 January
26
January
26
Tags
Striking and Totally Unexpected
If you would like to learn a little more about how epilepsy affects memory and more about my personal accounts, one of my previous articles, Shaken Memory, also talks about thes things. I consider this current article a revision, however, since I have learned a bit more about my condition.
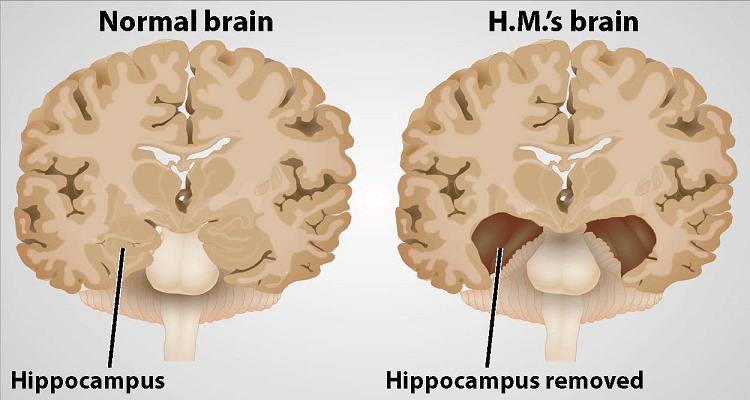
When Brenda Milner and William Scoville (1952) almost completely removed the medial temporal lobe (MTL) of a patient to treat his drug-resistant epilepsy, they did not know there would be a “striking and totally unexpected” memory deficit. However, this is when they discovered that this structure plays a crucial role in memory formation. The man was known as patient H.M. (Henry Moliason), and you are bound to read about his case study in any introductory neuroscience or psychology course.
Following the surgery, H.M. could barely hold any new information in his mind; in fact, he could only “retain a three-digit number for as long as 15 min by continuous rehearsal, organizing the digits according to an elaborate mnemonic scheme” (2). However, if he was distracted for even a brief period of time, he would completely forget the information. Hence, the researchers were able to come to the conclusion that the MTL was essential to memory formation.
This was an extreme example, but nowadays, there are many treatment options for epilepsy patients who do not respond to medications (some of which are described here and here). Modern technology has also led to much more favorable outcomes in surgery for those whose epilepsy does not respond to medicine or other treatments. With this technology, neurosurgeons have been able to be more cautious when removing any part of the MTL to treat epilepsy. Because of the work that Milner and Scoville did with H.M., I am able to tell you more about what the MTL does; so, let’s start learning!
Medial temporal lobe (MTL)
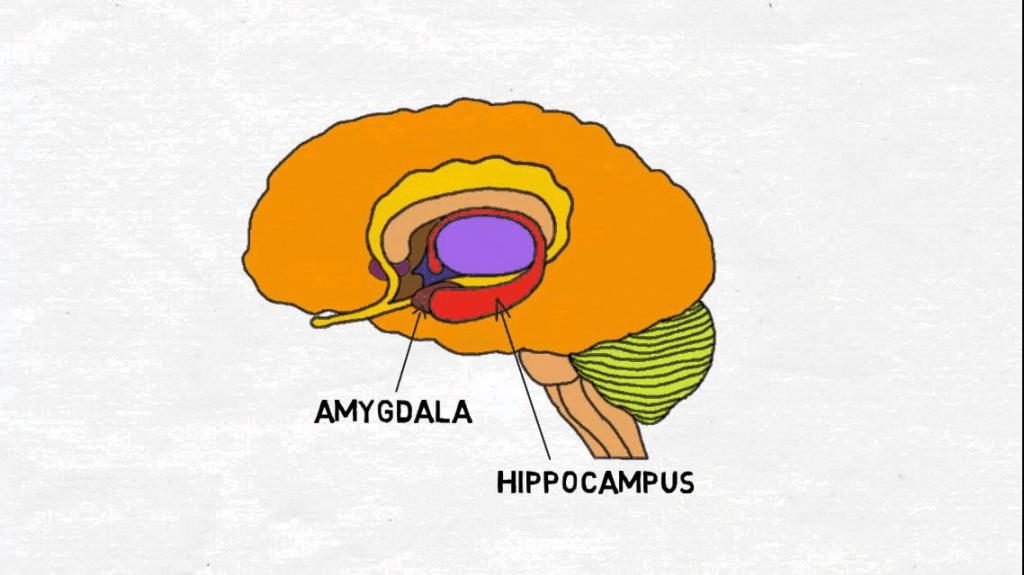
The Medial Temporal Lobe is a collection of structures towards the center of the brain that contribute to memory formation and retrieval, as well as emotional regulation (5). The MTL has different structures responsible for these different processes, and two of the most notable structures are the hippocampus and the amygdala.
