 June
29
June
29
Tags
Feelin’ the Beat (Frequency)
What do you think when you read the word interference? If you’re like most people, you probably think it’s negative. Colloquially, interference tends to be obstructive or destructive, like interference keeping your radio or TV from picking up a station, or pass interference in football. I’m NeuWriting to inform you of a recent study in the journal Cell [1] that describes how a type of constructive interference could have an incredibly positive effect…on brains! In short, this interference has the potential to provide a way to non-invasively stimulate specific areas of the brain, which could replace effective, yet invasive brain stimulation technologies currently used to treat movement disorders such as Parkinson’s disease, dystonia, and essential tremor.
Why does this matter? First, you want your brain stimulation to be specific. We know that stimulating very small, specific areas of the brain can treat particular diseases, but also stimulating surrounding areas can have negative side-effects. Second, you want it to be non-invasive, because brain surgery (or any surgery) is always risky. Current brain stimulation technologies are either specific but invasive (requiring implanting electrodes deep in the brain) or non-invasive but non-specific (waving a strong electromagnet over your head). This new method could be both non-invasive and specific, by using electric fields that alone do not affect the brain. These fields interfere with each other in a constructive way that stimulates a specific area of the brain, using the beat frequency of this interference pattern, something I’ll explain later. I should point out that this has so far only been tested in rodents, but because it is non-invasive there’s a chance it could be tested in humans sooner rather than later. In order to explain why this is exciting, I’ll start by going into more depth about two already existing technologies, deep brain stimulation and transcranial magnetic stimulation, as well as their strengths and limitations.
Specific but Invasive
If you think brain stimulation sounds a bit scary, you’re not wrong (although not everyone agrees — some people even do it to themselves). One type of brain stimulation, called deep brain stimulation or DBS, uses electrodes to apply tiny shocks to areas deep in the brain. When targeted to a specific brain region and carefully calibrated, this can have a profoundly positive effect on treating movement disorders such as Parkinson’s disease. Patients with Parkinson’s disease find it difficult to make smooth movements, and progressively more difficult to initiate movement (for more extensive information on Parkinson’s, visit this website). Patients in the early stages of Parkinson’s disease generally respond well to medication, but as the disease progresses the drugs can become less effective, which is when a deep brain stimulation (DBS) device can be implanted to primarily reduce the amount of drugs required, and thus reduce the side-effects of taking those drugs [2]. Remarkably, when brain stimulation is applied specifically in deep brain regions involved in motor control (usually the subthalamic nucleus or globus pallidus interna) these symptoms can disappear almost entirely and immediately, returning control of movement to the patients. Using advanced brain maps and the known locations of DBS electrodes in patients, scientists are steadily figuring out the best brain areas to stimulate [3]. However, for the treatment to be effective, the device must always be on to constantly apply the tiny shocks. In the videos below, watch for the sudden change in the tremor and the ability to move smoothly when the device is turned on or off.
DBS is also effective at treating the related movement disorders dystonia and essential tremor. Preliminary studies show promise for DBS treatment of obsessive-compulsive disorder and Tourette’s syndrome [4], but mixed results for the treatment of depression. However, the exact mechanism behind how DBS works remains unclear. The prevailing theory is that the tiny shocks interfere with or block the abnormal activity in a brain area (see, interference can be good!). In order to figure out the mechanism, researchers are now using a new type of DBS device to not just stimulate, but also record neural activity with the goal of understanding the abnormal brain activity in these diseases, as well as how exactly the stimulation helps. This is a unique advantage to DBS that no other technology can currently provide.

An example of DBS electrode placement.
Unfortunately, this form of DBS has a major downside: it necessitates seriously invasive brain surgery, which risks infection in the brain or damage to brain structures, potentially leading to loss of brain function, other complications, or even death [5,6]. Needless to say, a non-invasive method that could achieve the same specificity as DBS would be a preferable treatment.

