 March
02
March
02
Tags
Mindfulness as a treatment for anxiety
Anxiety disorders, not to be confused with occasional feelings of anxiety, are the most common category of mental disorders around the world, and carry significant burdens of distress and impairment for those suffering from them. These include generalized anxiety disorder, social anxiety disorder, panic disorder, and phobia-related disorders. While effective anxiety disorder treatments exist, such as medications and psychotherapy, many people face barriers in accessing them. These barriers may be financial, logistical, or due to lack of awareness and/or stigma. According to the Centers for Disease Control and Prevention’s 2022 National Health Statistics Report, only 62.9-66.7% of those in the US who reported having severe anxiety symptoms received mental health treatment [1]. Further, among those who do seek help, not everyone benefits from existing treatment options. For instance, medications aren’t effective for everyone who tries them, as they treat symptoms rather than the causes of anxiety (which we still understand poorly). Clearly, there is an ongoing need for more widely-accessible, evidence-based anxiety treatments. Recently, researchers and clinicians alike have had their eyes on mindfulness as a potential remedy.
What is Mindfulness?
One of my favorite descriptions of mindfulness comes from Jack Kornfield, an internationally known meditation teacher:
“Mindfulness is paying attention to what is happening inside and outside you in the present moment. This begins with something that is incredibly simple: A pause. Imagine being in a movie theater, immersed in a fast-paced thriller. Suddenly, the screen freezes. No longer swept away in the action, you become aware of where you are, the people around you, aware of the pulsing tension in your body, of what you’re thinking and feeling. You are in the midst of a pause. Learning to pause in the midst of your life brings you back to what’s actually happening. You’re not caught up in the movie, and in that space, you can see more clearly what you are thinking and feeling and what is going on around you.”
This analogy gets at the heart of mindfulness and why it’s so challenging. It’s too easy to become so swept away with our daily activities that we neglect to check in with how we are feeling – both physically and emotionally. Have you ever spent time engaged in a task, perhaps hard at work on your computer, and you suddenly realize that your shoulders are aching from being tensed or hunched over for so long? Or, in a moment of conflict, have you responded to someone you care about in a way that was hurtful because you yourself were hurting, but you couldn’t recognize it until later? It’s practically effortless to become mentally disconnected from our bodies and even our emotions when we are caught up in the movie that is life, and this can have unfortunate consequences.
Mindfulness is a broad category of activities that can help us reconnect our minds and bodies, and become more of an observer of our thoughts and feelings rather than being consumed by them. Perhaps meditation is one of the first things that comes to mind. Some other ways of practicing mindfulness could be creative activities like art and music, exercise, spiritualism, journaling, and breathing practices. Really, any activity that takes you out of contemplating the past or worrying about the future, and keeps you grounded in the present, is a mindful activity.
Previous NeuWriters have written about the neuroscience of mindfulness and how it relates to our well-being [2-4]. Generally speaking, the research evidence is positive when it comes to the benefits of a mindfulness practice. It can change our brain activity in ways that may facilitate emotional processing [5] and help with pain management [6]. Additionally, previous research based on self-reports has suggested that mindfulness can help us manage symptoms of anxiety and depression [7]. However, for multiple reasons, it has been challenging to study mindfulness in a way that would allow direct comparison to other treatments, such as medication. This is partly due to the fact that there are countless ways to practice mindfulness, so without a standardized approach it has been difficult to attribute any benefits to a single cause. Fortunately, a structured mindfulness course exists called Mindfulness-Based Stress Reduction (MBSR), and over time it has become more widely-researched than any other mindfulness-based intervention, making it an appropriate target for a clinical trial.
Mindfulness-Based Stress Reduction
Dr. Elizabeth Hoge and colleagues recently published the results of the first clinical trial directly assessing the effectiveness of a standardized, evidence-based mindfulness practice for treating anxiety disorders [8]. MBSR is an 8-week structured course developed in the 1970s by Dr. Jon Kabat-Zinn that combines Buddhist teachings with secular western medical approaches. The course consists of weekly 2.5 hour-long meetings, 45 minutes of daily homework, and a day-long retreat between the 6th and 7th week. Throughout the course, students are instructed in three general techniques: mindfulness meditation (generally focusing on the breath for a length of time), body scanning (a meditative practice that involves mentally scanning through the body to bring attention and awareness to sensations to each area), and simple yoga positions (focusing especially on mind-body awareness). While MBSR and related practices have grown in popularity and shown promise in reducing anxiety, the authors wanted to directly compare the standardized course with a commonly prescribed anxiety medication – escitalopram (AKA lexapro).