The hippocampus is a structure towards the very center of our brain, and its primary function is memory formation. This is aided by the widespread connections that the hippocampus has to other parts of the brain. The hippocampus receives input from many structures that deal with the processing of sensory information, and that allows the hippocampus to form memories of all different types. These processes include spatial memory, visual perception, and perception of space and time. One structure that communicates with the hippocampus is the amygdala, which is also an essential structure in the MTL, However, it does much more than aid in memory formation and retrieval.
The amygdala is located just in front of the hippocampus, and it regulates emotional output. Recently, it has also been found to aid in decision-making, attention, and reward-based associations (such as in operant conditioning), as well as learning. As mentioned before, it interacts with other structures of the MTL, such as the hippocampus, to add an emotional component to our memories. So, even though you may have heard of the amygdala related to fear, it actually is responsible for much more.
Medial Temporal Lobe Epilepsy (MTLE)
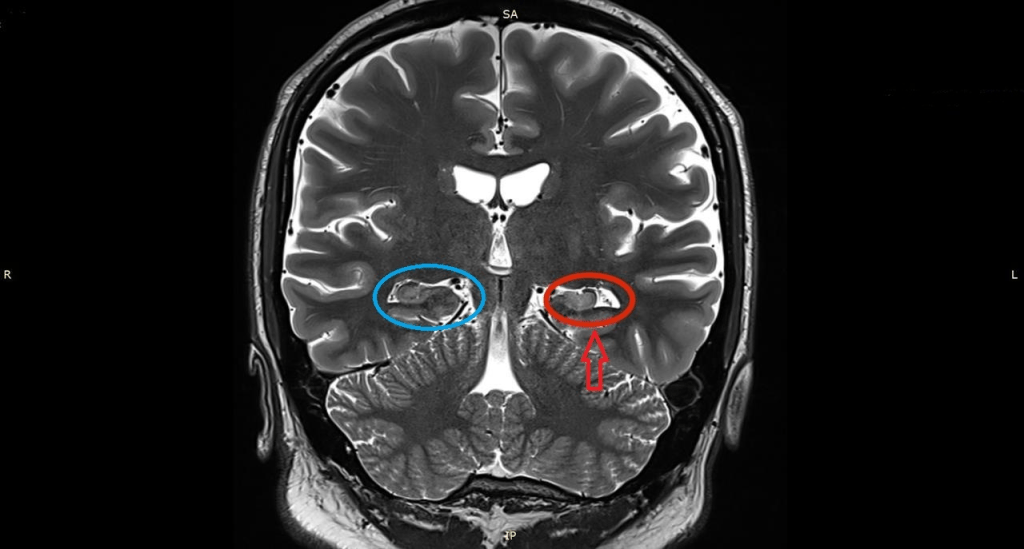
Even though the removal of his MTL cured his seizures, H.M. didn’t actually have Medial Temporal Lobe Epilepsy himself (7). However, MTLE is the most common type of epilepsy, affecting 50 million people worldwide, according to a survey conducted in 2021 (8). That said, MTLE is simply epilepsy where seizures occur in or originate from the MTL. It can consist of many different kinds of seizures, and those recovering from an MTL seizure may experience various memory deficits after the main (ictal) phase of the seizure. This is known as the postictal state, and it can last a few hours or even for weeks afterward (more about seizures and the postictal state in this Neuwrite article and this one). Research has found that epileptic patients with MTLE in the left hemisphere of their brains (like me) generally have verbal memory (memory of facts and information) deficits in this phase, whereas those with MTLE in the right hemisphere have deficits in their visual memory (memory of what objects or symbols look like) (10). These deficits also vary depending on the severity of the seizure and the progression of the disease.