X-ray image of implanted DBS electrodes.
Non-Invasive but Non-Specific
Another common form of therapeutic brain stimulation is non-invasive, but only moderately specific. Transcranial Magnetic Stimulation, or TMS, uses magnetic fields to stimulate electrical activity in the brain without requiring any surgery. However, to produce a strong enough magnetic field, you need a large, expensive machine. Thus patients must come in for periodic treatments, and DBS-style constant stimulation is not an option. While TMS is much more specific (and much less scary and controversial) than electroconvulsive therapy (ECT) — which is still used in extreme cases and essentially induces a seizure in the whole brain — it is unable to stimulate a deep brain region without also affecting much of the brain areas surrounding it. Studies have shown that TMS treatment on prefrontal regions of the brain can effectively alleviate depression, leading to its FDA approval for this application in 2008. How exactly magnetizing the brain relieves depression is still poorly understood, but it is thought to more or less “reset” the systems of the brain and re-establish connections responsible for mood [7]. (For more detail on brain stimulation therapies see this page from the National Institutes of Mental Health)
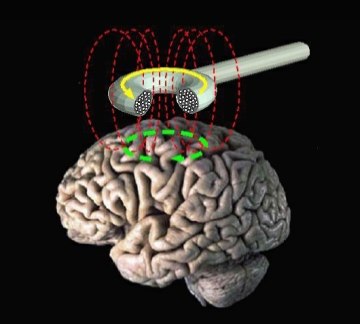
Diagram of the magnetic field produced by a TMS device.
Interference is a common thread in brain stimulation therapies. Regardless of how it is delivered, the stimulation disrupts some badly behaving brain activity, often leading to a positive outcome.
Now bear with me, we’re about to use physics to take interference to a whole new level.
Using physics to take interference to a whole new level
Temporally Interfering Electric Fields, or TEF, is the brand new brain stimulation technique recently published in Cell [1]. It is non-invasive, only requiring placement of electrodes on the outside of the head, and specific enough to activate a single deep brain area. How can it do this when the electric field has to pass through all that brain matter? Maybe you already guessed it…the answer is interference. Specifically, it has to do with how electric fields, or any kind of fields or waves, interfere with each other.

The top wave equals the sum of the two lower waves. Left, constructive interference; right, destructive interference.
In physics, interference refers to when two or more different waves combine to produce a combined wave that could have a higher (constructive interference) or lower (destructive interference) amplitude or intensity. When two waves with different frequencies combine, they produce an interference pattern that changes between constructive and destructive interference at a rate equal to the difference between their frequencies.

Animation of how the interference pattern and beat frequency (blue wave) emerges when the frequency of one wave (green) changes.
When applied to sound frequencies, you can hear this as a slow modulation in the amplitude of the sound. For example, if two trumpets play concert A, which should oscillate 440 times a second or 440Hz, but one trumpet is slightly out of tune at 442Hz, you would hear an unpleasant “wobble” that is actually the volume of the sound modulating at 442-440=2Hz, or twice per second. This is called a “beat frequency” — the wobble you hear is the beat. You can see and hear the phenomenon in this video:
All of this applies to brain stimulation because neurons can only “hear”, or respond to, certain frequencies of electric fields, much like how we can only hear a certain range of sound frequencies. If an electric field oscillates too fast, the electrical properties of neurons cannot keep up and there will be no effect. However, when two electric fields with slightly different frequencies interfere with each other, they produce a beat frequency that a neuron will be able to respond to.
To understand how TEF gets specificity, we also have to consider the shape of electric fields in three dimensions because electric fields will only constructively interfere if they line up correctly. Therefore, the beat frequency will only be felt by neurons in the area where the two electric fields align — everywhere else will only be exposed to the higher frequencies and be (theoretically) unaffected. Furthermore, the location of stimulation can be shifted by simply changing the amount of current sent through the electrodes on either side: increasing current on one side pushes the stimulation location toward the opposite side.

