 August
25
August
25
Tags
An Appetite for Epilepsy
Have you ever wondered what really makes up your body? Well, even if you haven’t, you’ll be surprised to know that there are trillions of microorganisms living inside you, so many that they outnumber your actual body cells 10 to 1: for every one of your cells, there are 10 microorganisms. That’s right, you’ve got other organisms living inside you. In recent years, special attention has been paid to the organisms living in your gut. These tiny organisms in your gut have been of special interest to the scientific community over the past decade or so. There are many reasons that scientists, biotech companies, and pharmaceutical companies, among others, are so interested in learning about and understanding all that lives down there. Your gut microbiome health is starting to show promise in helping a variety of diseases and disorders, such as liver diseases, inflammatory bowel diseases (IBD), heart problems, obesity, diabetes, depression, and many others. However, of special interest to us is the possible benefits of harnessing the gut microbiome to help treat those with intractable epilepsy, which is epilepsy that is resistant to conventional methods of preventing seizures, such as antiepileptic drugs.
Research in the last couple of years has found promise in harnessing the gut microbiome to help lower the likelihood of seizures, and substantially so. A groundbreaking paper cited almost ubiquitously in the research using the gut microbiome to treat epilepsy, is that of Dr. Christine Olson and colleagues. To briefly summarize this paper, the authors used a mouse model of epilepsy where the mice were given a strict ketogenic diet consisting of a high intake of healthy fats, and low consumption of carbohydrates. When this diet was combined with a healthy gut microbiome, the mice had a substantially lowered frequency of seizures. This paper is critical to understanding the connection between the gut and the brain because it shows us that diet can easily influence our brain.
The gut microbiome and the gut-brain axis
Prior to discussing the impact of these findings, we must appreciate the complexity of the gut microbiome and its connection to the brain. Little organisms, known as microbes, live inside your body–especially in your gastrointestinal tract (stomach and intestines). These organisms are what make up the gut microbiome. The microbes specifically in your gut microbiome are aptly named gut microbiota. These gut microbiota play an important part in a whole range of functions, which includes performing various metabolic functions and keeping you healthy by protecting you from nefarious bacteria and viruses. Currently being studied is their role in protecting against neurological diseases like depression, epilepsy, and amyotrophic lateral sclerosis (which you might know as ALS, broadly recognized as the disease Stephen Hawking had, and the origin of the “ice bucket challenge” trend). The effects that the gut microbiome has on our brain and neurologic health are mediated through what is known as the gut-brain axis, defined by Jeremy Appleton (2018) as “a bidirectional communication network that links the enteric [gut] and central nervous systems…not only anatomical, but it extends to include endocrine, humoral, metabolic, and immune routes of communication as well.”
A major way that the gut influences the brain indirectly is by the production of neurotransmitters, the chemicals used by neurons to communicate and transmit signals. The production of these various neurotransmitters is one way by which the gut microbiota influences the brain’s health and potentially confers protection against various diseases.
The gut-brain axis and important neurotransmitters for understanding epilepsy
Two important neurotransmitters, glutamate and gamma-aminobutyric acid (GABA), are produced by the gut microbiome. These neurotransmitters are also important to understanding the gut’s role in seizure protection. To put it briefly, studies (Meira et al. 2019) into the keto diet and its role in epilepsy treatment found that there seemed to be increased levels of GABA in the brains of those patients on the keto diet. Now, I must digress into explaining the roles of Glutamate and GABA so we can understand why this is important to understand how the keto diet helps with seizure protection.
Glutamate and GABA are the body’s major excitatory and inhibitory neurotransmitters, respectively, and thus have antagonistic (opposite) effects on the brain. Disorders and diseases that are a result of an imbalance of these two neurotransmitters usually can be ameliorated by supplying more of the neurotransmitter that is lessened. For instance, some forms of epilepsy can result in an imbalance of the Glutamate/GABA ratio, where the ratio is biased towards the glutamate side. If we consider that epilepsy is overexcitation of the brain, meaning that there are too many neurons sending excitatory signals at the same time, knowing that epilepsy can be triggered by heightened levels of glutamate, an excitatory neurotransmitter, it follows that providing more GABA to the system of a patient with epilepsy would help to reduce their chance of having a seizure. And that is just what has been found; numerous studies have linked increased levels of GABA to antiepileptic effects.
Since your gut is composed of both your stomach and your intestines, your diet impacts the microbiome substantially, hence how your diet can influence your brain health. Since the paper we will be looking at discusses how the keto diet works with your gut to confer seizure protection, I will discuss how the keto diet impacts your gut microbiome and what downstream effects it has been shown to produce.
