particular tissues. For example, in the walls of the intestine, there is a thin layer of cells called intestinal epithelial cells that is in charge of absorbing the nutrients from food into our bloodstream. These cells are exposed to more potential harms than other cell types and can be injured just by the regular physical stress of bowel movements or by interactions with food material. In the small crypts of the intestine, there are niches where intestinal stem cells reside, dividing and constantly giving rise to new intestinal epithelial cells, replacing old and injured cells.
This special flexibility that makes stem cells so useful can also make them dangerous! Their capacity for self-renewal is what allows them to properly perform their regenerative functions, but dysregulation of their proliferation can be devastating, with several types of cancer can arise from rogue stem cells. For example, leukemia can develop if the stem cells in the bone marrow lose their capacity to self-regulate, and so proliferate and differentiate into white blood cells without any control. In those cases, it is possible to perform a bone marrow transplant, or to remove hematopoietic stem cells from patients, treat them in the lab to ‘cure’ them, and then insert them again into the patient [1,2] In essence, adult stem cells can be used for therapy to try to ‘fix’ the tissues they already reside in, and using stem cells to tackle disease is a major field of current research.
Stem cells in the human brain
What about stem cells in the brain? The stem cells that reside in the brain are called neural progenitor cells (NPCs), which are able to differentiate into neurons and glial cells, which are the cells that act as support for neurons. They are most important during development, not only giving rise to the cells that will form our brain after birth, but also helping to modulate the architecture of the brain during formation. They do so by directing the migration and differentiation of newly-formed cells via various signals and cues [3]. However, they are also present in the adult brain, albeit in much lower numbers than during development. Their role in the adult brain is less clear, as they are limited in their capacity to repair injury, and their capability to differentiate into different neuronal types is also a cause for controversy [4]. While most hypotheses point to a potential role of NPCs in the formation of new cells in the adult brain to promote brain plasticity (check our recent article about it!), a lot of questions still remain [5].
Working with NPCs may seem like a complicated endeavor, given that taking biopsies from brain tissue in living humans is a very invasive procedure that cannot be done under normal circumstances. However, scientists have figured out a way to generate NPCs in the lab in a more approachable manner. It turns out that in the same way that stem cells can differentiate into more specific cell types, it’s also possible for differentiated cells to ‘revert’ to a semi-pluripotent state under specific conditions in the lab [6]. The most common procedure to do so is to perform a biopsy of the skin and isolate from it a type of cell called dermal fibroblasts. These cells are in charge of creating the connective tissue in the skin, and while isolated in a dish in the lab, can be reprogrammed to become stem-cell like [7]. The cells created this way are called induced-pluripotent stem cells (iPSCs).
iPSCs have revolutionized research
The advent of iPSC-related technologies has substantially changed the field of research and regenerative medicine. These cells have the potential to become any other cell type of the body and have the same genetic background as the patients they are derived from. As you can probably imagine, the applications here are endless; it is not entirely utopic to think that in the future we might be able to grow organs, or parts of them, that we could transplant back into patients without fear of immunological rejection. Or perhaps we could use these lab-grown organ models to test for drugs that would work in the patient. The first approach is already in use to some degree in many transplant procedures, for example for bone marrow cancers as we mentioned before. The second approach is being explored for many diseases but can be especially important for various types of cancers [8]. In those cases, the therapy approach consists of chemotherapy cocktails where sometimes it is difficult to find the correct combination.
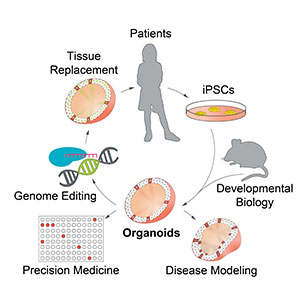
Is it really possible to grow organs in the lab using iPSCs as the starting point? The answer is not yet, but the field is working towards it. Models for different organs of the body already exist: scientists can grow 3D cell models that have similar structural and functional properties as the real thing, which are called ‘organoids’. Many have been developed for tissues like the heart, liver, and intestines (see Review [9] for more details), to the point that they are starting to be suggested as possible therapy to repair injured tissue in these organs [10]. And yes, ‘organoids’ of the brain also exist!