TAME Trial
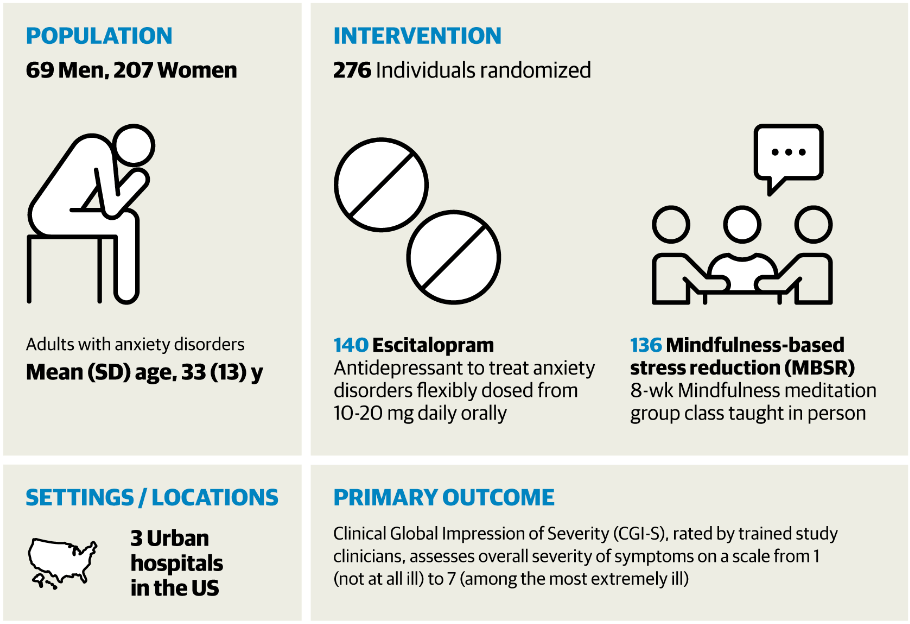
In this clinical trial, called Treatments for Anxiety: Meditation and Escitalopram (TAME), 276 adults diagnosed with an anxiety disorder were recruited and randomly assigned to either 8 weeks of the MBSR course or 10-20mg of escitalopram. Due to some people dropping out of the study and/or not completing the medication treatment or MBSR course, the final sample consisted of 208 people.
The research team was primarily interested in seeing whether the intensity of anxiety symptoms among those in the MBSR course would show similar improvements to those taking medication. They did this using the Clinical Global Impression of Severity scale (CGI-S), which is a simple and non-specific tool for measuring a psychiatric patient’s functioning over the course of a treatment. It consists of a single question answered by a clinician: “Considering your total clinical experience with this particular population, how mentally ill is the patient at this time?” This is answered on a 7-point scale: 1=normal, not at all ill; 2=borderline mentally ill; 3=mildly ill; 4=moderately ill; 5=markedly ill; 6=severely ill; 7=among the most extremely ill patients. The clinician decides upon this rating based on discussions with the patient, including both what they observe and what the patient tells them about their symptoms, behavior, and overall functioning in the past week. At the start of the trial, the average severity across all participants was in the moderate to markedly ill range (4-5).
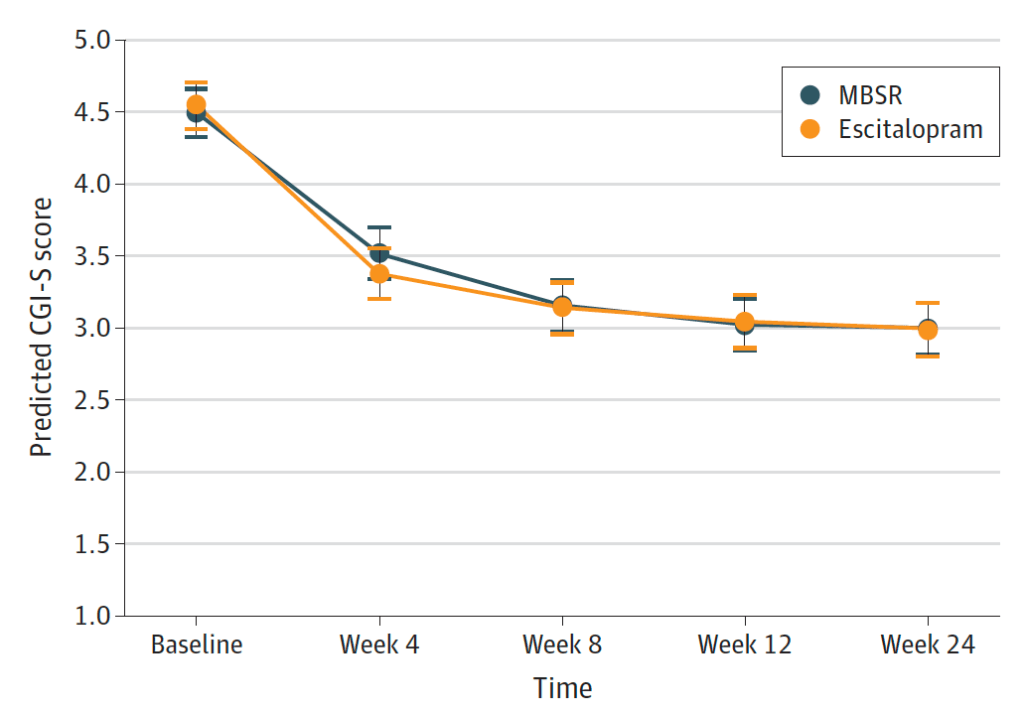
Both the MBSR and medication treatment groups showed improvement in anxiety symptoms. The greatest change occurred early on in the trial; by week 4, the average of both groups’ CGI-S scores transitioned from the moderately-markedly ill range (4-5) into the mildly-moderately ill (3-4) range. By week 8, there was a further (albeit less drastic) reduction in symptom severity. The difference between the CGI-S score between groups was not statistically significant, suggesting similar clinical benefits. Interestingly, the research team also followed up with participants at 12 and 24 weeks after the start of the trial, and those that had kept up with their treatment continued to show improvements, leveling off around the bottom of the mildly ill (3) range.
