 June
17
June
17
Tags
How Neuroscience Tools Can Help Patients Regain Their Vision
Biomedical scientists, including many neuroscientists, often get into the scientific research game with the goal of seeing a future in which their work can directly impact human health and wellbeing. There is often a disconnect, however, between the long hours in the lab working with cells, rodents, or computers and the eventual future applications of the work. It can be difficult for the public (and admittedly scientists ourselves) to envision what may come of the scientific technologies and breakthroughs occurring today in the laboratory. Therefore, it is really exciting for scientists and non-scientists alike when a commonly used neuroscience laboratory technique has successfully crossed over into the realm of human health.
Vision has evolved to be the dominant sense for humans as compared to other animals that often rely more on other senses like hearing or smelling. For instance, our visual acuity is three times higher than even our furry canine friends at home [1]. For this reason, diseases that cause loss of vision can be extremely difficult for patients to adjust to. Retinitis pigmentosa is a rare disease that is caused by one of many genetic abnormalities that leads to the degeneration of the light-sensitive cells in the retinas at the back of our eyes. This degeneration begins with the loss of night vision, progresses to the loss of peripheral vision, and eventually can lead to near or complete blindness. In one such case, 40 years of living with retinitis pigmentosa left one 58-year-old man with only the ability to detect light (whether it was light or dark in the room, without the ability to see any objects or details). What if I told you that a commonly used tool in neuroscience labs has allowed for the partial restoration of this man’s vision? Before we get there, let’s review how the retina senses light and transmits that information to our brains and some of the many years of work that allowed scientists to achieve this feat of bringing laboratory science to human health.
The Retina
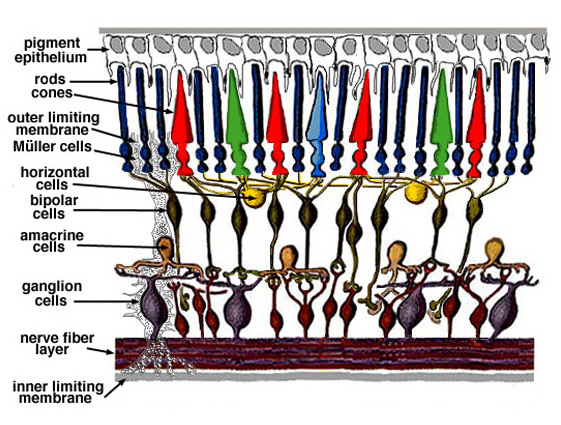
Located on the back surface of our eyes, the retina is the key sensor for light coming into the eyes and translator of that light into nerve activity that can be understood by our brains to form our visual perception. While the structure of the retina and the processes that translate this information are extremely complicated, we can simplify our understanding by looking at which major groups of cells transmit incoming light signals. Photoreceptors, made up of rod and cone cells, are the light-sensitive cells that contain pigments that absorb light and transduce this absorption into signals our nervous system can understand. The symptoms of retinitis pigmentosa are due to the destruction of these photoreceptors (first the rods, then the cones), leaving them insensitive to incoming light. In a healthy retina, photoreceptors signal their light-induced changes to bipolar neurons, which transmit the information to the retinal ganglion cells (RGCs). Importantly, these RGCs are the neurons that make up the optic nerve and send signals first encoded by the eye to the brain.
With this knowledge, we can understand that the problem patients with retinitis pigmentosa face is that the cells in their eyes are no longer sensitive to light. However, the last few decades of neuroscience research have produced interesting tools that may be able to overcome this loss by making neurons sensitive to light by optogenetics.
What is optogenetics?
Optogenetics is the process by which neuroscientists can make innately light-insensitive cells into cells whose activity can be turned on or off by light of certain wavelengths. To achieve this, researchers may use carefully designed and controlled viruses injected into certain parts of the brain of laboratory organisms. Naturally occurring viruses, like the influenza virus or those that cause the common cold, cause illness by entering cells and hijacking the cell’s own protein-making machinery to make copies of themselves. Carefully engineered lab viruses do also make use of the protein machinery of brain cells, but are designed to deliver only the necessary genetic information to, in this case, produce specific types of channels to be expressed in the cell membrane of the neurons of interest.
These special light-sensitive channels are often found naturally occurring across the kingdoms of life: the most famous and widely used example of one of these channels can be found naturally in green algae. Once the neurons of interest are compelled to produce these new channels by viral delivery of the necessary genetic information, light of specific colors from lasers or LEDs can be delivered to them, causing the channels to open. The opening of these channels allows for the flow of ions into or out of the cell, mimicking the function of the many other complex channels that control how neurons communicate with each other. With enough of these special light-sensitive channels, light can be used to turn on (activate) or off (inhibit) the capacity of the neurons to propagate signals with the other cells they communicate with. For more specifics on optogenetics, see these previous NeuWriteSD articles!