Brain organoids and their applications
Brain organoids can be generated from iPSCs using the right conditions of chemical factors that push them to differentiate into neurons and glial cells. Currently, there are several protocols to develop brain organoids, and you can generate them for different brain regions. This technology opens a big window of opportunity to study early brain development, something very tricky to accomplish otherwise. In the same way, they provide a magnificent tool to study neurodevelopmental disorders, as it is possible to derive iPSCs from, let’s say, schizophrenia patients and compare them to brain organoids from healthy people. This approach is already being used for several neurological disorders (see [11,12] reviews to learn more about this), and important insights are being learned about the mechanisms that give rise to these diseases in the developing brain.
It has now been demonstrated that cells in brain organoids self-organize into internal layers that mimic those of early development when the brain is forming. In the same way, comparing the gene expression of early brain fetuses and brain organoids shows a close resemblance, indicating that they are indeed similar to the early brain during gestation [13]. However, obvious limitations remain. Brain organoids lack very important cell types that are not derived from NPCs, such as microglia, the immune cells of the brain. These cells are generated outside of the brain and migrate there during development, and therefore cannot be obtained by the current methods to generate brain organoids. One possible approach is to generate microglia in parallel and then ‘infuse’ brain organoids with them to then migrate inside and incorporate into the neuron network. Another important feature brain organoids lack is blood vessels. Current protocols also don’t have the capacity to generate the endothelial cells that form the veins and arteries. One way to address this issue has been to transplant brain organoids into mouse brains. It was observed that mouse neurons not only interconnected with the human neurons from the brain organoid, but blood vessels from the mice irrigated into the brain organoid and even became functional [14]. These are very exciting findings that surely will help in solving these important issues.
The field of stem cell therapy and organoids is advancing rapidly and we are bound to observe very impactful changes in the field of regenerative medicine in the future. Stay tuned to learn more about the amazing possibilities that stem cells offer to treat a wide range of human ailments.
References
1. Bonnet, D. Biology of human bone marrow stem cells. Clinical and experimental medicine 3, 140-149 (2003).
2. Leung, W. et al. High success rate of hematopoietic cell transplantation regardless of donor source in children with very high-risk leukemia. Blood 118, 223-230 (2011).
3. Martínez-Cerdeño, V. & Noctor, S.C. Neural Progenitor Cell Terminology. Frontiers in Neuroanatomy 12 (2018).
4. Sorrells, S.F. et al. Human hippocampal neurogenesis drops sharply in children to undetectable levels in adults. Nature 555, 377-381 (2018).
5. Morales, A.V. & Mira, H. Adult Neural Stem Cells: Born to Last. Frontiers in Cell and Developmental Biology 7 (2019).
6. Malik, N. & Rao, M.S. A review of the methods for human iPSC derivation. Methods Mol Biol 997, 23-33 (2013).
7. Park, I.H., Lerou, P.H., Zhao, R., Huo, H. & Daley, G.Q. Generation of human-induced pluripotent stem cells. Nat Protoc 3, 1180-1186 (2008).
8. Kondo, J. & Inoue, M. Application of Cancer Organoid Model for Drug Screening and Personalized Therapy. Cells 8 (2019).
9. Rossi, G., Manfrin, A. & Lutolf, M.P. Progress and potential in organoid research. Nature Reviews Genetics 19, 671-687 (2018).
10. Meran, L. et al. Engineering transplantable jejunal mucosal grafts using patient-derived organoids from children with intestinal failure. Nat Med (2020).
11. Di Lullo, E. & Kriegstein, A.R. The use of brain organoids to investigate neural development and disease. Nature Reviews Neuroscience 18, 573-584 (2017).
12. Trujillo, C.A. & Muotri, A.R. Brain Organoids and the Study of Neurodevelopment. Trends in molecular medicine 24, 982-990 (2018).
13. Amiri, A. et al. Transcriptome and epigenome landscape of human cortical development modeled in organoids. Science 362 (2018).
14. Mansour, A.A. et al. An in vivo model of functional and vascularized human brain organoids. Nat Biotechnol36, 432-441 (2018).

Pingback: BRAIN ORGANOIDS AND ITS ETHICAL IMPLICATIONS | NeuWrite San Diego