How waves interfere in two dimensions. Color indicates amplitude: red is high and blue is low.
The authors of the paper tested this technology in rodents in two important ways. First, they showed that they were able to increase the activity of neurons specifically in the hippocampus, a relatively deep brain region, without affecting other brain areas. Second, they targeted brain motor areas in anesthetized mice, and were able to initiate movements in different body parts depending on the specific focus of the stimulation. The movements corresponded to how different parts of the motor cortex control the movement of specific body parts, thus providing evidence that the stimulation can be specific, and its location can be shifted effectvely. Much more work needs to be done to determine the capabilities and side effects of Temporally Interfering Electric Fields — such as whether long term exposure to high frequency electric fields can have unforeseen effects — but overall TEF appears very promising.
And the Beat (Frequency) goes on
TEF is not the only new technology that could someday be used to treat brain diseases in humans. Others include using light (optogenetics), sound (ultrasound), or specially designed drugs and receptors (DREADDs). Optogenetics and DREADDs have the potential to be incredibly specific, down to the level of particular types of brain cells, but would likely require very invasive techniques (injecting viruses into the brain, yes really). For now, TEF appears to be just the right balance of specificity and non-invasiveness that you want in your brain stimulation, but one important drawback for the time being is that it can only stimulate the brain. If the new efforts to understand abnormal neural activity recorded from DBS devices are successful and further experiments confirm the safety and effectiveness of TEF, it would have a considerable positive impact on treating severe Parkinsons disease, other movement disorders, and perhaps major neurological disorders such as depression.
Instead of feeling major brain surgery, hopefully someday soon these patients will be feeling the Beat (Frequency).
References
- Grossman, N., Bono, D., Dedic, N., Kodandaramaiah, S. B., Rudenko, A., Suk, H.-J., … Boyden, E. S. (2017). Noninvasive Deep Brain Stimulation via Temporally Interfering Electric Fields. Cell, 169(6), 1029–1041.e16. doi.org/10.1016/j.cell.2017.05.024
- Almeida, L., Deeb, W., Spears, C., Opri, E., Molina, R., Martinez-ramirez, D., … Okun, M. S. (2017). Current Practice and the Future of Deep Brain Stimulation Therapy in Parkinson’s Disease. Semin Neurol 2017;37:205–214. doi.org/10.1055/s-0037-1601893
- Horn, A., Reich, M., Vorwerk, J., Li, N., Wenzel, G., Fang, Q., Schmitz-Hübsch, T., Nickl, R., Kupsch, A., Volkmann, J., Kühn, A. A. and Fox, M. D. (2017), Connectivity predicts deep brain stimulation outcome in Parkinson’s disease. Ann Neurol.. Accepted Author Manuscript. doi.org/10.1002/ana.24974
- Welter, M., Houeto, J., Thobois, S., Bataille, B., Guenot, M., Worbe, Y., … Czernecki, V. (2017). Anterior pallidal deep brain stimulation for Tourette’s syndrome : a randomised , double-blind , controlled trial. 4422(17), 1–10. doi.org/10.1016/S1474-4422(17)30160-6
- Fernández-Pajarín, G., Sesar, A., Ares, B. et al. Acta Neurochir (2017). Delayed complications of deep brain stimulation: 16-year experience in 249 patients. doi.org/10.1007/s00701-017-3252-7
- Jing Zhang, Tao Wang, Chen-cheng Zhang, Kristina Zeljic, Shikun Zhan, Bo-min Sun, Dian-you Li (2016). The safety issues and hardware-related complications of deep brain stimulation therapy: a single-center retrospective analysis of 478 patients with Parkinson’s disease. doi.org/10.2147/CIA.S130882
- Anderson, R. J., Hoy, K. E., Daskalakis, Z. J., & Fitzgerald, P. B. (2016). Clinical Neurophysiology Repetitive transcranial magnetic stimulation for treatment resistant depression : Re-establishing connections. Clinical Neurophysiology, 127(11), 3394–3405. doi.org/10.1016/j.clinph.2016.08.015

You must be logged in to post a comment.