Optogenetics has seemingly been employed throughout all of the little corners of the neuroscience field. It is a convenient and powerful tool that can be used to probe the connections of neurons in slices of the brain, and even change the behavior of organisms from worms to rodents in real time (see the images below for an example!). While optogenetics is used in labs every day to study neuroscience outside of vision, what you may now be able to appreciate is that optogenetics might also be a very convenient tool to restore light sensitivity to the cells of the eye if that function were to be lost.


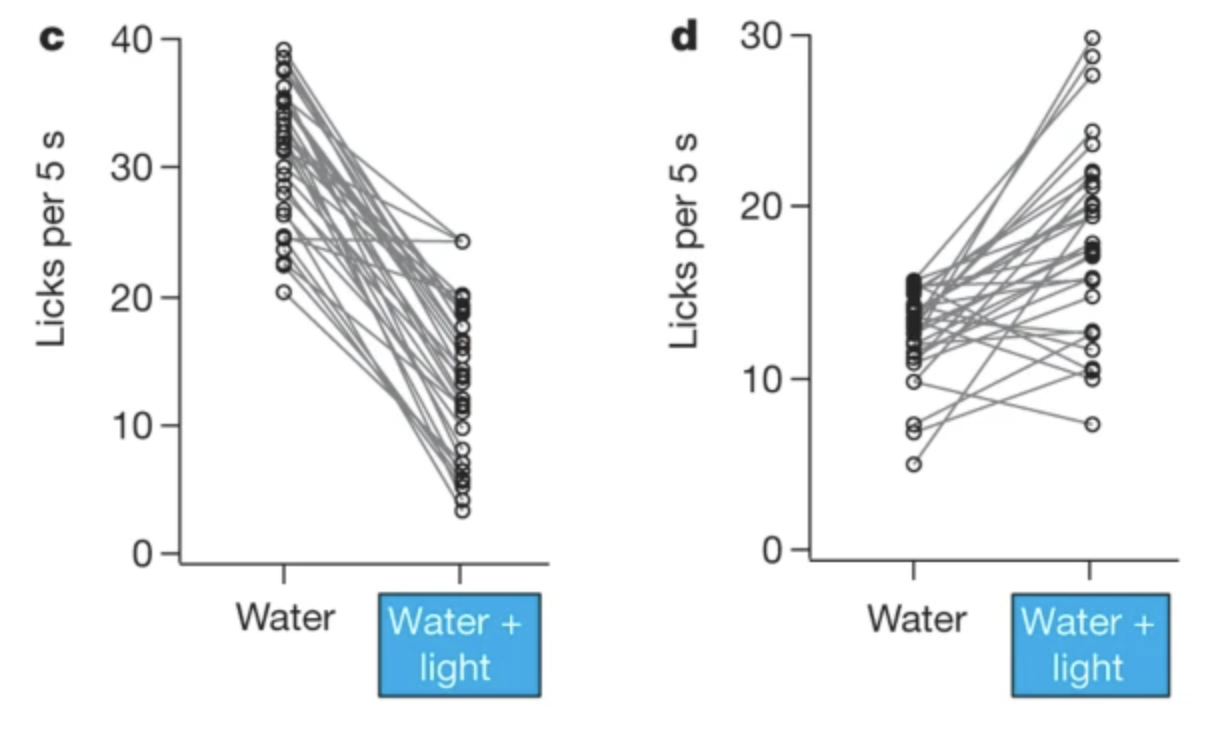
An example of optogenetics being used to control brain activity in the lab [2]. On the left, a thirsty mouse is happily licking at a water delivery spout. In the middle, the mouse reacts to licking at the same water spout after optogenetics is used to activate the part of the brain responsible for “bitter” taste. The closed eyes and grimace indicate that this mouse might be thinking, “yuck!” To the right, a quantification of the number of licks at the spout by the mice reveal that the licking is decreased when the “bitter” portion of the cerebral cortex is turned on (c), indicating that the plain water may have taken on a bitter taste. The opposite is true and licking behavior increases when the light source is in the “sweet” part of the brain (d), perhaps because the water is now perceived as sweet. Although the water being licked at never changes, optogenetic activation of different parts of the brain certainly changes the perception the mouse has of the water!