When looking at the effectiveness of potential new health treatments, it’s important to consider any so-called adverse events across groups. These are unwanted/unpleasant outcomes or side effects that are judged to be possibly or definitely related to the given treatment. Adverse events are fairly common with medications, but less is known about unwanted side effects of mindfulness practice. At the risk of sounding like a pharmaceutical advertisement, adverse events that were reported in 5% or more of participants in the medication group included sleep disturbance, drowsiness, nausea, fatigue, headache, delayed orgasm, decreased libido, abnormal dreaming, decreased appetite, jitteriness, dizziness, increased sweating, and increased anxiety. In the MBSR group, the only adverse event that affected 5% or more of participants was increased anxiety. Thus, for patients who experience unacceptable levels of side effects from escitalopram, it’s possible that mindfulness is a feasible alternative treatment option.
Medication vs Mindfulness: What Now?
This recent clinical trial showed that completing a MBSR course, which consisted of weekly classes and daily meditation practice, was an effective treatment for clinically diagnosed anxiety disorders. Importantly, it was shown to be as effective as a commonly prescribed anxiety medication. This is not to say that people do not need or should not try medication as a treatment – rather, there are pros and cons to both, and now patients will have another evidence-backed option to consider when deciding how they want to move forward. There are many people with anxiety disorders who don’t respond well to medication, don’t have access to medication, or are uncomfortable seeking care in a psychiatric setting. On the other hand, it’s important to note that a routine mindfulness practice comes with a considerable time and effort commitment, which not everyone has the time and energy to keep up with. Further, there is no reason why someone couldn’t choose to try both options simultaneously, and examining the joint effectiveness of mindfulness and medication would be a logical next step after this trial.
There are important limitations of this trial to acknowledge. Recruitment for the study happened at three urban academic medical centers, which limits sample diversity; participants consisted of mostly women (75%), mostly white people (60% compared to 18% Asian, 14% Black, and 7% other), and most participants were highly educated. This may limit how generalizable these findings are to less represented groups of people, and follow-up studies within these groups are warranted. They also did not collect data on whether or not participants’ anxiety disorders were chronic, which could impact the way they respond to treatment. Nonetheless, this trial is a good first step in demonstrating that a mindfulness regimen may be an effective alternative treatment for those able and willing to give it a try.
Interested in trying MBSR?
While MBSR courses are internationally available in academic and health centers, they generally come with a cost. However, if you are interested in trying MBSR on your own time, a completely free and online version is available here. This course was developed by Dr. Dave Potter, a fully certified MBSR instructor with 12 years of experience teaching live, in-person classes. Regardless of where you are and when you take it, there are optional weekly and monthly zoom meetings where you can ask questions and share your experience with other students and practitioners. You can even get a certificate of completion if you follow the course through to the end.
References
[1] Zablotsky B, et al. (2022) Assessing anxiety and depression: A comparison of National Health Interview Survey measures. National Health
Statistics Reports; no 172. Hyattsville, MD: National Center for Health Statistics. DOI: https://dx.doi.org/10.15620/cdc:117491.
[2] https://neuwritesd.org/2019/08/29/the-neuroscience-of-the-breath/
[3] https://neuwritesd.org/2019/04/11/breathe-the-pain-away-mindfulness-and-chronic-pain/
[4] https://neuwritesd.org/2018/10/11/the-neuroscience-of-mindfulness-meditation/
[5] Weng, HY, et al. (2013). Compassion Training Alters Altruism and Neural Responses to Suffering. Psychological Science, 24(7), 1171–1180. https://doi.org/10.1177/0956797612469537
[6] Kabat-Zinn, J et al. (1985) “The clinical use of mindfulness meditation for the self-regulation of chronic pain.” Journal of behavioral medicine vol. 8,2: 163-90. doi:10.1007/BF00845519
[7] Kabat-Zinn, J, et al. (1992). Effectiveness of a meditation-based stress reduction program in the treatment of anxiety disorders. The American journal of psychiatry, 149(7), 936–943. https://doi.org/10.1176/ajp.149.7.936
[8] Hoge EA, et al. (2023) Mindfulness-Based Stress Reduction vs Escitalopram for the Treatment of Adults With Anxiety Disorders: A Randomized Clinical Trial. JAMA Psychiatry, 80(1):13–21. doi:10.1001/jamapsychiatry.2022.3679


You must be logged in to post a comment.