Patients with MTLE who have suffered a seizure may also become depressed or anxious for a few days or even weeks after their seizure. Depression and anxiety occur in the postictal state when the amygdala is affected, and the amygdala can even be activated during the ictal phase of a seizure, leading to emotional reactions such as fear, dreamy states, memory flashbacks, or heart palpitations (11). Furthermore, recent research on the amygdala shows that this may be the reason why epilepsy patients are more likely to have depression and/or anxiety (11): 14% of MTLE patients show evidence of amygdala enlargement (12).
As someone with MTLE in the left hemisphere of my brain, I have experienced verbal memory deficits: following a seizure, I have not been able to remember who I was, what year it was, and one time I didn’t know who my mom was either for about an hour after. I also have no recollection of having the interactions that others told me about (an example of this is in this article). As well, after a seizure in April of 2022, I became really depressed and lethargic for about a week. I was already depressed and anxious at the time, and this only exacerbated it.
Mesial Temporal Sclerosis (MTS)
Sometimes, the MTL becomes injured and/or scarred due to trauma, or even as a result of repeated epileptic seizures. This can then result in a condition known as Mesial Temporal Sclerosis (MTS). You may have heard the term “sclerosis” in names such as “Multiple Sclerosis (MS)” or “Amyotrophic Lateral Sclerosis (ALS)”. Sclerosis means that there is scar tissue that has formed in the brain tissue. As such, Mesial Temporal Sclerosis simply means that scar tissue is present in the MTL.
In fact, MTS is present in 60-70% of patients with MTLE (13). MTLE is the most frequently diagnosed epileptic syndrome in adults (14) because MTS can result from trauma. This is why, for instance, when investigating the cause of a patient’s epilepsy, MRI scans of the MTL are taken in very fine detail to reveal structural abnormalities, such as MTS.
Researchers have also been able to accurately detect seizure onset in most cases of MTLE, originating primarily in the hippocampus, in the form of a condition known as hippocampal sclerosis (15;16). In fact, the MTL is the primary location affected in most cases of epilepsy. Thus, symptoms of MTS overlap with MTLE: muscle spasms or convulsions, behavioral changes, and strange sensations, such as auras or seizures. Most cases of MTS occur as hippocampal sclerosis. In both of these conditions (MTLE and MTS), hippocampal sclerosis is often deemed epileptogenic, or the tissue that results in epileptic seizures.
A closer look at my brain
I suffered a severe traumatic brain injury and was diagnosed with posttraumatic epilepsy early on in my recovery. Recently, however, I decided to see an epileptologist, or a neurologist who specializes in treating patients with epilepsy. Finding it weird that it never came to my mind to see an epileptologist, I decided to do so back in August of 2022 because I was having more frequent seizures. The doctor decided to order MRI scans of my brain; the MRI images showed left-sided MTS, and furthermore MTLE. One of the MRI images that shows the evidence of MTS is shown below.