Optogenetics and Vision in the Lab
Indeed, much work in the laboratory went into testing whether optogenetics could be used to restore light sensitivity in the retina before optogenetics made its way to our 58-year-old retinitis pigmentosa patient (we are getting to him soon!). In the past 15 years, neuroscientists have used optogenetics to reactivate the damaged retinas of mice with similar genetic predispositions to retinitis pigmentosa as human patients. Researchers have added optogenetic light-sensitive channels to the damaged cone photoreceptors [3], the usually light-insensitive intermediate step bipolar neurons [4], and the RGCs that send visual information to the brain [5]. In each case, the researchers showed that the introduction of these channels allowed visual information to once again reach the visual cortex, the part of the brain that processes the light information coming from the eyes to form what we perceive as vision, and improved the rodents’ performance on visual tasks.
The next step in the laboratory process brought optogenetics technology to the retinas of primates, whose eyes are the closest in structure and function to our own in the animal kingdom [6]. A group of researchers from France and the United States used a special type of virus that targets RGCs to introduce an amber light-sensitive channel to the retina, as this color of light is thought to be less likely to damage the eye than the light used to test retinal optogenetics in mice. They found that the virus was well tolerated by the eye and didn’t cause an immune reaction, which is a common response to natural viruses, but can be avoided when using these carefully engineering delivery viruses. They also saw that the introduced channels successfully made the retinas sensitive to specific patterns of light shone upon them. By decoding the response of the retinas to the light, the researchers estimated that the visual acuity using this optogenetics technique could be improved to as good as 20/249, an improvement from the 20/400 rating that defines legal blindness [7].
Can optogenetics be used to treat blindness in humans?

Finally, it’s time to see how these many years of studies in the laboratory have translated to our retinitis pigmentosa patient. In a very recently published case study of one 58-year-old male patient [8], a group of scientists containing many of the same researchers as the primate study attempted to bring their technique to the human eye. The researchers injected the same RGC-targeting virus delivering an amber light-sensitive channel into one of the patient’s eyes. They found that the virus didn’t cause any immune response or change in the patient’s health. In order to deliver enough light to the retina to activate the channels, the researchers also fitted the patient with a special pair of goggles. The goggles use a camera to record from the point of view of the patient and translate that view to monochrome amber light of different intensities that is then projected onto the retina.
While the patient was completely unable to locate or count objects on a table in front of them before the procedure, they were able to locate a large object on the table in 92% of trials and accurately count a small number of objects on the table without touching them with over 50% accuracy after the introduction of the channels into the RGCs. Additionally, the researchers took recordings from electrodes placed on the scalp of the patient during these tasks and found that information specific to the objects in front of them made it all the way to the visual cortex for processing. While these tests occurred in the lab under controlled conditions, the patient also anecdotally shared that with the help of the optogenetic channels and the goggles, they were able to see the bold white lines that make up crosswalks on the street.
The future of optogenetics and vision restoration
The process of bringing tools from the laboratory into therapies for humans is a long one. While these results in the first human patient to undergo this procedure indicate that the use of this technology has room for improvement in restoring vision, they also indicate the astounding reality that our technologies can bring back aspects of vision that many patients thought they would never experience again. With time and hard work, we may be able to look forward to a future in which retinal restoration rivals natural sight with the help of newer and better neuroscience tools.
References
- Lind O, Milton I, Andersson E, Jensen P, Roth LSV (2017) High visual acuity revealed in dogs. PLoS ONE, 12(12):e0188557
- Peng Y, Gillis-Smith S, Jin H, Trankner D, Ryba NJP, Zuker CS (2015) Sweet and bitter taste in the brain of awake behaving animals. Nature, 527:512-515
- Busskamp V, Duebel J, Balya D, et al. (2010) Genetic reactivation of cone photoreceptors restores visual responses in retinitis pigmentosa. Science, 329(5990):413-417
- Lagali PS, Balya D, Awatramani GB, et al. (2008) Light-activated channels targeted to ON bipolar cells restore visual function in retinal degeneration. Nature Neuroscience, 11(6):667-675
- Bi A, Cui J, Ma YP, Olshevskaya E, Pu M, Diszhoor AM, Pan ZH (2006) Ectopic expression of a microbial-type rhodopsin restores visual responses in mice with photoreceptor degeneration. Neuron, 50:23-33
- Picaud S, Dalkara D, Marazova K, Goureau O, Roska B, Sahel J (2019) The primate model for understanding and restoring vision. PNAS, 116(52):26280-26287
- Gauvain G, Akolkar H, Chaffiol A, et al. (2021) Optogenetic therapy: high spatiotemporal resolution and pattern discrimination compatible with vision restoration in non-human primates. Communications Biology, 4(125):1-15\
- Sahel J, Boulanger-Scemama E, Pagot C, et al. (2021) Partial recovery of visual function in a blind patient after optogenetic therapy. Nature Medicine, doi:10.1038/s41591-021-01351-4
Cover Image Source: ROTFLOLEB/Wikimedia Commons/CC BY-SA 3.0

You must be logged in to post a comment.