The keto diet and the gut microbiome
The keto diet is a high-fat, low-carb diet. Some foods it consists of are meats, cheeses, nuts and seeds, eggs, fatty fish, butter, and cream. On the flip side, foods that are high in carbohydrates such as any sugary food, bread, and other grain/wheat-based products, most fruits, and beans shouldn’t be eaten on the keto diet. (Mawer 2020). If you love Mexican food, like I do since I am a born and raised San Diegan, this diet would be really hard to stick to.
The Olson et al. (2018) paper found that, among other things, the keto diet significantly and rapidly alters the composition of the gut microbiome. Many bacteria species populations are increased, showing that something in the keto diet helps to nourish these bacteria. So, whatever it is that the keto diet brings to the gut to nourish it, it may be the reason why the keto diet works to confer seizure protection but only with an intact gut microbiome.
Turning back to the keto diet and Glutamate/GABA concentrations, the study mentioned above (Meira et al. 2019) found that GABA concentrations in the brains of patients on the keto diet were elevated, as mentioned before. Why is this? Well, the study tells us that the keto diet promotes certain enzymes that lead to the production of GABA. Since GABA has already been shown to produce an antiepileptic effect (reduce seizures), we can conclude that the keto diet helps to reduce seizures because it increases GABA production. However, since your diet affects and interacts with your gut microbiome, the keto diet is necessary but not sufficient for increased GABA production.
The antiepileptic effects of the gut microbiome and the keto diet
A very important piece to the puzzle concerning the use of the gut microbiome to treat epilepsy was uncovered by researchers Olson et al. (2018), who in a monumental study tested the efficacy of using the keto diet to treat epilepsy, in conjunction with a healthy gut microbiome. It is important to note a key concept here: necessary but not sufficient. A healthy gut microbiome is necessary to aid in seizure protection, as well as the keto diet, but by themselves are not sufficient. What this means is that neither of them alone confers seizure protection, but together, they do.
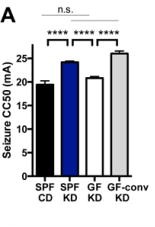
But how do we know that we also need a healthy gut microbiome, and the keto diet isn’t sufficient for seizure protection by itself? That’s where understanding the figure to the left can help us. In this figure, the graph tracks differences in seizure threshold between those on the keto diet vs control diet and those with a healthy microbiome vs those without one. We see dramatically increased seizure thresholds in both groups with a healthy gut microbiome and fed the keto diet (bar 2 and 4, acronyms are listed in the table on the left). If all that was needed was the KD, all of the mice on the KD would have relatively equal, elevated seizure thresholds. However, only the mice with an intact gut microbiome and being fed the KD at the same time (SPF KD and GF-conv KD) were able to reap the benefits. Hence, necessary but not sufficient.
Biotherapeutic potentials
With the revelations of this study, a large body of research was born, which investigates the gut microbiome’s benefits and its therapeutic potential. Both academic institutions and biotech companies want to uncover the mysteries of the gut, and as well the gut-brain axis. From ALS, to epilepsy, to depression, there are many therapeutic targets that the gut-brain axis has been postulated to be involved in, and pioneering biotech companies are especially joining this new and exciting journey.
References
Appleton J. (2018). The Gut-Brain Axis: Influence of Microbiota on Mood and Mental Health. Integrative medicine (Encinitas, Calif.), 17(4), 28–32.
D’Andrea Meira, I., Romão, T. T., Pires do Prado, H. J., Krüger, L. T., Pires, M., & da Conceição, P. O. (2019). Ketogenic Diet and Epilepsy: What We Know So Far. Frontiers in neuroscience, 13, 5. https://doi.org/10.3389/fnins.2019.00005
Mawer, R. (2020, October 22). The ketogenic diet: A detailed beginner’s guide to keto. Healthline. Retrieved August 24, 2022, from https://www.healthline.com/nutrition/ketogenic-diet-101#sample-plan
Olson, C. A., Vuong, H. E., Yano, J. M., Liang, Q. Y., Nusbaum, D. J., & Hsiao, E. Y. (2018). The Gut Microbiota Mediates the Anti-Seizure Effects of the Ketogenic Diet. Cell, 173(7), 1728–1741.e13. https://doi.org/10.1016/j.cell.2018.04.027



Pingback: An Appetite for Epilepsy – Keto World USA Blog