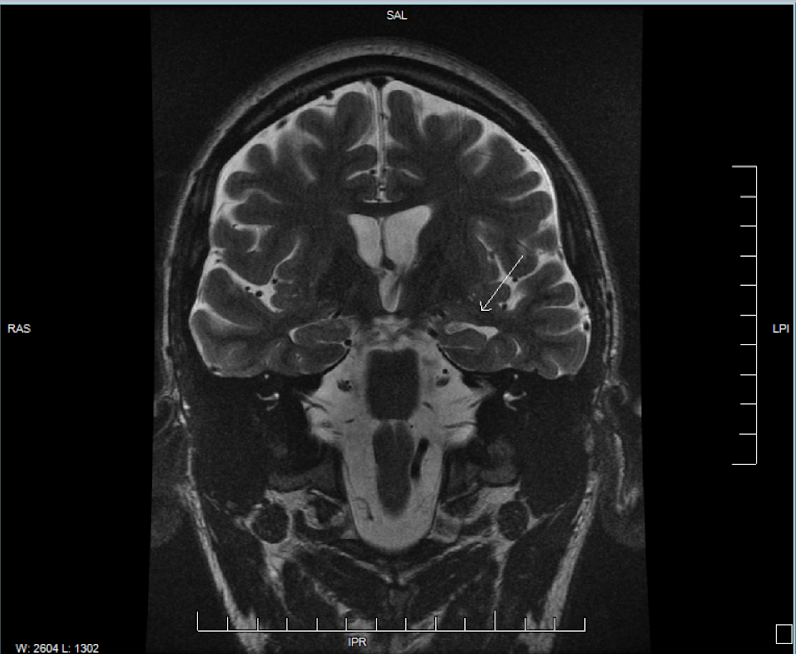
The white tissue that the arrow is pointing to is scar tissue, indicative of left-sided MTS
Although most people with MTS do not have memory deficits as severe as H.M. (like me), with the worsening of MTS, memory deficits may begin to present (17). Therefore, we still need to protect our brains and limit the risks of lowering our seizure threshold (the likelihood of having a seizure: lower threshold, higher likelihood of having a seizure) so our disorder does not progress. This includes getting adequate sleep, remembering to take antiepileptic medications, trying to avoid alcohol (although I know it’s hard to resist a fun night out), and not taking illicit drugs (like cocaine, meth, heroin, etc). If we do not, our condition will worsen, because repeated seizures just create more scar tissue.
Conclusion
Although we know a lot more about memory and emotion than we did half a century ago, we are still finding out more, due to disorders of the structures in the MTL. This all began with the tragic story of H.M., whose memory was severely impacted after the removal of these structures. As well, the disorders we discussed in this article—MTLE and MTS—elucidate other aspects of memory in the brain, or rather, how memory can go awry. A curious fact to me is that the type of memory deficit present after an MTL seizure, verbal or visual, can result from whichever side of the MTL that scarring (MTS) occurs on. As someone with MTLE and MTS following a severe traumatic brain injury, I have one last thing to tell you: please protect your brain.
References
- https://neuwritesd.org/2021/07/22/17677/
- https://www.sciencedirect.com/science/article/pii/S0896627308010957
- https://neuwritesd.org/2022/08/25/an-appetite-for-epilepsy/
- https://neuwritesd.org/2022/10/13/the-wandering-nerve/
- https://www.scienceabc.com/pure-sciences/the-medial-temporal-lobe-structure-and-functions.html
- https://en.wikipedia.org/wiki/Operant_conditioning
- https://www.brainfacts.org/in-the-lab/tools-and-techniques/2018/the-curious-case-of-patient-hm-082818
- https://www.ncbi.nlm.nih.gov/books/NBK549852/
- https://neuwritesd.org/2022/11/17/a-series-of-exciting-events/
- https://www.statpearls.com/ArticleLibrary/viewarticle/28844
- https://onlinelibrary.wiley.com/doi/10.1002/jnr.23689
- https://www.frontiersin.org/articles/10.3389/fneur.2013.00166/full
- https://www.scielo.br/j/jecn/a/PLYYrJ8RxqBWjPgCDzMbsHx/?lang=en#:~:text=Mesial%20temporal%20lobe%20sclerosis%20(MTS,distinct%20hippocampal%20pathology%20remains%20undetermined.
- https://www.thelancet.com/article/S2352-3964(18)30067-7/fulltext
- https://pubmed.ncbi.nlm.nih.gov/25727907/
- https://pubmed.ncbi.nlm.nih.gov/15101831/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5873595/



You must be logged in to post a comment.